Last Updated on August 30, 2023
Complex regional pain syndrome or CRPS is a chronic painful condition causing intense pain, usually in the arms, hands, legs, or feet that usually results after an injury to the limb though few instances have been reported in the face or genitalia too.
The severity of the symptoms can range from mild to severe and the symptoms may last months or years. The cause of complex regional pain syndrome or CRPS is not known exactly.
Most of the people are known to recover fully. The symptoms recur in a few cases and can persist for years.
Previously, complex regional pain syndrome has been called by many names like
- Reflex sympathetic dystrophy
- Sudeck’s atrophy
- Reflex neurovascular dystrophy
- Algoneurodystrophy
- Causalgia [When associated with nerve injury]
Females are affected three times more commonly than males. The upper limb is more commonly affected than the lower in adults whereas in children leg is more common.
It is very rare in children. The incidence of CRPS type I is higher than that of CRPS type II.
Types of Complex Regional Pain Syndrome
Depending on the presence or absence of nerve involvement it can be on of the two types.
- Type I
- Earlier called reflex sympathetic dystrophy
- there is no demonstrable nerve lesions.
- Type II
- Earlier known as causalgia
- Associated with nerve damage.
CRPS can also either be acute (short-term) or chronic (lasting > 6 months).
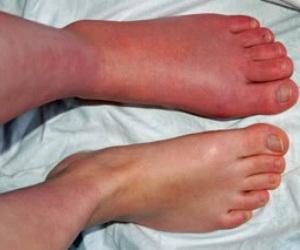
Causes of Complex Regional Pain Syndrome
Type II CRPS is associated with nerve injury.
Trauma to the limb is the most common cause of type I CRPS cases.
Following injuries may precipitate CRPS
- Sprain/strain
- Surgical wounds
- Fractures
- Crush injury/contusion
Rarely, the cases have been reported following venous puncture, lacerations, burns, inflammatory Conditions and electric shock.
Pathophysiology
The exact cause of the condition is not known.
It is believed persistent painful stimuli from an injured region cause peripheral and central sensitization.
The following explanations have been suggested for the development of CRPS
- Nervous system dysfunction
- Sympathetic hyperactivity due to disturbances
- somatosensory misinterpretation
- Neurogenic inflammation
- Increased inflammatory response
- Heightened pain sensations in pain fibers
- Hypoxia due to tightening of blood vessels
It is important to note that there are no specific diagnostic tests and CRPS is diagnosed mainly clinically.
Symptoms of CRPS
The symptoms of CRPS may begin immediately or even weeks after the initial injury. The following are the prominent symptoms. Not all the symptoms are present in all the patients. Moreover, the number of symptoms reduces as the recovery occurs.
- Pain
- Most common
- Spontaneous and diffuse over a region
- Burning, aching or throbbing
- Gets worsened with activity
- Difficulty in using the affected limb, easy fatigue
- Feeling as if the limb is foreign
- Temperature difference when compared to opposite limb
- Warmer or cooler
- Sweaty or drier than the opposite
A physical examination may reveal
- Weakness of the limb
- Clumpsy activities
- Decreased range of motion
- Tremors, dystonia, muscle spasms
- Decreased sensation
- Pain to touch and exaggerated response to pain, abnormal sweating [allodynia, hyperpathia, hyperhydrosis]
- Altered skin color
- Edema on the affected side
- Atrophy of the soft tissues, muscles, and bones [disuse also contributes]
- Decreased hair in the affected area and altered nail growth
The diagnosis of complex regional pain syndrome is mainly clinical.
Diagnostic Work-up
There is no specific confirmatory diagnostic test for the presence of CRPS. Routine blood investigations and imaging may not yield much information.
X-rays may show disuse osteoporosis of the involved limb part.
3-phase bone scintigraphy in early CRPS that occurs after fracture may help to diagnose and differentiate from other pain syndromes.
Neurogenic inflammation markers like interleukin-6, tumor necrosis factor-alpha, tryptase, and endothelin-1 may be raised.
Treatment of Complex Regional Pain Syndrome
The objective of the treatment is to restore functional extremity. Treatment is more effective when started early.
Following are the various treatment modalities.
Drugs
- Opioids or NSAIDs for pain control
- Tricyclic antidepressant
- Amitriptyline
- Desipramine
- Gamma-aminobutyric acid (GABA) agonist
- Baclofen for dystonia
- Gabapentin – for pain and sensory symptoms
- Intranasal calcitonin reduces pain
- Bisphosphonates
- improve pain, swelling, and range of movement
- mechanism of action unknown
- Corticosteroids
- Lidocaine patch
Interventional Procedures
- Sympathetic ganglion nerve blocks
- Intravenous regional sympathetic block
Guanethidine, bretylium, droperidol and ketanserin are commonly used for these blocks
Intravenous Infusions
- Phentolamine infusion
- Ketamine infusion
- IV immunoglobulin
Other Measures
- Epidural clonidine
- Spinal cord stimulation/neuromodulation
- Transcranial magnetic stimulation
Physical Therapy
Physical therapy is the most important component of treatment. It begins with the mobilization of the limb under supervision. Patients with less severe symptoms and have better motor functions are likely to benefit the most.
Physical therapy works to improve the blood flow and strength of the limb and works on mind training as well.
The following are the important components of physical therapy.
- Graded motor imagery including mirror therapy
- Desensitization of the affected part by exposure to various substances
- Lifestyle changes
- Quitting smoking:
- better management of existing health issues
- Exercises
- Stockings to reduce swelling
- Behavioural therapy for stress and anxiety control
Surgical Care
- Surgical sympathectomy
- Surgical decompression in CRPS type II if there is a defined nerve [i.e. capral tunnel syndrome]
- Amputation of the affected limb
- Last resort
- Rarely recommended
Prognosis of Complex Regional Pain Syndrome
In most people, CRPS usually gets better with time and eventually goes away.
Rarely, it may become prolonged.
Recurrence may be seen in about a quarter of cases.
Early intervention is associated with better results.
References
- Rockett M. Diagnosis, mechanisms and treatment of complex regional pain syndrome. Curr Opin Anaesthesiol. 2014 Oct. 27(5):494-500. [Link]
- Lee DH, Lee KJ, Cho KI, Noh EC, Jang JH, Kim YC, et al. Brain alterations and neurocognitive dysfunction in patients with complex regional pain syndrome. J Pain. 2015 Jun. 16 (6):580-6.