Last Updated on August 2, 2019
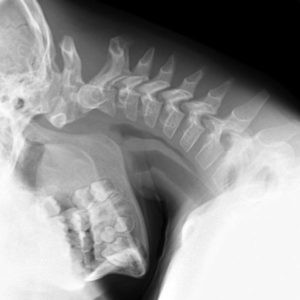
Os odontoideum is an anomaly where the tip of the odontoid process is divided by a wide transverse gap. This leaves the apical segment without its basilar support. the odontoid process or dens is separated from the body of the axis. Odontoid process is part of axis [name of the second vertebra] in a normal population.
This makes odontoid process loose and can lead to cervical instability and neural symptoms though many of os odontoideum cases are asymptomatic.
This anomaly is very rare and the exact incidence is unknown. While the exact etiology is not understood, it most likely represents an unrecognized fracture at the base of the odontoid or damage to the epiphyseal plate during the first few years of life.
Either of these can compromise the blood supply to the developing odontoid, resulting in the os odontoideum.
Classification [ Anderson/Alonzo classification]
- Type I: fracture of the upper part of the odontoid peg. Rare and potentially unstable
- Type II: fracture at the base of the odontoid. Unstable, and has a high risk of non-union
- Type III: through the odontoid and into the lateral masses of C2. Best prognosis for healing because of the larger surface area of the fracture.
Relevant Anatomy
The second cervical vertebra is also known as axis. It is identified by the presence of the dens (also called odontoid process), which is a strong, tooth-like process projecting upwards from the body of axis. The dens is usually believed to represent the centrum (body) of the atlas or first cervical vertebra which has fused with the centrum of the axis.
The dens articulates anteriorly with the anterior arch of the atlas, and posteriorly with the transverse ligament of the atlas.
During development, C0, C1, and C2 sclerotomes contribute to various portions of the dens. The principal portion of the dens body arises from the original center of C1.
The atlantoaxial joint stability is mainly by provided by ligaments.
The vertebral artery passes inferior to the C1-C2 facet joint, then course laterally through the transverse foramen of C2. Just above the C1 lateral mass, they turn medially and meet to progress cephalad into the foramen magnum. Deviations in the course are known.
Etiology
Although it was originally thought to be a congenital lesion due to a failure of the center of ossification of the dens to fuse with the body of C2, it may actually represent an unremembered and/or unrecognized fracture through the C2/dens growth plate before the age of 5 or 6.
Other causes postulated are embryological or vascular.
Os odontoideum has an increased frequency in patients with Morquio syndrome, Multiple Epiphyseal Dysplasia, and Down syndrome.
The level of mobility is below the transverse atlantal ligament and therefore results in abnormal mobility of the dens with respect to C2.
Subtypes of Os odontoideum
Orthotopic
The separated part is in a normal position with a wide gap between C2 and os odontoideum.
Dystopic
The separated part is displaced.
Presentation of Os Odontoideum
The age at diagnosis varies significantly from the first to the sixth decade of life.
A significant percentage of people with os odontoideum remain asymptomatic. It may be detected incidentally.
Symptoms of os odontoideum occur due to neck instability
- Neck pain
- Torticollis and headache
- Thoracic pain only.
- Symptoms of neurovascular compression – compression of the vertebral artery and spinal cord
- Transitory diffuse paresis that may progress to myelopathy to complete spinal cord injury.
- Weakness and ataxia
- Syncope
- Vertigo
- Visual disturbances
- Brainstem infarcts and seizures are seen.
On examination, tenderness may be noted in the C1-C2 region. The patient should be evaluated for a range of motion examination and assessment of cerebellar and brainstem function. Gait evaluation and Romberg test need to be checked.
Upper motor neuron findings like spasticity, hyperreflexia, clonus, and proprioceptive loss are commonly found in atlanto-axial instability.
Differential Diagnosis
- persistent ossiculum terminale
- odontoid fracture
Imaging Studies
Radiologic evaluation is used to confirm the diagnosis and estimate the degree of spinal instability.
Open-mouth anterior-posterior view
This xray could help to differentiate between os odinteum, its subtypes and tell if it is a fracture or os odontoideum.
It appears as a round or oval ossicle which has a smooth uniform cortex. It is separated from the base of the axis by a wide gap. There is a mismatch between the ossicle border and the axis body.
The gap separating the os and the axis should lies above the level of the superior articular facets.
Orthotopic os odontoideum appear free and in a relatively anatomic position whereas a dystopic ossicle may be fixed to the clivus or to the anterior ring of the atlas.
There would be a hypertrophy of the anterior arch of the atlas due to osseous reaction to chronic atlantoaxial instability. Presence of this hypertrophy differentiates the os odontoideum from an acute dens fracture.
Flexion-extension lateral radiographs.
Relative motion is observed in symptomatic patients, seen typically in the anterior-posterior plane but can be visualized in all planes in some patients.
MRI
MRI is able to show the cord compression and pathologic changes within the cord. It is able to show relationship of os odontoideum to surrounding bony tissues
CT angiography/Magnetic resonance angiography
Helpful in understanding aberrant vertebral artery anatomy or persistence of the first segmental artery
Treatment of Os Odontoideum
Non Operative Management
Observation is sufficient in nonsymptomatic patients. Medical management of symptomatic patients consists of cervical traction, physical therapy, cervical collar use, and anti-inflammatory medications.
Physical therapy may include traction and three to six months in a Minerva jacket or a brace. In most patients, the therapy leads to fusion of the atlanto-axial joint.
Operative Management
Operative management is indicated in the following settings
- Spinal instability
- Neurologic involvement
- Intractable pain
Changes on flexion-extension plain lateral cervical radiographs serve as reasonable guidelines for surgery:
- Posterior atlantodens interval <13 mm
- Sagittal plane rotational angle> 20°
- Instability index > 40%
- C1-C2 translation > 5 mm
Several surgical options have been utilized for os odontoideum:
Posterior atlantoaxial onlay fusion
These are associated with high pseudarthrosis rates and should be restricted to younger children for whom wire passage is considered high risk.
This procedure requires postoperative external immobilization, such as a halo brace or Minerva cast.
Wiring and Fusion
It can be posterior atlantoaxial wiring and fusion or posterior occipitocervical wiring and fusion
While posterior wiring procedures have a long record of successful atlantoaxial stabilization, their use is declining in this patient population. Shortcomings include the need for postoperative halo or Minerva cast immobilization.
Posterior Magerl screw fixation and fusion
The Magerl technique of posterior C2-C1 screw fixation reliably and cost-effectively immobilizes the atlantoaxial joint.
Harms-Goel technique of C1-C2 fusion
Goel-Harms has become the common C1-2 stabilization option in adults and older children.
Anterior resection of the os fragment
Rarely, symptoms and cord compression persist. In these cases, anterior decompression with removal of the os fragment is recommended.
Complications
- Non-operative management may be complicated by the progression of instability.
- Surgical complications
- Pseudarthrosis rates are from 0-4%.
- Neurologic decline may occur after surgery
- Injury to the vertebral artery
- Posterior cervical wound infections, anesthesia complications,
- Ongoing muscular neck pain