Last Updated on July 31, 2019
Kienbock disease is osteonecrosis of lunate bone. It is also referred to as lunatomalacia, as coined by Robert Kienbock, a Viennese radiologist Robert Kienbock in 1910. It leads to the collapse of the lunate bone in the wrist following avascular necrosis of the lunate. It usually involves a single side.
Cause of Kienbock Disease
There is no single proven etiology. Vascular supply, lunate and distal radius geometry, the relationship between the radial curvature of the lunate and capitates, repetitive trauma and negative ulnar variance have been thought to put lunate at risk in event of repetitive loading.
The avascular necrosis is caused by disruption of blood supply to the lunate. Gymnasts and manual laborers are said to be at risk.
Presentation of Kienbock Disease
The most common age for presentation is 20-40 years in males. Women tend to present in much older age.
Dorsal wrist pain related to activity, wrist stiffness, and poor grip strength are common complaints. The pain may radiate up the wrist and forearm.
In males, the dominant hand is more commonly involved whereas women have almost the same involvement of dominant and nondominant hands.
On examination, there is swelling on the dorsal aspect of the wrist. Swelling and tenderness are frequently present over the radiocarpal joint. There may be associated with swelling over the lunate. Passive dorsiflexion of the middle finger produces the characteristic pain. Wrist dorsiflexion may also be limited. The grip is often weak.
Classifications of Kienbock Disease
Lichtman’s modification of Stahl’s classification is most widely used and divides the disease into 5 stages, as follows:
Stage I
Normal radiograph
Stage II
Increased radiodensity of lunate with a possible decrease of lunate height on the radial side only
Stage IIIa
Lunate collapse, no scaphoid rotation.
Stage IIIb
Lunate collapse, fixed scaphoid rotation
Stage IV
Degenerative changes around the lunate
Imaging
Xray
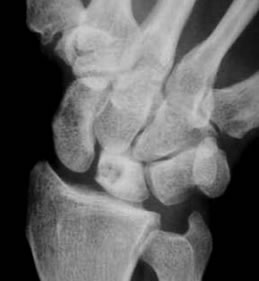
Initially, this may be normal or show sclerosis of the lunate. The lunate shows progressive loss of height, and fragmentation. The lunate collapse causes further degenerative joint changes (because of carpal instability) with bone cysts within the lunate.
Eventually, degenerative changes may involve the whole wrist. Plain films must also be examined to determine the amount of ulnar variance.
X-rays may show no specific abnormality in the early stages and MRI scans may be required.
CT
A CT scan would be the best imaging modality to evaluate the bony architecture of the lunate and useful in determining the true extent of disease and these have been found to the upgrading of the stage of disease [for example stage II disease may be upgraded to stage III].
Moreover, fractures that split the lunate into volar and dorsal halves are more evident with tomograms.
Bone Scan
Bone scanning is not specific enough but may help exclude the presence of Kienbock disease.
MRI
MRI is an extremely sensitive and specific test to detect the presence of marrow changes consistent with osteonecrosis. MRI has also been used to indirectly demonstrate revascularization following operative treatment.
Management of Keinbock Disease
The aim of the treatment is to reduce compressive loading of the lunate, permitting revascularisation and preventing lunate collapse.
In the early stage of disease splint and NSAIDs are used for treatment.
For reducing lunate load and allowing revascularisation may require surgery.
The primary contraindication to consider in the operative treatment of Kienbock disease is ulnar-positive or ulnar-neutral variance because in such cases, joint-leveling procedures (radial shortening and ulnar lengthening) cannot be performed.
Operative treatment can be classified broadly into
- Lunate excision with or without replacement
- Joint-leveling procedures
- Intercarpal fusions
- Revascularization
- Salvage procedures
- Other Procedures
Lunate excision with or without replacement
It could be either simple lunate excision, excision with soft-tissue (fascial or palmaris longus tendon graft) replacement or silicone replacement arthroplasty.
Joint Leveling Procedures
Radial shortening and ulnar lengthening are the two procedures to restore ulnar variance. The goal is to produce a wrist with neutral ulnar variance and these procedures reduce the strains on lunate up to 70%.
Intercarpal Fusions
Various intercarpal fusions for the treatment of Kienbock disease have been reported. The goal is to reduce lunate strain and, in procedures that involve the scaphoid, to correct and maintain proper scaphoid position.
- Scaphotrapeziotrapezoid fusion
- Scaphocapitate fusion.
- Scapitohamate fusion
Intercarpal fusions are more likely to be reserved for patients when a joint-leveling procedure is contraindicated due to with neutral or positive ulnar variance.
Revascularization
It involves the use of a vascular pedicle directly implanted into the lunate. It is done in a young patient with ulnar neutral or positive variance in whom a radial shortening is not an option. It is also suitable in a patient who wishes to avoid an intercarpal fusion.
Salvage Procedures
Salvage procedures are reserved for later stages of the disease and include proximal row carpectomy and wrist arthrodesis.
Other Procedures
- External fixation and bone grafting
- Arthroscopic debridement
- Wrist denervation
- Metaphyseal decompression
- Lunate core decompression
Image Credit: http://www.davidlnelson.md/articles/Kienbocks.htm