Last Updated on August 2, 2019
The leg length discrepancy means there is inequality of the length of the lower limbs. It is also called as limb length inequality. The problem is extremely common with 23% of the general population having a discrepancy of 1 cm or more
Leg length discrepancy causes compensatory gait abnormalities, degenerative arthritis of the lower extremity and lumbar spine. In addition to the length inequality, these patients may also have angular and torsional deformities that may influence their functional leg lengths. For example, flexion contractures around the knee and hip can cause apparent shortening of the leg.

Hip abduction contracture and ankle equinus cause functional lengthening.
Small leg length discrepancy is well compensated by the body and hardly requires any treatment. Bigger differences need to be equalized to prevent osteoarthritis, scoliosis, and backache in later life.
Causes of Leg Length Discrepancy
The causes can generally be divided into two broad categories: congenital and acquired.
Congenital limb length inequality
- Longitudinal deficiency of the fibula
- Hemihypertrophy syndromes
- Klippel-Trénaunay-Weber syndrome
- Skeletal Dysplasias
- Proximal femoral focal deficiency
- Developmental dysplasia of the hip
- Unilateral clubfoot
- Vascular malformation
- Congenital pseudarthrosis of the tibia
- Ollier’s disease
Paralytic disorders
- Spasticity (cerebral palsy)
- Poliomyelitis
- Spina bifida
- Spinal dysraphism
Acquired
- Physis disruption
- Infection
- Trauma
- Tumor
- Malunion of fracture
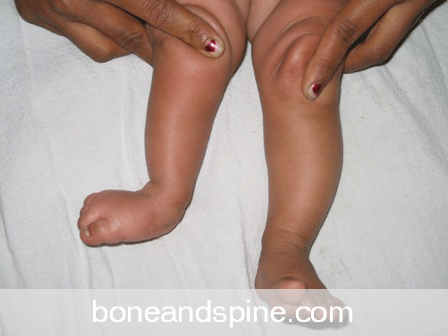
Functional Effects of Limb Length Discrepancy
- Back pain
- increased prevalence of back pain
- Osteoarthritis
- decreased coverage of femoral head on long leg side leads to osteoarthritis
- Structural scoliosis
- Limb length discrepancy increases the incidence of structural scoliosis
- Inefficient gait
Classification of Limb Length Discrepancy
- Static
- malunion of femur or tibia
- Progressive
- Physeal growth arrest
- Congenital
- Absolute discrepancy increases
- Proportion stands the same
Presentation of Limb Length Discrepancy
Patients could be without symptoms or present with gait abnormalities and deformities. Symptoms of the condition leading to discrepancy may be present.
The examination is done in detail to know the apparent and true leg length and associated deformities. It is important to know the status of spine and limb deformities as deformity correction may affect the leg length and thus final amount of correction needed.
The leg length discrepancy may be measured by block test or with measuring tape.
Block Method
For block testing, the patient stands and blocks are added under the short leg until the pelvis is level. The discrepancy can be measured from the block. This method takes into account the disparity in foot height between the two limbs and also aids in determining the functional LLD. This method is slightly more reliable and accurate than the use of the tape measure.
It is initial screening method as it would not take into the account the deformities that could be affecting the length.
Tape measure
A tape measure is typically used to measure the length of each lower extremity by measuring the distance between the anterior superior iliac spine (ASIS) and the medial malleolus and is referred to as the “direct” clinical method for measuring leg length discrepancy The value could be affected by differences in the girth of the two limbs, and difficulty in identifying bony prominences as well as angular deformities
An apparent leg length can be measured from the umbilicus to the medial malleoli of the ankle
Tape measurement measures the true limb length from the anterior superior iliac spine to the medial malleolus with a tape measure after correcting pelvic tilt and deformities.
The patient is finally evaluated for the status of hip, knee and ankle joints. Any deformity there would affect the apparent limb length. For example, hip adduction contracture causes apparent shortening.
Imaging
X-rays of Hand
These are done for determining the bone age.
Orthoroentogenogram
An orthoroentgenogram utilizes three radiographic exposures centered over the hip, knee and ankle joints in order to minimize magnification error.
Scanogram
With the lower limbs similarly positioned with both patellae pointing towards the ceiling and a radio-opaque ruler taped to the table between the limbs. The film cassette is moved under the patient between exposures while the patient remains motionless between the three exposures. [In orthroentogenogram, a single cassette is used.]
Teleoroentgenogram
The teleoroentgenogram is a full-length standing AP radiograph of the lower extremity in standing position with both patellae pointing directly anteriorly. The x-ray beam centered at the knee from a distance of approximately 6 feet (180 cm) while the patient stands erect. An attempt is made to level the pelvis with an appropriately sized lift placed under the short limb
CT Scanography
CT scanography is the most accurate diagnostic test with contractures of the hip, knee, or ankle. It obtains digitalized images.
Prediction and Projections of Limb Length Discrepancies
Patients are often seen as young and for accurate correction of leg length, it needs to be determined what would be their leg length discrepancy at the time of maturity. This knowledge is then incorporated into the treatment which then plans the quantum of correction
It is assumed that growth continues until 16 yrs in boys and until 14 yrs in girls.
It is assumed that leg grows 23 mm/year, with most of that coming from the knee (15 mm/yr)
- Proximal femur – 3 mm / yr
- Distal femur – 9 mm / yr
- Proximal tibia – 6 mm / yr
- Distal tibia – 5 mm / yr
Moseley Graph
Moseley devised a straight-line graph based on a logarithmic scale of relative rates of limb growth along w/ expected discrepancy at maturity;
– straight line graph also allows estimation of how epiphysiodesis will affect the long lower limb at different ages;
– graph requires > 3 sequential measurements of bone age at 4-month intervals
Green-Anderson tables
These use extremity length for a given age.
Multiplier method
It is a prediction based on multiplying the current discrepancy by a sex and age-specific factor. It is most accurate for congenital leg length discrepancies.
Treatment of Leg Length Discrepancy
Goals of treatment are
- Leg length equality within 1 cm
- Level pelvis
- Functional improvement
In certain cases, small leg length inequality may be beneficial to the patient especially in neuromuscular disorders to aid in clearance in the swing phase of gait.
Depending on the severity of the difference, different treatments can be used for correction of the inequality.
Treatment of leg length inequality involves many different approaches. Nonoperative treatment involves the use of shoe raises or orthotics.
Surgical approach deals with the problem by
- Correction of deformity if present
- Shortening of the normal leg
- Lengthening of the affected leg
- Combination of shortening and lengthening.
Non-operative Treatment
An inequality < 2cm projected at maturity is generally without any functional problems. Raises up to 1 cm can be inserted in the shoe. For larger leg length inequalities, the shoe must be built up.
Leg length inequalities beyond 5 cm are difficult to treat with a shoe lift.
A foot-in-foot prosthesis can be used for larger leg length inequalities but is often not tolerated well. It is often used as a temporary measure.
Surgical Treatment
Shortening of the long side
Epiphysiodesis of femur, tibia, or both
Epiphysiodesis inhibits the growth of the limb and can be used to correct 2-5 cm of projected limb length discrepancy.
It can be performed only in skeletally immature patients where growth potential is still present.
Because the procedure effectively shortens the longer leg and is usually done on the uninvolved side, it may be unappealing to the patient and family.
It can be used alone or with limb lengthening of the short limb.
Shortening of Mature Limb
This involves ostectomy and removal of bone segment followed by fixation of remaining fragments with the desirable fixation device.
Limb lengthening of the short side
It is contemplated in cases > 5 cm projected discrepancy. It can be combined with a shortening procedure (epiphysiodesis, ostectomy) on the long side when the discrepancy is large [>8 cmm]
Lengthening is usually done by corticotomy and gradual distraction
The limits of lengthening depend on patient tolerance, bony consolidation, maintenance of a range of motion, and stability of the joints above and below the lengthened limb.
Numerous fixation devices are available, such as the ring fixator with fine wires, monolateral fixator with half pins, or a hybrid frame.
Large leg length inequalities can be treated by staged lengthenings or by simultaneous ipsilateral femoral and tibial lengthenings.
Adverse effects of limb lengthening include muscle weakness, pain, and possible physeal inhibition.
It is contraindicated in the case of acetabular dysplasia and instability of the knee due to congenital ligament deficiency since a major joint dislocation may follow distraction.
Amputation and Prosthetic Fitting
- Non-reconstructable limb [Severe limb dysplasia]
- > 20 cm projected leg length discrepancy
References
- Kaufman KR, Miller LS, Sutherland DH: Gait asymmetry in patients with limb-length inequality. J Pediatr Orthop 16:144-150, 1996
- Liu XC, Fabry G, Molenaers G, et al: Kinematic and kinetic asymmetry in patients with leg-length discrepancy. J Pediatr Orthop 18:187-189, 1998
- Aaron A, Weinstein D, Thickman D, et al: Comparison of orthoroentgenography and computed tomography in the measurement of limb-length discrepancy. J Bone Joint Surg 74:897-902, 1992
- Karger C, Guille JT, Bowen JR: Lengthening of congenital lower limb deficiencies. Clin Orthop 291:236-245, 1993
- Maffulli N, Fixsen JA: Distraction osteogenesis in congenital limb length discrepancy: a review. J R Coll Surg Edinb 41:258-264, 1996
- Noonan KJ, Leyes M, Forriol F, et al: Distraction osteogenesis of the lower extremity with use of monolateral external fixation. J Bone Joint Surg Am 80:793-806, 1998
- Maffulli N, Lombari C, Matarazzo L, et al: A review of 240 patients undergoing distraction osteogenesis for congenital post-traumatic or postinfective lower limb length discrepancy. J Am Coll Surg 182:394-402, 1996
- Aaron AD, Eilert RE: Results of the Wagner and Ilizarov methods of limb-lengthening. J Bone Joint Surg Am 78:20-29, 1996