Last Updated on March 22, 2024
The scaphoid is the most frequently fractured carpal bone. Scaphoid fractures account for up to 15% of acute wrist injuries and 50% to 80% of carpal fractures. Scaphoid fractures have been reported in people aged 10-70 years but commonly occur in young, active individuals, peak incidence being in the second and third decades of life.
Scaphoid fractures are most common following a fall, athletic injury, or motor vehicle accident.
They have a high incidence of nonunion, frequent malunion, wrist instability, and posttraumatic arthritis.
Scaphoid injuries are more common in men than in women.
Most of the scaphoid fractures occur at the waist [see classification] – 65%, proximal third – 25%, and distal third – 10%.
What Are Occult Scaphoid Fractures?
Occult fractures of the scaphoid are the fractures that are suspected clinically but do not show up in the x-rays. Up to 30% of all scaphoid fractures may not be detected on initial x-rays.
If an occult fracture of the scaphoid or severe concomitant wrist injury is suspected but not visible on initial x-rays, the wrist should be immobilized for 10 days in a forearm cast or splint, and the patient should be re-evaluated clinically as well radiologically.
MRI and radionuclide and MRI scans are reliable methods of diagnosing occult fractures of the scaphoid but are expensive investigations.
Anatomy of Scaphoid
The wrist contains eight small bones, which are arranged in two rows, proximal and distal.
The proximal bones, from the radial to the medial side, are the scaphoid, lunate, triquetrum, and pisiform.
The distal bones are, in similar fashion are the trapezium, trapezoid, capitate, and hamate.
Out of proximal four bones, only the scaphoid and lunate articulate with the radius and are responsible for transmission of the entire force of a fall on the hand to the forearm.
Anatomic snuffbox is often used to mark tenderness of the scaphoid injury. It is bordered by the extensor pollicis longus tendon medially, the extensor pollicis brevis and abductor pollicis longus tendons laterally, and the styloid process of the radius proximally.
The scaphoid is Greek for boat and the bone resembles a bent and twisted boat.
The plane of the scaphoid is 450 of palmar tilt to the longitudinal axis of the forearm and 450 radial angulation from the central axis of the forearm on the PA projection.
Major blood supply of scaphoid is a dorsal carpal branch, a branch of the radial artery which enters scaphoid in a nonarticular ridge on the dorsal surface. It supplies proximal 80% of scaphoid via retrograde blood flow.
Minor blood supply from the superficial palmar arch, a branch of the volar radial artery which enters the distal tubercle and supplies distal 20% of the scaphoid.
75% of scaphoid bone is covered by articular cartilage.
The entire proximal half of the scaphoid is an articular surface within the radiocarpal joint. Therefore, the blood supply can enter only on the distal palmar segment and dorsal ridge.
For this reason, proximal-pole fractures require the longest time to union and are associated with a high incidence of osteonecrosis. Approximately one-third of patients have no perforating vessels proximal to the scaphoid waist.
Intrinsic ligaments that attach scaphoid to lunate and distally to the trapezium and trapezoid stabilize the scaphoid.
These ligaments restrict the motion permitting a degree of rotation proximally and a degree of gliding distally.
The scaphoid acts as a link across the midcarpal joint, connecting the proximal and distal carpal rows.
The scaphoid is the key to the carpus because it allows both tremendous mobility of the wrist in flexion/extension and radial/ulnar deviation and provides stability as the intercalated segment linking the proximal and the distal carpal rows.
Both intrinsic and extrinsic ligaments attach and surround the scaphoid allowing the scaphoid to flex with wrist flexion and radial deviation and extend during wrist extension and ulnar deviation.
Much of the wrist motion is a result of the rotation of the scaphoid and the rest of the proximal row during radial and ulnar deviation. The scaphoid rotates to become more vertical, or collinear with the radius, with ulnar deviation bringing the lunate and triquetrum into the dorsal rotation (ie, the distal surface of the bone rotates dorsally).
With radial deviation, the scaphoid rotates to become more horizontal, or perpendicular to the long axis of the radius.
Mechanism of Injury
The scaphoid serves to coordinate and smooth the motions of the proximal and distal rows.
Any shear strain that occurs across the midcarpal joint is transferred through the scaphoid, and may cause fractures and dislocations.
The usual mechanism of injury is a fall onto the outstretched hand (FOOSH) that results in forceful hyperextension of the wrist and impaction of the scaphoid against the dorsal rim of the radius. On getting dorsiflexed >95 degrees, the proximal pole of the scaphoid is tightly held between the capitate, the dorsal lip of the radius, and the taut palmar capsule resulting in fracture of waist. Waist fractures are the type most commonly associated with transscaphoid perilunate fracture-dislocations
Another mechanism is compression injury caused by a longitudinal load or impaction of the wrist. It often leads to fracture of the scaphoid without displacement. When the hand is outstretched and the wrist is in ulnar deviation, the scaphoid is vertical aligned. The axial load combined with the normal palmar curvature of the scaphoid results in a bending moment that collapses the scaphoid. The fracture can involve the scaphoid waist, proximal pole, or the tubercle.
Fractures of the tubercle can be caused by either compression or avulsion.
Proximal pole fractures can be caused by an avulsion of the scapholunate ligament.
In many wrist sprain injuries, the dorsal rim of the radius and the waist of the scaphoid about, resulting in a contusion of the scaphoid and tenderness in the snuffbox.
Snuffbox tenderness is so common in scaphoid injury and considered to be clinical sign suggestive of scaphoid fracture even if the x-rays do not show fracture as the fracture line may be more visible after some resorption [another x-ray at 7-14 days]
Scaphoid fractures in children and the elderly are uncommon. In children, the force causes distal radial physis to fail first and in the elderly, the distal radial metaphysis usually fractures before the scaphoid.
Concomitant distal radius fracture also may occur, particularly radial styloid fractures and dorsal rim fractures, because the line of injury produces a shear fracture of the radius rather than a disruption of the radiocarpal ligaments..
An unstable scaphoid fracture results in a dissociation of the proximal and distal carpal rows and tendency to collapse.
In high energy injuries, other musculoskeletal system parts should be assessed.
Median nerve injuries can occur and can be addressed at the time of surgical treatment. If carpal tunnel develops late, it should be addressed urgently.
Classification of Scaphoid Fractures
Scaphoid fractures have been classified according to various criteria.
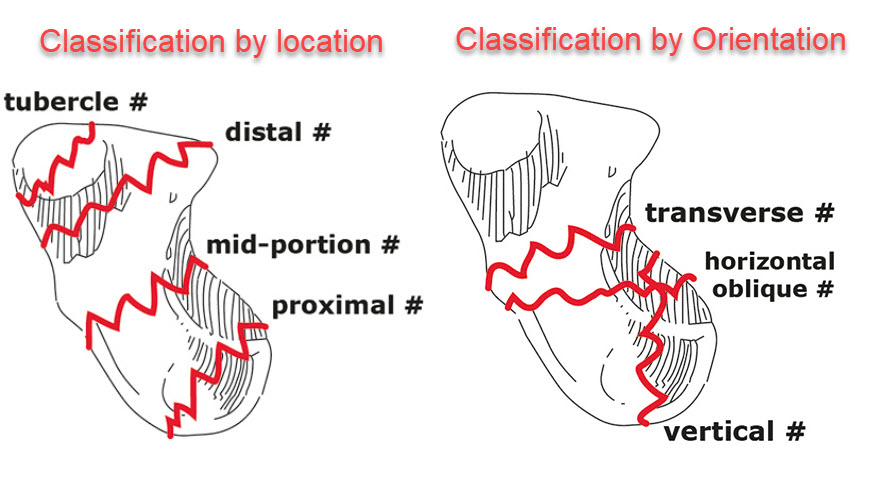
According to Anatomic Location
- Tubercle fractures
- Distal-pole fractures
- Waist Fractures
- Proximal-pole fractures
According to the plane of Fracture
- Horizontal oblique
- Transverse,
- Vertical oblique
According to Stability
Stable Fractures
Incomplete fractures or fractures with the incompletely disrupted articular surface (intact overlying cartilage). Neither displacement nor motion about the fracture occurs with wrist motion. Stable fractures are not associated with ligamentous injury. They are treated with immobilization alone.
Unstable fractures
These are complete fractures with motion about the fracture site.
Findings that indicate instability are
- Cortical offset greater than 1 mm
- Fracture angulation
- Associated ligamentous injury
- Motion with ulnar or radial deviation.
There could be associated ligamentous injury, most frequently involving the scapholunate ligament. It is indicated by widened scapholunate interval may widen, or a DISI pattern
Unstable fractures require fixation.
Herbert and Fisher classification
It is a comprehensive classification and serves as a guide to the treatment of scaphoid fractures. It classifies fractures according to the time of injury and subsequent healing
Type A: Stable Acute Fractures
These are incomplete fractures which unite rapidly with minimal treatment
Type A1
Fracture of tuberosity
Type A2
Incomplete fracture through waist
Type B: Unstable Acute Fractures
These fractures are likely to displace in plaster. Delayed union is common and internal fixation is the treatment of choice
Type B1
Distal oblique fracture
Type B2
Complete fracture of waist
Type B3
Proximal pole fracture
Type B4
Transscaphoid-perilunate fracture dislocation of the carpus
Type B5
Comminuted fractures
Type C
Delayed union- There is a widening of the fracture line, the formation of cysts adjacent to the fracture and proximal fragment becomes relatively dense.
Type D
Established nonunion
The fibrous union can occur after conservative treatment. It is a stable non-union with minimal deformity and variable cystic change. It may progress to pseudarthrosis in time which is hallmarked by unstable progressive deformity and leads to the development of osteoarthritis.
Type D1
Fibrous union
Type D2
Pseudarthrosis
Clinical Presentation
After an acute injury, the patient generally presents with pain and swelling in the wrist. Often there would be a history of falling on the outstretched hand
On examination, there would be tenderness in the snuffbox. For distal pole fractures, a reliable correlation exists with pain provoked by deep palpation at the volar tubercle of the scaphoid, which is the first bony prominence distal to the volar distal radius. For waist fractures, focal tenderness is most often found in the anatomic snuffbox.
For proximal pole fractures, tenderness is often found just distal to the Lister tubercle
An associated swelling may occasionally be noticed. There is a decrease in range of motion and extremes of motion may elicit pain.
It is not uncommon for a fractured scaphoid to go unnoticed. The range of motion may be decreased. Swelling around the radial and posterior aspects of the wrist is common. If
Differential Diagnoses
- Distal Radial Fracture
- De Quervain Tenosynovitis
- Wrist Dislocation
- Ligamentous injury
Imaging
The diagnosis of scaphoid fracture is usually made by x-ray. Following x-rays are done in case of suspected scaphoid fracture for radiological diagnosis.
- Posteroanterior view with the hand in a fist [This puts scaphoid in extension]
- Lateral view
- Radial oblique view
- Ulnar oblique view
Scaphoid View
The patient with a scaphoid fracture often holds the wrist in radial deviation, thereby shortening the scaphoid and limiting its evaluation.
To elongate, the scaphoid view is often obtained by positioning the wrist in ulnar deviation and angling the tube cranially by 20-40.
If required comparative views of the opposite uninjured wrist can be done.
In spite of this, undisplaced scaphoid fractures may not be visible on the initial set of x-rays.
Sometimes the presentation is delayed and depending upon the period since the injury, late presentation of a fracture or an established nonunion may show resorption at the fracture site, subchondral sclerosis, and displacement may occur.
Fractures of the distal radius, perilunate dislocation may occur be associated.
There is almost always a ligament damage that accompanies this injury.
Scaphoid Series Xrays
Scaphoid series is a series of x-rays which can be filmed when there is a clinical evidence of scaphoid fracture but the lesion is not visible on routine projections.
Scaphoid series is helpful for better visualization of the scaphoid and other carpal and improves exposure of the intercarpal joint spaces.
Scaphoid series consists of a sequence of the following four radiographs-
- Wrist hyperextended and in ulnar deviation with the fist clenched and the thumb extended.
- 15° supination view.
- 15° pronation view.
- Lateral view in a neutral position
For negative x-rays in case of suspected scaphoid fracture.
A scaphoid cast is applied x-rays are repeated after 10-14 days. For earlier confirmation MRI, CT, or bone scan may be done.
In case of an athlete who wants to return to competition without waiting 7-14 days for repeated radiographs, a bone scan may be obtained after 72 hours.
Bone scanning – Sensitivity 99%, specificity of 86%
- MRI sensitivity 88% and a specificity of 100%,
- Bone scanning sensitivity 72% and a specificity of 99%
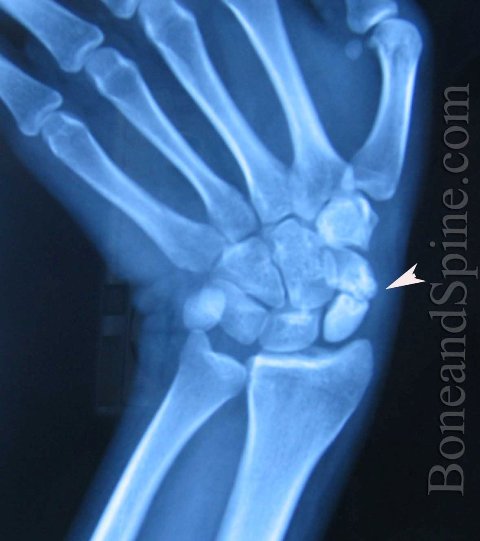
Fracture is typically visible as a lucent line with at least 1 disrupted cortex. In overriding fragments, a stress fracture, or fracture healing a radiopaque line may be seen.
Angulation of the scaphoid or separate fracture fragments may be observed
Small avulsions and incomplete horizontal-oblique or distal-pole fractures are more difficult to detect
Angulation of the scaphoid at the fracture is often called the humpback deformity and is associated with a greater likelihood of nonunion, worse clinical outcome, and arthritis.
Determination of the intrascaphoid angle on a tomographic image may reveal angulation.
A comparative view of the opposite wrist may aid in confirmation or rule out a finding.
Nuclear Imaging
Radionuclide bone scanning is typically performed 3-7 days after the initial injury if the radiographic findings are normal. Intense, focal tracer accumulation is considered a positive finding.
Bone contusions, degenerative disease, intraosseous ganglion, or active process cause increased activity within the scaphoid.
MRI
MRI is is noninvasive and readily available, and it can assess bone healing and evaluate bone contusions and ligamentous injuries.
CT
Its sensitivity and specificity are estimated to be 100% when used 5-10 days postinjury. It is better in delineating the injury and identified small avulsions too. Intrascaphoid angle can be easily calculated.CT scan is helpful for evaluation of union
Treatment of Scaphoid Fractures
When displacement occurs about the scaphoid fracture, ligamentous injury and instability should be suspected.
The most common carpal instability pattern is scapholunate dissociation. It is frequently the first radiographic sign to suggest instability.
Recognition of carpal instability is important and helpful in treatment planning.
Nonoperative Treatment
Thumb spica cast immobilization
This is done in the stable nondisplaced fracture. This would constitute the majority of scaphoid fractures. if the patient has normal xrays but there is a high level of suspicion can immobilize in thumb spica and reevaluate in 12 to 14 days.
Beoth long arm spica and short arm casting is advised by different authors and there is no consensus yet.
Duration of casting depends on the location of the fracture
- Distal-waist for 3 months
- Mid-waist for 4 months
- Proximal third for 5 months
Athletes should not return to play until imaging shows a healed fracture
Augmentation with the pulsed electromagnetic field has been found to be beneficial in a delayed union.
With conservative treatment, scaphoid fractures with <1mm displacement have a union rate of 90%.
Operative Treatment
This involves the reduction and fixation of the fracture. This could be an open reduction and internal fixation or closed reduction and percutaneous screw fixation.
This treatment is indicated in unstable fractures as seen by
- Proximal pole fractures
- Displacement > 1 mm
- 15° scaphoid humpback deformity/ intrascaphoid angle of > 35°
- Radiolunate angle > 15° (DISI)
- Associated with scapholunate ligament disruption/ carpal instability/perilunate dislocation
- Comminuted fractures
- Unstable vertical or oblique fractures
Other factors for consideration of surgical treatment are
- Early return is desired in cases of nondisplaced fracture
- Delayed presentation of acute fracture
- Carpal instability (lunate tilt on radiograph)
- Evidence of nonunion or osteonecrosis
The fractures are fixed by smooth Kirschner wires or a Herbert screw. Dorsal approach is used in proximal pole fractures and volar approach is indicated in the waist and distal pole fractures and fractures with humpback flexion deformities. Arthroscopic assistance may be used in fixation.
Union rates of 90-95% have been reported with operative treatment of scaphoid fractures.
Complications of Scaphoid Fractures
Scaphoid Nonunion
Nonunion of scaphoid fracture occurs because of delayed diagnosis, gross displacement, associated injuries of the carpus, and impaired blood supply etc.
About 40% of non-unions are undiagnosed at the time of original injury.
Nonunion is 20% more common in smokers.
Timely recognized non-unions, without degenerative changes, can be treated by fixation and grafting.
Untreated scaphoid nonunion could lead to scaphoid nonunion advanced collapse of the wrist which, with time would lead to wrist arthritis.
In patients where the fracture has not shown any union even after 12 weeks of immobilization, the option of surgery should be discussed with the patient. If the patient wants a further trial of non-operative treatment, another cast can be applied for 4 weeks.
A fracture not uniting after 16 weeks should be considered for surgery.
The surgery consists of opening the fracture, removal of fibrous tissue, fixation with a compression screw and bone grafting.
Scaphoid nonunion can be of two types stable (Herbert Type D1) and unstable non union (Herbert Type D2) of scaphoid.
Stable nonunion of the scaphoid is characterized by a firm fibrous nonunion that prevents deformity from occurring
Xray of these cases would show a fracture line with variable cystic changes affecting the bone fragments. The patient in this kind of nonunion have minimal symptoms.
The patient with stable scaphoid nonunion should be encouraged to get treated in spite being symptom-free as fixation of stable nonunions give better results than unstable nonunions. [ And there is a risk of becoming a stable union an unstable union with additional trauma.]
An early treatment further reduces the incidence of secondary osteoarthritis. Percutaneous screw fixation provides good results.
Unstable Scaphoid Nonunion (Herbert Type D2) has sclerosis of bone surfaces, synovial erosion, fibrous cysts indicate an unstable nonunion.
Unstable scaphoid nonunion leads to decrease in fragment size, collapse and deformity.
Time between the initial fracture and treatment of the nonunion and the presence of osteonecrosis are important determinants of prognosis.
MRI can be used preoperatively for assessing presence of osteonecrosis.
Treatment of Scaphoid nonunion
Inlay (Russe) bone graft
The procedure is done in the following cases-
- Minimal deformity – No humpback scaphoid
- No adjacent carpal collapse
Interposition (Fisk) bone graft
- An opening wedge graft that is designed to restore scaphoid length and angulation
- adjacent carpal collapse
- excessive flexion deformity (humpback scaphoid)
Vascular bone graft
- From radius or medial femoral condyle
- Good option for proximal pole fractures with confirmed osteonecrosis by MRI
- Absence of pancarpal arthritis and collapse
Scapholunate Dissociation and SNAC wrist (Scaphoid nonunion advanced collapse)
Scaphoid fracture non-union leads to wrist instability, collapse, and degenerative changes.
Nonunions of the scaphoid are treated in one of the following ways:
- Radial styloidectomy
- Excision of the proximal fragment
- Proximal row carpectomy
- Total or partial arthrodesis of the wrist
Osteonecrosis of the Scaphoid
- The incidence – 30-40%,
- Most frequently occurs in fractures of the proximal third.
- Poor reduction, delayed surgery, and inadequate fixation of the scaphoid can increase the incident of osteonecrosis.
- Revision surgery with vascularized bone grafts may be necessary..
Late VISI of Carpus
the best way to prevent VISI deformity is to adequately repair the lunotriquetral interosseous ligament.
Late case of the VISI deformities can be treated with a dorsal capsulodesis involving the lunate and triquetrum or an ulnar four-bone arthrodesis.
Wrist Stiffness
Nearly all patients with transscaphoid perilunate fracture-dislocations will experience some decrease in wrist motion. Stable fixation in these injuries allows for early range-of-motion exercise, which may reduce the loss of motion. Static progressive splints can help certain patients regain motion postoperatively.
Wrist Arthrosis
In a number of cases, articular damage to the scaphoid or radius has been shown to be the inciting event for wrist degeneration. Osteonecrosis, poor reduction, and inadequate stabilization of the scaphoid can result in wrist arthrosis. In this cases, salvage procedures such as proximal row carpectomy or partial wrist arthrodesis can relieve pain and still allow some motion. In severe cases, a total wrist arthrodesis may be required.
Prognosis of Scaphoid Fractures
Proximal pole fractures have the poorest prognosis because the blood supply to the proximal pole is disrupted by the fracture.
Proximal 5th AVN rate of 100% and proximal 3rd AVN rate of 33%.
Transverse fracture patterns are considered more stable than vertical or oblique oriented fractures
The site of the fracture in scaphoid has been related to union rate. The reported rate of fractures in scaphoid is
- Waist fractures – 80%
- Proximal pole – 15%
- Tuberosity – 4%
- Distal articular fractures – 1%
The scaphoid staple fixation is associated with the union in about 95% of patients.
Surgery is increasingly used for patients who will not tolerate prolonged casting.
References
- Carpenter CR, Pines JM, Schuur JD, Muir M, Calfee RP, Raja AS. Adult scaphoid fracture. Acad Emerg Med. 2014 Feb. 21 (2):101-21
- Karantanas A, Dailiana Z, Malizos K. The role of MR imaging in scaphoid disorders. Eur Radiol. 2007 Nov. 17(11):2860-71.
- Capo JT, Shamian B, Rizzo M. Percutaneous screw fixation without bone grafting of scaphoid non-union. Isr Med Assoc J. 2012 Dec. 14(12):729-32.
- Huckstadt T, Klitscher D, Weltzien A, et al. Pediatric fractures of the carpal scaphoid: a retrospective clinical and radiological study. J Pediatr Orthop. 2007 Jun. 27(4):447-50.
- Pao VS, Chang J. Scaphoid nonunion: diagnosis and treatment. Plast Reconstr Surg. 2003 Nov. 112(6):1666-76; quiz 1677; discussion 1678-9.