Last Updated on November 22, 2023
Achilles tendon rupture commonly occurs in people playing recreational sports. The rupture usually occurs during an activity that puts a load on the Achilles tendon. Achilles tendon rupture is common generally people of middle age and above and can be treated both conservatively as well as surgically.
Most of the Achilles tendon rupture occurs approximately 2-6 cm above the calcaneal insertion of the tendon. Left leg is more affected than the right leg. It is thought that the left Achilles tendon is torn more often as right-handed people start push-off more often with the left foot.
Achilles tendon is the tendon of gastrocnemius and soleus muscles, located behind and above the heel and inserts on the posterior aspect if calcaneum.
It functions to move the foot into plantar flexion [downwards movement of the foot].
[Read Anatomy of Achilles tendon and Achilles tendinosis]
Persons who have had an Achilles rupture are more likely than others to have Achilles tendinosis and repeat rupture on the opposite side.
Causes of Achilles Tendon Rupture
Rupture of Achilles tendon can occur when a forceful push puts the excessive load at the tendon. – sudden or plantar flexion. Sudden or forced dorsiflexion of the ankle may also be the cause. Atrophy of Achilles tendon may contribute.
This is commonly seen in playing running, football, basketball, and tennis games. Achilles tendon is commonly seen in middle-aged recreational players. The push-off movement uses a strong contraction of the calf muscles which can stress the Achilles tendon too much.
Factors that increase the risk of Achilles tendon rupture –
- Prolonged oral steroids
- Local corticosteroid injections around the Achilles tendon
- Cushing’s syndrome [Rise in person’s own cortisol levels]
- Increasing age
- Achilles tendinosis
- Previous rupture of Achilles tendon
- Systemic conditions that weaken the tendon and make it prone to rupture
- Rheumatoid arthritis
- Gout
- Systemic lupus erythematosus.
- Quinolone antibiotics like ciprofloxacin
Presentation Achilles Tendon Rupture [Symptoms and Signs]
The symptoms may be noticed suddenly during a sporting activity or may occur even in normal walking.
There is a sudden sharp pain behind the heel and a snap or feeling of giving way. The sudden sharp pain settles quickly but some aching at the back of the lower leg may remain.
The patient is able to walk and bear weight but is not able to push off the ground on the side of rupture. The patient is also not able to tiptoe on the affected side.
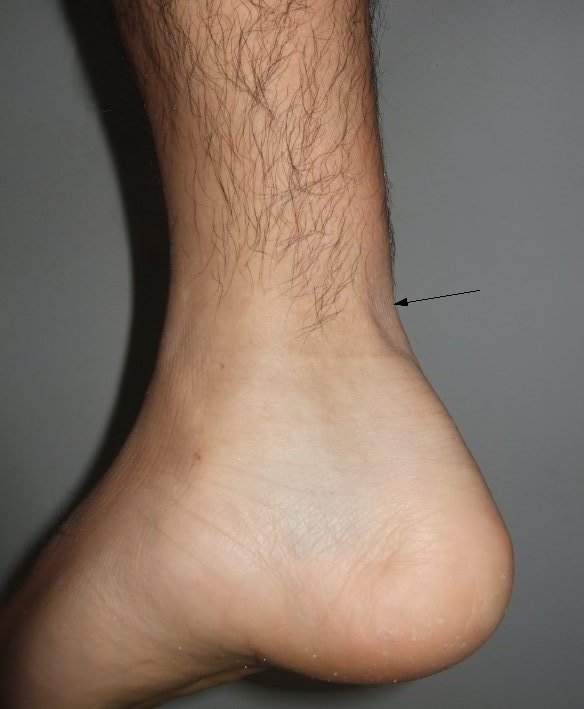
On examination, the normal contour of the Achilles tendon is not visible. The swelling of the area may be present. A gap may be felt above the back of the heel. A comparison with the opposite side helps to gauge the findings better.
Acute ruptures may show bruising have bruising around the area. The swelling of the calf may be present.
Clinical tests for Achilles tendon rupture
These include the following:
Hyperdorsiflexion sign
The patient lies prone and the knees are flexed to 90 degrees.
The examiner passively dorsiflexes both passive dorsiflexions of both feet. The affected feet goes farther in dorsiflexion than unaffected feet.
Thompson test
Pat lies prone and calf is squeezed in the extended leg. In a normal person, plantar flexion of the foot occurs with squeezing of the calf. In the case of Achilles tendon rupture, the extended leg may demonstrate no passive plantar flexion of the on squeezing of the calf.
O’Brien Needle Test
A needle is inserted about 10 cm proximal insertion of the Achilles tendon at calcaneum. When the foot is passively dorsiflexed, the hub of the needle will tilt towards head when Achilles tendon is intact but not in case of the ruptured tendon.
Differential Diagnoses
- Achilles tendinosis
- Calf strain
- Deep vein thrombosis of leg
- Ankle arthritis
Lab Studies
Not required for diagnosis but may be done for workup for surgery or to rule out other conditions.
Imaging
Ultrasound can be used to confirm the diagnosis of Achilles tendon rupture. It can also be used to determine the tendon thickness and site of the tear.
Magnetic resonance imaging can differentiate partial tears from complete tears. It can also tell about the presence of Achilles tendinosis.
X-rays do not have a major role in Achilles tendon rupture diagnosis.
Treatment of Achilles Tendon Rupture
Achilles tendon rupture is treated by nonoperative and operative methods.
In nonoperative treatment, brace or cast is applied in plantar flexion. This relieves the tension of the tendon and tendon is allowed to heal naturally usually up to 8 weeks. If tendon fails to heal, surgical repair may be done at a later stage.
In surgical treatment, torn ends Achilles tendon with or without augmentation by a tendon or a tendon graft is done. Following this, the limb is kept either in cast or orthosis about eight weeks
Both surgery and conservative treatment have been found to be effective.
But surgery has been associated with less number of re-ruptures and better strength of plantar flexion. But, the surgery carries the risk of wound healing problems.
Therefore surgery may be a better choice for active sports persons or young patients. Older or less active patients or patients with medical conditions may undergo conservative treatment.
The treatment is always influenced by the patient’s expectations and choices.
In an old neglected case, surgery should be preferred
Conservative Treatment
Indications for preference for conservative treatment of Achilles tendon rupture
- Elderly and/or inactive patients
- Systemic illnesses
- Poor skin integrity.
- Patients with diabetes
- History of wound healing problems
- Vascular disease
- Neuropathies
The patient is treated by serial casting and crutch ambulation without weight bearing
In the beginning, a long leg cast is applied with the knee in slight flexion and ankle in maximum plantar flexion to approximate the torn edges of the tendon.
The cast is changed in series, decreasing the plantar flexion and eventually moving toward short-leg casts in a neutral ankle position. The treatment is continued for 6-12 weeks.
After that patient is put on physical therapy.
Conservative treatment is less expensive and offers lesser risk. But chances of re-rupture are high.
Surgery for Achilles Tendon Rupture
The surgery includes Achilles tendon repair with or without augmentation by another tendon. Commonly used tendons for augmentation are flexor hallucis longus or peroneus tendon. Reinforcement mesh or fascial augmentation may be considered.
Surgery can be performed by two methods
- Open surgery – Involves making an incision in the back of the leg and stitching the torn ends of Achilles tendon together.
- Percutaneous surgery- The surgeon makes several small incisions, rather than one large incision to sew the tendon back together.
Percutaneous surgery has a lesser risk of wound healing problems but higher chances of sural nerve entrapment.
The patient needs extensive rehabilitation after conservative and surgical therapy to achieve the range of motion and functional strength. Rehabilitation includes stretch exercises and strengthening exercises. [see below]
Physical Therapy after Achilles Tendon Repair
The exercise should be performed under the supervision of expert and a continued assessment by the treating therapist which should guide the progress.
Following is a rough working protocol only and should be individualized from case to case.
- For the first three weeks
- the foot is kept in plaster or adjustable boot locked out at 30° of plantar flexion nonweight bearing
- Well-leg cycling and weight training may be done for cardiovascular conditioning
- In the next 3-8 weeks
- The patient is allowed to bear weight gradually beginning with toe touch and progressing to full weight bearing towards the end.
- The walking orthosis is adjusted by reducing 5 degrees every week till 10 degrees of plantar flexion is left.
- After 8 weeks
- A shoe with a lift in shoes may be worn.
- Passive stretch and range of motion exercises are begun.
- The patient should wean into regular shoe over a period of 2-4 weeks.
- Begin and gradually increase active/resistive exercises of the Achilles.
- The range of motion exercises should now cover an almost full range of motion.
- At 3 months
- Heel lifts should be weaned off
- Exercises like controlled squats, bilateral calf raise, toe raise, and eccentric exercises should begin
- Cycling should be done.
- The patient can progress to training jogging, jumping, and eccentric loading and sports specific exercises.
Prevention of Achilles Tendon Rupture
Achilles tendon rupture is not always preventable but following precautions would make it less likely.
- Do proper warm up before exercise.
- Gradually increase the intensity and duration of raining.
- Wear proper fitting shoe wear
Prognosis of Achilles Tendon Rupture
The tendon does take six to eight week and more time is needed for rehabilitation. Usually one can take 4 to 12 months before return to sport or previous activity level. A small amount of weakness may occur in some cases.
Complications occur both in conservative and operative treatment.
Immobilization may result in scarring or contracture. Wound complications are the primary concern with surgery [infection, sloughing, sinus formation, adhesions, and sural nerve injury]
Re-rupture can occur but are about three times less with surgery.