Last Updated on October 30, 2023
The microfracture chondroplasty is a technique to treat full-thickness cartilage defects that lead to the formation of new joint surface cartilage.
It includes the debridement of the damaged area and puncturing the underlying bone with a micro-instrument or pick to allow bleeding from the bone. The resulting blood clot that fills the cartilage defect has specialized cells which have the potential to transform into new cartilage.
This procedure is reserved for more significant areas of joint surface damage where the lesion is full thickness and down to the underlying bone. Microfracture can be performed on any size lesion, but better results have been obtained with lesions smaller than 400 mm.
The articular cartilage of the knee is 2 to 4 mm thick, avascular tissue devoid of nerves and lymphatics. Articular cartilage defects that extend for the full thickness to subchondral bone rarely heal without intervention. These injuries could be due to acute trauma or repetitive strain.
Initially developed for knee defects, microfracture chondroplasty is used now for hip, talus, elbow, and shoulder as well.
Indications for Microfracture Chondroplasty
- Full-thickness articular cartilage defects in the weight-bearing area
- Unstable cartilage flaps in these regions that extend to the subchondral bone
Timing of Procedure
Acute full thickness cartilage loss is treated as soon as possible.
Chronic lesions or degenerative lesions are first treated conservatively initially for at least 12 weeks by activity modification, physical therapy, NSAIDs, and joint injections, as appropriate.
Patients who have failed conservative treatment for chronic or degenerative lesions then become candidates for microfracture chondroplasty.
Contraindications
- Patients who unable or unlikely to complete the rehabilitation
- Advanced age
- Generalized degenerative changes
- Inflammatory arthritis
- Unstable knees are relative contraindications.
Most of these are relative contraindications
Surgical Technique of Microfracture Chondroplasty
The procedure is done under either regional or general anesthesia.
The patient is kept supine on a standard operating table.
Standard arthroscopic portals can be used for microfracture.
The lesion is identified for microfracture and probed thoroughly to make sure that all bordering cartilage is stable.
A creation of stable full-thickness borders of cartilage surrounding a central lesion is optimal for microfracture chondroplasty. It provides some degree of protection to the regenerating tissue that is forming in the treated lesion.
Using a shaver, all loose flaps of cartilage are removed.
Then proceed to remove the calcified cartilage layer by using a hand-held curette.
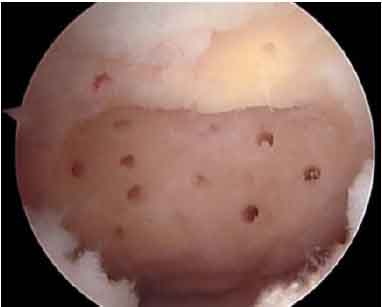
This will complete the bed preparation.
Now advance the arthroscopic awls through the subchondral bone to create multiple small holes or microfractures to a depth that allows the return of fat droplets or blood from the cancellous bone.
The usual depth of the holes is 2 to 4 mm.
Keep the holes as close together as possible without breaking one into the next.
The microfracture awl produces a roughened surface in the subchondral bone. This rough surface allows the marrow clot to adhere more easily.
Once the microfracture is complete, the pieces of equipment is removed from the joint. Do not use intra-articular drains. All portal sites are closed with suture and wounds are dressed.
Rehabilitation
Put the patient on the continuous passive motion, as tolerated. Stationary biking without resistance and deep-water exercise programs are started at 1 to 2 weeks after microfracture.
Patients with weight-bearing lesions are also prescribed toe-touch weight bearing with crutches for 6 to 8 weeks.
Patients who have undergone microfracture chondroplasty in the patellofemoral joint are treated in a locking brace with flexion limited to 20 degrees.
This is done to eliminate shear forces across the lesion during walking. Brace is removed/unlocked only for continuous passive motion exercises. The brace is worn for at least 8 weeks. The brace is then discontinued after the full range of motion is gradually achieved over approximately 1 week.
Anti-inflammatory medications and physical therapy modalities are prescribed as appropriate.