Last Updated on November 20, 2019
Proximal tibia fractures refer to fractures of the upper portion of tibia below the knee. These fractures could be intra-articular or extra-articular. Intra-articular fractures are also called tibial plateau fractures and have been discussed separately.
This article would restrict to non-articular fractures of the proximal tibia. These fractures include metaphysic and diaphysis of the tibia and roughly include upper one-third of the tibia.
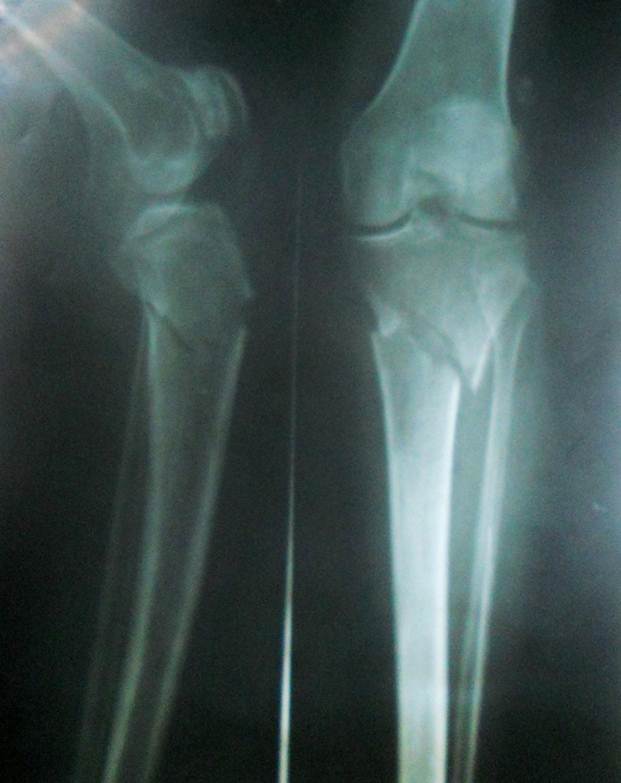
These fractures are different from tibial shaft fractures as the treatment approach and outcomes are different.
Like tibial plateau fractures, fractures of the proximal third of tibia are associated with severe soft tissue injuries.
Fractures of the proximal tibial shaft that are associated with high rates of malunion in valgus and procurvatum [apex anterior]
Fractures of proximal third of tibia account for 5-11% of all tibial shaft fractures.
These fractures may result from trauma, stress and any pathology that weakens the bone.
In young adults, the fractures occur often as a result of a high-energy injury, such as a fall from a considerable height, sports-related trauma, and motor vehicle accidents.
Such fractures are commonly associated with compartment syndrome.
Older persons have poor quality bone and often get fractures because of low-energy injury (fall from a standing position).
Anatomy of Upper Tibia
Tibia is broader at the proximal-most end and narrows distally.
It is triangular in cross section and has a wide metaphyseal region.
Muscles attached to the proximal tibia act as deforming forces after fracture. Thus patellar tendon causes proximal fragment into extension and causes the fragment to be apex anterior or procurvatum position.
Hamstring tendons cause flexion of the distal fragment. Pes anserinus causes varus position of proximal fragment. Muscles of the anterior compartment of the leg would cause valgus force.
Classification of Proximal Tibial Shaft Fracture [AO]
Type A
Simple fracture pattern
Type B
Wedge fracture pattern
Type C
Comminuted fracture pattern
Clinical Presentation
Patients present with pain and swelling of the injured region. Soft tissue injury may vary in severity, depending on the severity of the injury.
Some patients, especially those with a stress fracture or minimal trauma may present with pain and inability to bear weight
The examination would reveal swelling, contusions, blisters or open wounds depending on the severity of the injury.
Compartment syndrome can occur and should always be examined for.
Distal pulses and nerves should be examined and compared with the opposite side.
Imaging
X-rays
Anteroposterior and lateral views are basic x-rays. Oblique views may be considered when the fracture configuration is not clear.
Intra-articular extension of the fracture lines should be deliberately looked for. Tibia plateau integrity should always be checked.
AP and lateral views of ipsilateral ankle should always be included in the view
Computed tomography
It is not required in routine. It is quite sensitive to confirm or rule out an intra-articular fracture.
Treatment of Proximal Tibia Fractures
Open fractures and those with compartment syndrome require emergency surgery.
Nonsurgical treatment is indicated in undisplaced fractures or displaced fractures where patients are not suitable for surgery.
Surgery is indicated in displaced fractures.
Definitive treatment is by internal fixation. External fixation may be used for temporary fixation when soft tissue conditions do not permit early surgery.
Nonoperative Treatment
Closed reduction and cast immobilization is the standard non-operative method. Undisplaced fractures can simply be immobilized. Low energy fractures with acceptable alignment can be very well treated by non-operative methods
Following fracture, situations can be included
- < 5 degrees varus-valgus angulation
- < 10 degrees anterior/posterior angulation
- 50% cortical apposition
- < 1 cm shortening
- < 10 degrees rotational alignment
The patient is treated by a long leg cast followed by a functional brace at 4 weeks. The knee is kept in slight flexion.
Operative Treatment
All displaced fractures showing displacements/deformities more than mentioned for non-operative methods should be operated.
Definitive treatment is by either intramedullary nailing or fixation with plate preferably locking plate.
External fixation is indicated in fractures with extensive soft-tissue compromise and polytrauma. Often this choice is used as a temporary measure to maintain limb length until the soft tissue heals good enough for performing surgery or the patient can become stable enough to be operated.
Intramedullary Nailing

Intramedullary nailing can only be carried when there is enough proximal bone to accept two locking screws (5-6 cm). Improper patient selection or improper technique can lead to high rates of malunion.
Plate Fixation
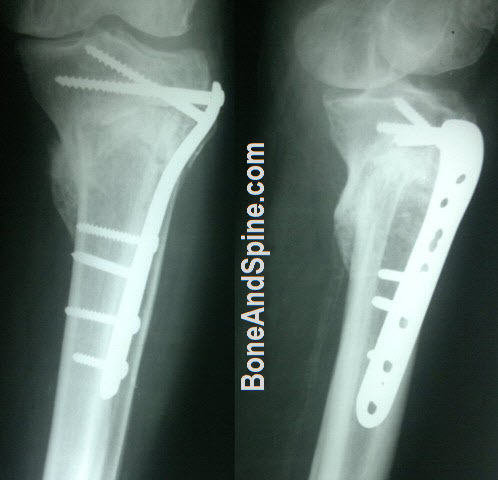
The preferred implant is locking proximal tibial plate which enables the surgeon percutaneous plating without extensively opening the fracture and with minimum soft tissue dissection.
It is best suited for transverse or oblique fractures. The plate may be used on the lateral side or media side [The plated differ in shape for medial and lateral sides. There are different plates for the left and right side.
The lateral plate is preferred because of better available soft tissue cover.