Last Updated on November 13, 2019
Joint aspiration or arthrocentesis is the procedure by which joint fluid is withdrawn using a needle. The fluid withdrawn is used in diagnostic tests. Arthrocentesis could also be used for therapeutic purposes.
Analysis of the joint fluid can enable the physician to differentiate between various joint pathologies.
Joint aspiration is a quick, inexpensive procedure and can be performed in outpatient settings.
Some deep joints like hip joint or joints of the spine should be aspirated under ultrasonographic guidance for improved accuracy.
Indications for Joint Aspiration
For diagnosis
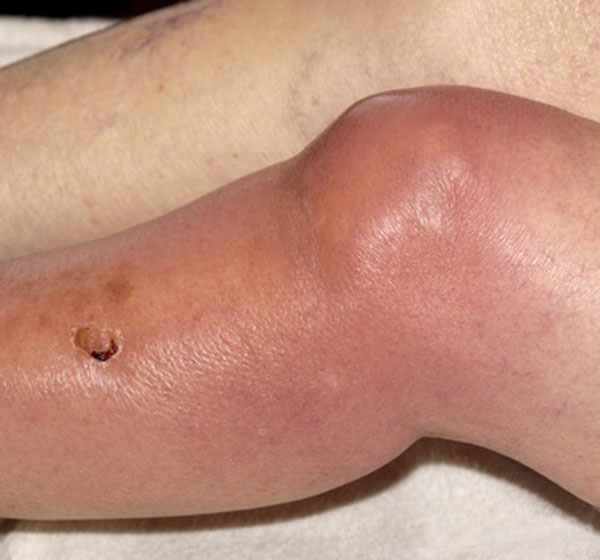
Joint aspiration should be considered for any patient with an inflamed joint [red, warm, tender, swollen, and painful] ] or joints who do not have an established diagnosis. In cases of prosthetic joint infections also, joint aspiration should be performed
For Treatment
Repeated aspirations can be used to relieve discomfort and prevent joint damage and is considered as part of the management of a septic joint.
Aspiration in cases of hemarthrosis can prevent adhesions.
Aspiration can be performed immediately prior to injecting intra-articular medications.
Contraindications for Joint Aspiration
Unless there is a strong suspicion of septic arthritis, a needle should not be passed through an area of infection (eg, overlying cellulitis) to avoid seeding of infection.
Patients who are on anticoagulant therapy or have a bleeding condition like hemophilia or thrombocytopenia are at increased risk for hemarthrosis with arthrocentesis. Whenever possible, aspiration should be delayed until the coagulopathy is reversed.
Different Gauges of Needles to be Used
- 1.5-in. 21- to 18-gauge needle for large joints like, knee, ankle or shoulder
- 1-in. 21-gauge needle for medium joints like wrist
- 1-in. 25-gauge needle for small joints metacarpophalangeal or metatarsophalangeal
- Longer needles if needed for deep joints or very obese patients
- A larger needle size may be selected if a large effusion is noted or if purulent fluid or hemarthrosis is known or suspected
Procedure of Joint Aspiration
The joint landmarks are palpated, and the insertion point is marked with ink.
The area is prepared with povidone-iodine solution and allowed to dry.
The iodine can then be wiped away from the needle insertion site with an alcohol pad to prevent irritation.
Chlorhexidine can be used in patients allergic to iodine.
If desired, 1% lidocaine without epinephrine can be instilled into the skin and subcutaneous tissue. Some surgeons prefer using spray.
The position of the patient may be lying or sitting, depending on the joint and preferences of the surgeon.
The joint to be aspirated is positioned depending on the joint type.
Some Important Tips
- If no fluid or only a small amount of fluid is encountered
- Move needle slightly further in the joint
- Thicker fluid/clogged debris – use wider bore needle
- Syringe fills and there is more fluid is still in the joint
- Change the syringe without removing the needle from the joint and without disturbing the needle’s position.
Arthrocentesis of Different Joints
Shoulder
The shoulder joint is usually aspirated in the sitting position. With the patient in a seated position, the arm is held comfortably at the patient’s side and externally rotated. The coracoid is palpated, and the needle is inserted approximately 1.5 in. laterally and 1.5 in. inferiorly.
Alternatively, the shoulder can be approached posteriorly by inserting the needle inferior to the acromion.
Wrist
The wrist is held in a straight line with the forearm. A dimple is palpated dorsally over the radiocarpal joint, which serves as the entry point for the needle. The needle is held perpendicular to the forearm and inserted dorsally.
Elbow
With the elbow in 90° flexion. The olecranon process, the lateral epicondyle, and the radial head are palpated. The needle is then inserted laterally into the triangle formed by these three structures.
Metacarpophalangeal joint
With the finger flexed, the needle is inserted dorsally and either medial or lateral to the extensor tendons.
Knee
The knee is slightly bent and the needle is held perpendicular to the leg. The needle is inserted medially beneath the patella at approximately 2 to the 3-o’clock position.
A lateral approach is also used in some cases.
if required, the prepatellar pouch can be emptied by gently applying pressure and squeezing the soft tissues.
Ankle
The ankle is held at 90° or slightly plantarflexed. A space medial to the tibialis anterior tendon or space palpated between the lateral malleolus and extensor digiti minimi can be used to approach the joint.
Metatarsophalangeal joint
The toe is held slightly flexed. The needle is inserted dorsally and either medial or lateral to the extensor tendons.
Complications of Joint Aspiration
Dry Tap
- Improper needle placement
- Small amount of effusion
- Mechanical obstruction of the needle against cartilage or thickened synovium
Cartilage Damage
Can be avoided by understanding the joint anatomy and avoiding further advancement of the needle into the joint space once synovial effusion enters the syringe.
Hemarthroses
- Usually small and self-limited
- and can be managed with observation alone.
Infection
With aseptic technique, the risk is negligible. In case the infection has occurred, it needs to be treated with antibiotics. Prophylactic antibiotics can be given where there is an increased risk of infection.
Analysis of Joint Fluid
Similar to other body fluids, common laboratory evaluation of synovial fluid involves
-
Physical examination
-
Chemical analysis
-
Microscopic evaluation
-
Microbiologic and serologic evaluations
- Cytology examination
Different types of preservatives may be required, as follows:
-
Sterile heparinized tubes for microbiology testing
-
Heparinized or EDTA tubes for cell count
-
No preservatives for most chemistry tests
-
Sodium fluoride NaF for glucose testing