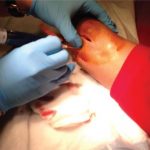
Methylene blue injection is an easy and safe way to rule out or confirm breakage of the joint capsule when there is an injury near or around the joint, thus establishing or ruling out the presence of open joint injury. Open joint injuries consist of are skin and soft-tissue injuries which communicate with the joint. It […]
Procedures
Radial Gutter Splint Indications and Procedure
A radial Gutter splint is a splint that is applied on the radial aspect of forearm and sandwiches 2nd [index]and 3rd [middle] fingers to provide both volar and dorsal support. Splints, as we know from our previous discussions are used to immobilize the injuries either temporarily or as definite treatment. Most common use of splints […]
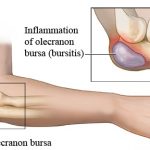
Aspiration of Olecranon Bursa
Aspiration of olecranon bursa is performed to obtain fluid for analysis. A bursa can become inflamed due to infection or for noninfective reasons like trauma, overuse, crystal deposition diseases etc. Non-infective or aseptic causes account for approximately two-thirds of all bursitis diagnoses. Infective or septic bursitis most commonly occurs due to seeding of bacteriae or […]
Ulnar Gutter Splint Application Procedure
An ulnar gutter splint extends from the proximal forearm to distal interphalangeal joints of fingers on the ulnar aspect of fingers wrist and forearm and is applied for various injuries of the ulnar aspect of the wrist and hand. It is also called Boxer splint. The splint is applied on the ulnar aspect and conforms to […]
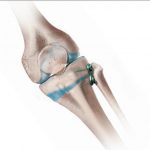
Eight Plate System for Epiphysiodesis
The Eight-figure plate or eight plate system or simply eight plate consists of the 2-holes plate and the 2 self-tapping screws and is used for control and correction of angular deformities like genu valgum or varus by a performing epiphysiodesis. Blount staples are the traditional most common implant used for hemiepiphysiodesis. This aims at stopping […]
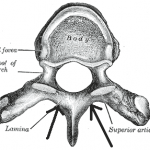
Laminectomy- Indications and Procedure
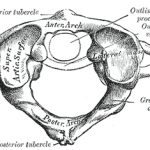
Laminectomy is a surgical procedure for decompressing the cord or nerve roots by removal of lamina part of the vertebra which forms the vertebral or neural arch. The vertebral arch is the ring of bone that joins the vertebral body to surround the spinal cord. [see anatomy] Each vertebra contains two laminae and the procedure […]
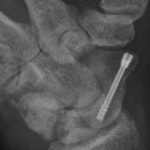
Internal Fixation of Scaphoid Fracture
Internal fixation of scaphoid can be done either percutaneously or using open reduction. In modern orthopedic practice, percutaneous fixation of the scaphoid is preferred where feasible because it is minimally invasive and there is no need for wide dissection and tissue injury caused by surgical dissection. Preoperative Planning The fracture pattern should be clear. Conventional […]
Surgery in Spinal Tuberculosis
Surgery in spinal tuberculosis is considered in the patients where the disease is not responding to the drug treatment, rest and other conservative measures. The aims of treatment of tuberculosis of the spine are: Control and cure of the existing active systemic and local infection and prevent its further spread. Achieving the stability of the […]
Tension Band Wiring Procedure
Tension band wiring is a procedure based on the tension band principle and uses K-wires/screws and SS wires for fracture fixation. Tension band wiring is commonly performed for patella and olecranon fractures. However, it can be done for many fractures including medial malleolus and greater trochanter fractures. In fact, it can be done for fractures […]
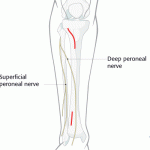
Different Surgical Approaches to Tibia
Surgical approaches to tibia are named according to the site of incision and the region accessed Anterolateral Approach to Tibia Indications This incision is the classical incision for plating of tibia or open reduction of tibial fractures. The entire tibia from knee to ankle may be exposed through this incision. It mobilizes the muscles of […]