Last Updated on August 2, 2019
Nail Patella syndrome is an autosomal dominant condition characterized abnormalities of the nails, knees, elbows, and pelvis.
The features vary in severity from individual to individual, even among members of the same family.
The classical description is of a tetrad of nail dysplasia, patellar aplasia-hypoplasia, elbow joint dysplasia, and iliac horns.
Nail abnormalities are seen in almost all individuals with nail-patella syndrome. Patients commonly have skeletal abnormalities involving the knees, elbows, and hips.
The kneecaps or patellae are small, irregularly shaped, or absent. Patellar dislocation is common.
Individuals have increased the risk of developing glaucoma at an early age. Some people develop kidney disease, which can progress to kidney failure.
The prevalence of nail-patella syndrome is estimated to be 1 in 50,000 individuals.
Males and females are equally affected.
Other Names for Nail Patella Syndrome
- Fong disease
- Hereditary onycho-osteodysplasia
- Hereditary osteo-onychodysplasia
- Osterreicher syndrome
- Pelvic horn syndrome
- Turner-Kieser syndrome
Pathophysiology and Genetics
The LMX1B gene is a transcription factor involved in the patterning of limbs including patterning of the nails, digits, elbows, and patellae. It is also involved in the differentiation and function of kidney podocytes, development of the anterior eye structures, and the central nervous system.
The LMX1B protein is important during early embryonic development of the limbs, kidneys, and eyes.
Mutations in the LMX1B gene lead to the production of defective protein but how it can lead to the signs and symptoms of nail-patella syndrome is not clear yet.
The loss of function of one allele of LMX1B is known to cause nail-patella syndrome.
Presentation of Nail Patella Syndrome
These patients also tend to have an overall typically thin body habitus, and they have difficulty gaining weight. Other findings on physical examination may include the following. These patients have the following spectrum of problems. Different people may have a different set of conditions and symptoms.
The hallmark features of this syndrome are poorly developed fingernails, toenails, and kneecaps.
Nail Anomalies
These are present at birth. Nails may be absent, short or dystrophic with ridges. Sometimes triangular lunulae is the sole nail anomaly. Thumb is usually most severely affected.
Decreased creases over the distal interphalangeal joints are noted.

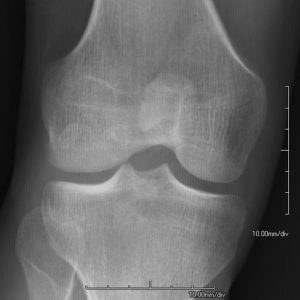
Knees
The patients have recurrent patellar dislocations and frequent knee pains. Deformities of the knees may be present.
Patellae may be absent or hypoplastic. Osteoarthritic changes may be present.
Elbows
Pain in the elbow and decreased movements of the elbow are known. The radius may be hypoplastic and posteriorly placed. Webbing of the skin may be present.
Back Pain
Back pain is common in nail-patella syndrome. Conditions like spondylolisthesis may be observed.
Kidneys
Proteinuria, hypertension, and/or decreased renal function may be observed. However,end-stage renal disease is relatively rare [5% of patients].
Eyes
A rise in eye pressure or open-angle glaucoma may be observed. Early detection of elevated intraocular pressure and appropriate treatment may prevent the nerve or retinal damage. Lester sign is a hyperpigmented, irregular ring in the iris may be noted.
Iliac Horns

These are bony prominences found in about 70% of patients which are typically asymptomatic and may be palpable on the posterolateral iliac bones or detected on x-ray. These are considered pathognomonic of nail-patella syndrome.
Other Conditions
Attention deficit disorder may be more common in patients with the nail-patella syndrome. These patients may have a higher risk of preeclampsia in pregnancy. It is a condition where there is a rise in blood pressure along with other changes.
Constipation and irritable bowel syndrome are more common
Flat foot or pes planus is seen in the majority of patients with the nail-patella syndrome.
Differential Diagnoses
- Genitopatellar syndrome
- Meier-Gorlin syndrome
- Patellar aplasia-hypoplasia
- RAPADILINO syndrome
- Small patella syndrome
Laboratory Studies
LMX1B Sequencing
This is diagnostic in the majority of patients. Once a mutation is found, other family members should also undergo testing.
Screening and Follow Up Investigations
- Yearly urinalysis with microscopy along with urine protein to creatinine ratio to assess kidney functions
- Yearly blood pressure measurements
- Yearly BUN and creatinine level assessments are indicated.
- Consider 24-hour urine protein and creatinine excretion if the above tests are abnormal.
Imaging
Xrays may reveal
- Iliac horns
- Hypoplastic patellae
- Abnormal radial heads.
MRI is indicated if joint surgery is contemplated. MRI is done to identify abnormal tendon, ligament, and/or muscle insertions and vessel distribution prior to surgery.
Dual-energy x-ray absorptiometry or DXA may be considered to evaluate bone mineral content.
Treatment
Drug treatment as required is started. For example, ACE inhibitors for proteinuria, hypertension, or both are indicated. No dietary restrictions are necessary unless hypertension or nephrotic syndrome develop.
Renal biopsy may be needed in some cases to assess kidney disease
Vitamin D analogs, thiazides, and prednisone are effective in reducing symptoms of nephrotic syndrome and end-stage renal failure.
Ocular examination may be considered on regular basis including intraocular pressure and visual fields examination.
Dialysis/ renal transplant may be indicated in as patients who have end-stage renal disease.
Physical therapy, bracing, and analgesics can be considered for joint pains.
Patella realignment surgery may help in cases of recurrent dislocation. Joint replacement may be beneficial in severe osteoarthritis of the knee or elbow.
Excision of the radial head may lead to pain relief but does not cause improvement in movements.
Annual renal function screening with urinalysis, and blood pressure assessment is indicated.
Prognosis of Nail Patella Syndrome
30-55% of patients with nail-patella syndrome develop a renal disease and end-stage renal disease may develop in about 5%.
Prognosis after renal transplantation is good.
All patients of nail-patella syndrome should undergo regular renal and ocular checkups.
Genetic counseling is recommended because the risk of having affected offspring is 50%. Prenatal diagnosis using molecular analysis is possible but severity cannot be predicted.