Last Updated on October 29, 2023
Pilon fractures or plafond fracture are fractures of the distal part of tibia involving its articular surface at the ankle joint. Pilon is a French word for pestle, an instrument used for crushing or pounding.
Pilon fractures account for approximately 10% of tibial fractures.
These fractures involve the dome of the distal tibial articular surface and extend into the adjacent metaphysis. The fibula may or may not be fractured.
The average patient age for pilon fractures is 35-40 years. They are more common in males than females.
Relevant Anatomy
The distal tibia and fibula, along with the ligaments and capsule the ankle mortise. The lateral aspect of the distal tibia forms a triangular notch, that articulates with the fibula. The bones are bound together by the anterior and posterior tibiofibular ligaments.
The ligaments often avulse fragments from the tibia and particular pattern of the fragments is noted [see below]
The blood supply in the distal leg is provided by branches that arise from the posterior tibial, peroneal, and dorsalis pedis arteries.
Pathophysiology of Pilon Fractures
The fractures occur due to high energy axial loading as in motor vehicle accidents or fall from height.
The pilon fractures are characterized by
- Articular impaction and comminution
- Metaphyseal bone comminution
- Soft tissue injury (open or Tscherne II/III closed fractures)
- 75% have associated fibula fractures
Following fragments are typically associated with pilon fractures. These fragments denote avulsed bone fragments with intact ligaments.
- Medial malleolar (deltoid ligament)
- Posterolateral/Volkmann fragment (posterior inferior tibiofibular ligament)
- Anterolateral/Chaput fragment (anterior inferior tibiofibular ligament)
- Posterior malleolar or Wagstaffe fragment
Mechanism of Injury
Pilon fractures occur when the talus is driven into the tibial plafond. The forces involved could be vertical, rotational, angular, or a combination of these.
Depending on the forces involved, different injury patterns result.
Low-impact pilon fractures
- Low-energy rotational force and some axial compression
- Little soft-tissue injury
- Little articular comminution
- Follow activities such as skiing
High-impact pilon fractures
- High-energy axial compression
- Extensive soft-tissue injury
- Severe articular and metaphyseal comminution
- Fall from a height or a high-speed motor vehicle accident
- The fibula is usually fractured
Classification of Pilon Fractures
Two fracture classifications are commonly used, both of them based on the fracture pattern seen on radiographs, the degree of comminution, and displacement of the fragments.
Ruedi and Allgower classification

Type A
Simple cleavage-type fractures with little or no articular displacement
Type B
Displaced by articular surface fractures without comminution
Type C
Intra-articular displacement with marked comminution
AO/OTA classification

Type A
- Extra-articular
- A1 – simple
- A2 – comminuted
- A3 – severely comminuted
Type B
- Fractures involve only a portion of the articular surface and a single column
- B1 – Pure split
- B2 – Split with depression
- B3 – Depression with multiple fragments
Type C
- Fractures involve the whole of the articular surface
- C1- Simple split in the articular surface and the metaphysis
- C2 – Simple articular split with multifragmentary metaphyseal split
- C3- Multiple fragments of the articular surface and the metaphysis
Klammer Classification of Posterior Pilon Fractures
Pilon fractures associated with posterior disruption and instability requires posterior stabilization and is potentially associated with worse outcomes.
The classification divides posterior pilon fractures into three primary categories by increasing degree of complexity, as follows
Type 1
Fractures with a single medially based posterior malleolar fragment
Type 2
The posterior fragment is split with possible posteromedial comminution
Type 3
Fractures have the fracture line of the posterior malleolus exit the medial malleolus anterior to the posterior colliculus, and an additional anteromedial fragment is present.
History and Physical Examination
Patients involved in high-energy trauma should be first be stabilized and critical injuries must be addressed first.
Clinical presentation varies, depending on the severity of the injury and the duration from the time of the injury
Ankle pain, inability to bear weight, deformity could be presenting symptom.
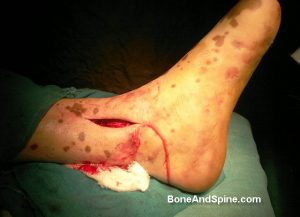
The examination must look for soft tissue integrity, swelling, abrasions, ecchymosis, fracture blisters, open wounds.
[Classification of soft tissue injury associated with fractures]
The patient should be examined for neurovascular injury and other musculoskeletal injuries.
Lab Studies
If patients have preexisting conditions or comorbidities, then appropriate blood investigations are done.
Imaging
Plain X-rays
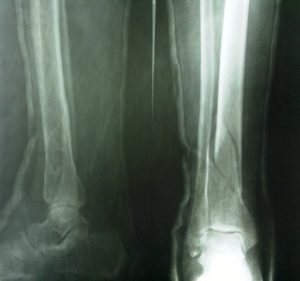
Plain x-rays include anteroposterior (AP), mortise, and lateral views centered over the ankle. Full-length radiographs of the leg, including the knee and ankle, help assess alignment and to rule out any other fractures in the limb.
Other regions of the body, such as the spine in the case of a fall from the height, may require radiographic evaluation, depending on clinical findings.
Traction radiographs [after application of spanning fixator] will yield a better understanding of the fracture anatomy.
CT
CT helps to understand the fracture better. Its 3D reconstruction especially is very useful to understand fracture fragments and their relation.
CT is most useful after ligamentotaxis is provided by a spanning external fixator [First span, then scan]
This provides a better understanding of the fracture pattern, the degree of comminution, the displacement, and the impaction of articular fragments that may not be evident on plain radiographs.
Angiography
Angiography is required if a vascular compromise is suspected.
Treatment of Pilon Fractures
Initial Management includes elevation and support of the limb by splintage, dressing of the wounds if present, NSAIDs and antibiotics.
Open fractures and those with vascular injury need to be operated immediately. For other fractures, the treatment may be conservative or operative.
Non-operative Treatment
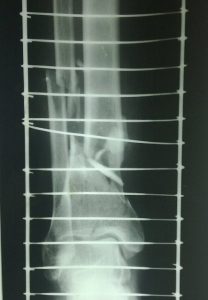
The non-operative treatment is by long leg cast for 6 weeks followed by fracture brace and range of motion exercises.
Non-operative treatment can be considered in stable fracture patterns without articular surface displacement, critically ill or nonambulatory patients or those with the risk of significant risk of skin problems.
It is less preferable to surgery because the loss of reduction is common and the monitoring of soft tissue injuries cannot be properly done.
Surgical Treatment
Indications for surgery include the following:
- Open fracture
- Displaced fracture with
- Articular fragments gap > 2 mm
- Step of more than 1 mm
- Rotational malalignment
- Vascular injury or compromise
- Compartment syndrome
The presence of soft-tissue swelling and/or blisters, peripheral vascular disease, and/or wound infection are contraindications for extensive surgery.
Arthroscopy may be used intraoperatively to aid visualization of the reduction.
Pilon fractures are frequently associated with soft tissue problems. Therefore most of these injuries cannot be operated early.
The nature and timing of surgery is dictated by
- Duration elapsed from injury
- Soft tissue condition
- Additional injuries
If there is a waiting period, preliminary stabilization is usually achieved with an external fixator which brings pain relief, the resolution of soft-tissue swelling and prevents contractures in soft tissue.
Definitive surgery is undertaken when the condition of soft tissues is optimized, marked by epithelization of blisters and wrinkling of the skin.
Different Surgical Options and Techniques
- External fixation (either spanning the ankle or not)
- Limited internal fixation with external fixation
- Open Reduction and Internal Fixation
If the fibula is fractured, it should be preferably operated
A cancellous(either autogenous or allograft or synthetic bone graft can be used to fill the resulting defect in the metaphyseal area during the reconstruction of articular part of the tibia.
Spanning external fixation across ankle joint
Ankle spanning external fixation can be used to provide acute fractures with significant joint depression or displacement to keep fragments in grossly aligned. The external fixator is left in place until the swelling resolves which usually takes 10-14 days.
External fixator can be used as definitive fixation as well when soft tissues condition won’t permit internal fixation.
The fixator could be joint-spanning articulated or nonspanning hybrid ring fixator
It can be combined with limited percutaneous fixation using lag screws.
Though associated with less soft tissue problems, the problems with external fixation include –
- pin and wire tract infections
- loss of ankle motion
- injury to neurovascular structures
- anatomic articular reconstruction may not be possible
Closed/Open Reduction and Internal Fixation

Lateral View
Internal fixation is the definitive fixation for the majority of pilon fractures. It can be done early if the soft tissue condition allows especially reduction and fixation with limited dissection.
Otherwise, the surgery could be delayed for soft tissues to heal.
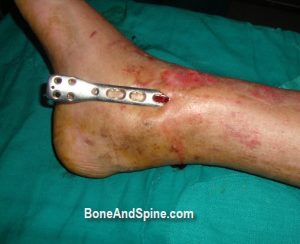
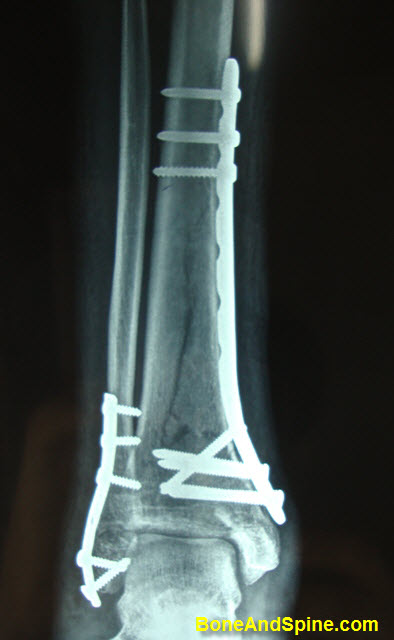
The approach to ankle varies on the type of fixation. The approach could be an anterior approach, anterolateral approach, anteromedial approach, medial approach posteromedial approach for tibia and lateral and posterolateral for fibula.
Internal fixation allows anatomic reduction of the articular surface, restoration of length, reconstruction of the metaphyseal shell and bone grafting.
The implants used in internal fixation are plates and screws.
Accurate reduction of the posterior fragment can be difficult through anteriorly placed approaches. In such situations, a posteromedial approach is added.
The anterior joint capsule is closed, but the anterior tibial fascia is left open to prevent postoperative compartment syndrome.
The skin should be closed under no tension.
A below-knee, posterior splint reinforced with two side splints is applied with the ankle held at 90°.
The leg is kept elevated. Regular observations are made to ensure early detection of a compartment syndrome. Active exercises are encouraged, and antithrombotic measures are instituted as necessary.
Patients are discharged home when comfortable. They should not bear weight on the operated leg until advised to do so.
Complications
- Wound Dehiscence
- Infection
- Varus malunion
- Nonunion
- Posttraumatic arthritis
- Chondrolysis
- Stiffness
Prognosis
Low-impact have better outcomes than high-impact pilon fractures. In general, good outcomes can be expected in approximately 60-80% of patients.
Many patients continue to improve for many years after the injury.
Ankle fusions may be required in approximately 3-27% of patients with posttraumatic arthritis.
References
- Cole PA, Mehrle RK, Bhandari M, Zlowodzki M. The pilon map: fracture lines and comminution zones in OTA/AO type 43C3 pilon fractures. J Orthop Trauma. 2013 Jul. 27(7):e152-6.
- Brumback RJ, McGarvey WC. Fractures of the tibial plafond. Evolving treatment concepts for the pilon fracture. Orthop Clin North Am. 1995 Apr. 26(2):273-85.
- Sands A, Grujic L, Byck DC, Agel J, Benirschke S, Swiontkowski MF. Clinical and functional outcomes of internal fixation of displaced pilon fractures. Clin Orthop Relat Res. 1998 Feb. 131-7.
- Ruedi TP, Allgower M. The operative treatment of intra-articular fractures of the lower end of the tibia. Clin Orthop Relat Res. 1979 Jan-Feb. 105-10.
- Watson JT, Moed BR, Karges DE, Cramer KE. Pilon fractures. Treatment protocol based on severity of soft tissue injury. Clin Orthop Relat Res. 2000 Jun. 78-90.
- Amorosa LF, Brown GD, Greisberg J. A surgical approach to posterior pilon fractures. J Orthop Trauma. 2010 Mar. 24(3):188-93.
- Syed MA, Panchbhavi VK. Fixation of tibial pilon fractures with percutaneous cannulated screws. Injury. 2004 Mar. 35(3):284-9
- Sirkin M, Sanders R. The treatment of pilon fractures. Orthop Clin North Am. 2001 Jan. 32(1):91-102
- Papadokostakis G, Kontakis G, Giannoudis P, Hadjipavlou A. External fixation devices in the treatment of fractures of the tibial plafond: a systematic review of the literature. J Bone Joint Surg Br. 2008 Jan. 90(1):1-6.
- Vives MJ, Abidi NA, Ishikawa SN, Taliwal RV, Sharkey PF. Soft tissue injuries with the use of safe corridors for transfixion wire placement during external fixation of distal tibia fractures: an anatomic study. J Orthop Trauma. 2001 Nov. 15(8):555-9.
- Sirkin MS. Plating of tibial pilon fractures. Am J Orthop (Belle Mead NJ). 2007 Dec. 36(12 Suppl 2):13-7.