Last Updated on March 22, 2022
Baker cyst or popliteal cyst is a soft-tissue swelling that contains gelatinous fluid, in the posterior aspect of the knee. It occurs both in adults and children. In adults, the baker cyst communicates frequently with join and is associated with an intraarticular condition like meniscal tears or osteoarthritis. However, in children, this condition often does not communicate with joint and is not associated with any underlying pathology.
The name comes after the person who described it first, Dr. William Morrant Baker.
The most common location of Baker cyst is distal the popliteal crease under the medial head of the gastrocnemius muscle.
The following discussion focuses on adult baker cyst. Later on, in the same article, we will also discuss popliteal cysts in children.
Other names for this condition are
- Gastrocnemio-semimembranosus bursae
- Semimembranosus burse
- Synovial cysts
- Posterior herniae of the knee joint.
The Baker cyst is unilateral mostly. It is almost twice as common in boys than the girls. In children, the cyst infrequently communicates with joint however in adults, intra-articular pathology is common and recurrence may recur if joint pathology is not corrected.
The reported rate of prevalence is 4.7% in adults.
Causes and Types
Often the cyst communicates with the knee joint. The knee joint effusions may cause the gastrocnemius-semimembranosus bursa with synovial fluid giving rise to cyst.
Most of the cases of Baker cyst are secondary. That means there is an underlying joint issue. Arthritis is most common secondary cause. Osteoarthritis is most common arthritides associates with Baker cyst.
- Meniscal tears
- Rheumatoid arthritis
- Gout
- Anterior cruciate liament tear
Some authors list meniscal tears as most common cause.
Less commonly the cyst may occur without any knee pathology.
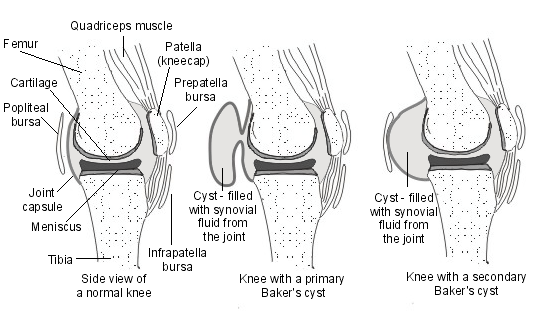
The cyst is primary if there is no knee pathology involved. It is called a secondary baker cyst if there is an underlying knee problem.
The cyst can vary in size, from a very small (asymptomatic) to a large one but a change in size is very common. Especially in smaller cysts a septum may exist separating the semimembranosus and gastrocnemius components. This may function as a flap valve allowing fluid to enter a popliteal cyst and not to exit it.
The cysts are medially located mostly but rarely they are laterally located. Occasionally extend into the calf of the leg.
Clinical Presentation – Symptoms and Signs of Baker Cyst
Swelling in the posterior aspect of the knee is the presenting complaint. Knee stiffness and pain may also occur. Symptoms of associated conditions may also be present. For example, in meniscal tears, locking of the knee may be present.
There could be vague posterior pain. stiffness in the back of the knee sometimes increased by activity
tightness behind the knee
The examination reveals a soft to firm swelling that is located usually distal to the popliteal crease.
The cyst can vary in size. In the same person, a change in size is common.
The popliteal cyst may be soft to firm in consistency. Transillumination test is positive [The passing of a strong beam of light through a part of the body for medical inspection.]
In the case of underlying pathology, the signs may point to that direction. For example, in meniscal tear, joint line tenderness may be present.
Other associations like chondral injury or cruciate ligament tear may need to be examined.
Large popliteal cysts can rupture and become painful.
Differential Diagnoses
- Ganglion cyst
- Meniscal cyst
- Popliteal artery aneurysm/ pseudoaneurysm
- Tumors
Imaging
X-rays
Plain radiographs provide limited information about the popliteal cyst but are useful for detecting other conditions commonly found in association with popliteal cysts, such as osteoarthritis, inflammatory arthritis, and loose bodies.
Baker cyst appears as a soft-tissue mass in the posteromedial knee joint. Occasionally, a Baker cyst is suggested by the presence of multiple, calcified, loose bodies in the cyst.
Ultrasound
It has almost replaced conventional arthrography as the initial assessment.
Ultrasonography allows determining whether the popliteal mass is a cyst or a mix of solid mass and cyst. Apart from assessment it also can determine the relation of the lesion to its adjacent structures and the presence of loose bodies or septations within the cyst.
While it is able to differentiate popliteal cysts from popliteal aneurysms and ganglion cysts, it is very helpful in differentiation from meniscal cysts or myxoid tumors.
Ultrasound does not very well identify communication to the joint space.
MRI
It is the gold standard for the diagnosis of Baker’s cyst. It can determine the extent and composition of the Baker cyst.
It can find communication between the cyst and joint space. In addition, it can assess the related disorders.
MRI is able to differentiate Baker cysts from other lesions.
CT
CT scan identifies the mass and also secondary findings, such as intracystic osseous fragments, mass effect, wall thickening, and bony erosion.
CT scanning is not as sensitive as MRI in detecting the associated internal derangement, which may be the cause of a Baker cyst.
Popliteal cyst usually arises in the medial part of the fossa. If the involvement is lateral, it could be something else.
Treatment of Baker Cyst
Most of the cases do not have symptoms. Asymptomatic cases do not require any treatment.
Nonoperative treatment is the first line of treatment. It mainly consists of
- Support stockings
- Non-steroidal anti-inflammatory drugs for pain control
- Ice compression are supportive treatments
- Fluid aspiration and steroid instillation
- Large Cyst
- Recurrence is common.
Operative treatment may be considered in cases where the cyst is very large, painful and other treatments have not worked.
The cysts are excised in these cases.
Whenever feasible underlying problem should also be addressed. For example, repairing a meniscal tear.
Though we are discussing that later, it is worthwhile to mention that in children, observation should be carried out on children for a period as the Baker cyst is known to regress in children.
Complications of Baker Cyst
Most of the popliteal cysts do not cause much of the problem. Large cysts, however, can cause pressure effects. following complications have been reported though these are rare
- Thrombophlebitis
- Stenosis of popliteal artery
- Nerve compression and muscle atrophy
- Rupture of the cyst
- Compartment Syndrome
Ruptured Baker cyst is discussed below.
Ruptured Baker Cyst
A Baker’s cyst can sometimes rupture. This can happen when the cyst is quite large. The rupture leads to leakage of the fluid into the calf causing strong pain, swelling and tightness of the calf.
The needs to be managed mostly with rest and supportive treatment as the fluid will be gradually resorbed by the body over a period of few weeks.
The recommended management for a ruptured cyst is
- RICE therapy
- Rest
- Intermittent Ice application
- Compression by elastic wrap
- Elevation – keeping the affected calf raised
- Medication for the pain
- Relative rest by avoiding activity
- Brace to support
The calf should be monitored for compartment syndrome.
Popliteal Cyst in Children
Baker cysts occur much less frequently in children than in adults. The estimated prevalence is about 2.4%.
Unlike the adult population, these are most often not associated with meniscal tears.
Most of them require observation only as the majority of lesions spontaneously resolve.
The presentation and physical features are juts like adults. These are located in the popliteal fossa medially and distal to the knee crease and are transilluminant soft tissue masses.
Most of these cases require observation only and resolve spontaneously.
Very rarely, the lesions with significant discomfort or very large cysts need to be excised. Those cases that do not regress spontaneously should also be excised.
References
- Sansone V, De Ponti A, Minio Paluello G, Del Maschio A. Popliteal cysts and associated disorders of the knee: critical review with MR imaging. Int Orthop. 1995;19:275-279.
- Torreggiani WC, Al-Ismail K, Munk PL, et al. The imaging spectrum of Baker’s (popliteal) cysts. Clin Radiol. 2002;57:681-691.
- DiRisio D, Lazaro R, Popp AJ. Nerve entrapment and calf atrophy caused by a Baker’s cyst: case report. Neurosurgery. 1994;35:333-334.
- Dunlop D, Parker PJ, Keating JF. Ruptured Baker’s cyst causing posterior compartment syndrome. Injury. 1997;28:561-562. [PubMed]
- Ji JH, Shafi M, Kim WY, Park SH, Cheon JO. Compressive neuropathy of the tibial nerve and peroneal nerve by a Baker’s cyst: case report. Knee. 2007;14:249-252. [PubMed]
- Olcott C, Mehigan JT. Popliteal artery stenosis caused by a Baker’s cyst. J Vasc Surg. 1986;4:403-405.