Last Updated on January 31, 2021
Charcot joint or Charcot arthropathy is the name given to neuropathic joint disease is a condition that causes progressive destruction of bone and soft tissues of joints especially weight-bearing joints and may also cause disruption of the bony architecture.
Charcot joint disease can occur at any joint but most commonly in the lower extremity, at the foot and ankle.
Charcot’s joint is named after Jean-Martin Charcot. Syphilis was the most common cause of Charcot arthropathy until 1936, now it is diabetes.
The prevalence of Charcot arthropathy has been reported from 0.1- 13% in different studies. Bilateral disease occurs in less than 10% of patients. A slight male preponderance has been reported.
Causes of Charcot Joint
It is a neuropathic condition and any condition that causes sensory or autonomic neuropathy can lead to a Charcot’s joint. Charcot joint has been reported as a complication of following
- Diabetes [most common cause]
- Syphilis
- Chronic alcoholism
- Leprosy
- Meningomyelocele
- Spinal cord injury
- Syringomyelia
- Renal dialysis
- Congenital insensitivity to pain.
Pathophysiology of Charcot Joint
The exact mechanism of Charcot joint disease is not known. Following theories suggest various mechanisms that may be responsible for this disease.
- Neurotraumatic theory
- Microinjury to the insensate joint
- Continuous microtrauma leads to progressive destruction and damage
- Neurovascular theory
- Increased blood flow in the limb due to preexisting condition
- Can result in an imbalance in destruction and synthesis
- Autonomic neuropathy leads to an abnormal bone formation
- Sensory neuropathy leads to an insensate joint that is susceptible to trauma.
Presentation of Charcot Joint
The clinical presentation of Charcot joint may vary from mild swelling and no deformity to moderate deformity with significant swelling depending on the stage of the disease.
Acute Charcot arthropathy presents with
- Swelling
- Increase in local skin temperature
- Erythema over joint
- Joint effusion
These features, in the presence of intact skin and a loss of protective sensation often point towards Charcot joint disease.
Typically, the pain minimal or when it is present, it is significantly less than the severity of joint involvement.
The patient may also have instability and loss of joint function.
Classification of Charcot Joint Disease
Saunders and Mrdjencovich classification is the most commonly used system. Their system classifies Charcot arthropathy of foot and ankle into 5 different patterns, as follows
- Pattern 1- Involves the forefoot [interphalangeal joints, the phalanges, and the metatarsophalangeal joint]
- Pattern 2- Tarsometatarsal joint
- Pattern 3- Cuneonavicular, talonavicular, and calcaneocuboid joints
- Pattern 4- Involves the ankle joint
- Pattern 5- Involves the posterior calcaneus
Patterns 2 and 3 are the most common.
Lab Studies
- Complete metabolic profile
- Complete blood count
- ESR
- Glycosylated hemoglobin (HbA1C) for diabetes
- Alkaline phosphatase, calcium, phosphorus, and parathyroid hormone for bony diseases like Paget
- Vitamin B12/folate levels
- DEficiency could suggest peripheral neuropathy or chronic alcoholism.
- Liver function tests
- Coagulation studies may be done in chronic alcoholism.
- Tests for syphlis
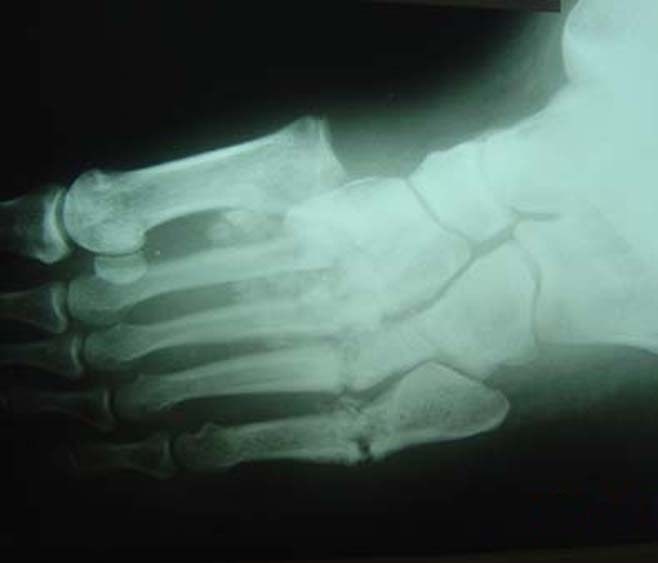
Imaging
Xrays help to confirm and stage disease and tell whether the disease is active. Osteopenia, periarticular fragmentation of bone, subluxations, dislocations, and fractures are usual finding in x-ray of Charcot joint depending on the destruction of the joint.
Bone scan can assist in differentiating between Charcot arthropathy and osteomyelitis.
MRI allows for anatomic imaging of the area. It also may help to distinguish between osteomyelitis and Charcot arthropathy.
Doppler ultrasound is used to rule out deep venous thrombosis.
Treatment
Treatment of Charcot arthropathy is primarily nonoperative.
Acute Phase
- Cast immobilization
- Reduces joint stress
- For 3-6 months
- Braces when casts are not suitable
Immobilization is discontinued when the disease process appears quite clinically, on x-ray and dermal thermometry
Patients are asked to reduce stress by remaining non-weight bearing or partial weight-bearing with crutches or walkers.
Follow up
After the removal of the cast lifelong protection of the involved limb is desired. Patients should wear a brace to protect the foot. A rocker-bottom sole can be used in presence of an ulcer. Plastazote inserts can be used for insensate feet.
The total healing process typically takes 1-2 years.
The major contraindication to surgery is active inflammation. Studies have shown less favorable outcomes when surgery is performed on an acute joint.
Surgical Treatment
Nondisplaced fractures, destroyed joints, destroyed bones, deformities like rocker bottom foot or clubfoot may require surgical treatment.
Surgery include
- Removal of bony prominence
- Osteotomy
- Arthrodesis
- Open reduction and internal fixation
- Reconstructive surgery
- Ankle fusion with Achilles tendon lengthening
- Amputation.
The choice of procedure is guided by the involvement of the joint and the severity of the destruction.