Last Updated on November 22, 2023
Shoulder impingement syndrome is said to occur when there is impingement of tendons of the rotator cuff and/or bursa in the shoulder in subacromial space [ from bones of the shoulder. Repeated impingement leads to irritation and inflammation of the structures irritated and inflamed as they pass through the subacromial space, the passage beneath the acromion. This can result in pain, weakness, and loss of movement at the shoulder.
Shoulder impingement syndrome is associated with the repeated overhead activity of the shoulder such as painting, lifting, swimming, tennis, and other overhead sports.
Shoulder impingement syndrome is also called painful arc syndrome, supraspinatus syndrome, and thrower’s shoulder.
Pathophysiology of Shoulder Impingement
The supraspinatus outlet is the space formed by acromion, coracoacromial arch, and acromioclavicular joint on the upper rim and the humeral head and glenoid below. It accommodates passage and excursion of the supraspinatus tendon. It is also called suprahumeral space or subacromial space.
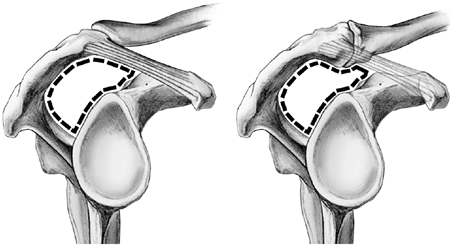
Abnormalities of the supraspinatus outlet or any pathology that causes further compromise [extrinsic compression] of the space and thus increased narrowing on raising the arm causes an impingement of the tendon resulting in impingement syndrome. When the humerus is placed in the forward-flexed and internally rotated position, it forces the greater tuberosity of the humerus into the undersurface of the acromion and coracoacromial arch causing further reduction of space.
Thickening or calcification of the coracoacromial ligament, loss of function of the rotator cuff muscles [cause the humerus to move superiorly], inflammation and thickening of the subacromial bursa may cause impingement.
Nonoutlet impingement occur due to loss of normal humeral head depression from
- A large rotator cuff tear
- Weakness in the rotator cuff muscles
- Thickening or hypertrophy of the subacromial bursa
Overuse or repetitive microtrauma in overhead activities as in swimming, baseball, volleyball, tennis or any vocation may cause shoulder impingement syndrome.
Secondary impingement is said to occur when there is a functional decrease in the supraspinatus outlet space due to the instability of the glenohumeral joint. It is the most common cause in young athletes with sports that require repeated overhead activities. This causes repetitive stresses on the static and dynamic glenohumeral stabilizers leading microtrauma and weakening of the glenohumeral ligaments and glenohumeral instability.
Instability places increased stress on rotator cuff tendons leading to tears and tendonitis. Due to the weakening of rotator cuff, the humeral head translates anteriorly and superiorly causing impingement. The treatment needs to address instability too.
Increased tensile stresses on the rotator cuff tendon due to abnormal glenohumeral joint motion is called glenoid impingement. This is believed to occur most commonly in throwing athletes.
Causes of Shoulder Impingement
| Primary Impingement | Secondary Impingement |
| Increased subacromial loading
A hooked acromion [type III] Os acromialeOsteophyte Calcific deposits in the subacromial space Acromioclavicular arthrosis leading to inferior osteophytes Hypertrophy of Coracoacromial ligament Prominent humeral greater tuberosity Trauma Overhead activity |
Rotator cuff overloadEccentric muscle overloadGlenohumeral instabilityWeakness of the long head of the biceps tendonGlenoid labral lesionsMuscle imbalanceScapular motion defectsTight posterior capsule
Paralysis of the trapezius muscle
|
Presentation of Shoulder Impingement Syndrome
Pain, especially on overhead activities, is the initial complaint. The pain may occur at night especially when the patient is lying on the affected shoulder. A grinding or popping sensation during movement of the shoulder may be present.
The range of motion at the shoulder may be limited by pain. A painful arc of movement may be present during forward elevation of the arm from 60° to 120°.
The pain is persistent and affects everyday activities. Reaching up behind the back or reaching up overhead may cause pain and interfere with daily activities.
With time, impingement syndrome can lead to inflammation of the rotator cuff tendons [tendonitis] and subacromial bursitis. If not treated appropriately, the rotator cuff tendons can start to thin and tear.
Impingement is generally seen in younger patients which if untreated may lead to tears in old age.
Tests for Impingement
Neer Test
The examiner performs maximal passive abduction in the scapular plane, with internal rotation, while the scapula is stabilized.
This causes impingement of supraspinatus tendon against anterior inferior acromion.
Hawkins-Kennedy Test
With patient sitting, the arm and elbow is flexed at to 90°, supported by the examiner. The examiner then stabilizes proximal to the elbow with their outside hand and with the other holds just proximal to the patient’s wrist. He then quickly moves the arm into internal rotation Pain and a grimacing facial expression indicate impingement of the supraspinatus tendon, and this is a positive Hawkins-Kennedy impingement sign.
Impingement Test
10 mL of a 1% lidocaine solution into the subacromial space and then repeats the tests for the impingement sign. Reduction of pain constitutes a positive impingement test result.
Drop Arm test
This evaluates for a supraspinatus muscle tear. In this test, the shoulder is abducted 90 degrees, flexed to 30 degrees and point thumbs down. The test is positive if the patient is unable to keep arms elevated after the examiner releases.
Supraspinatus Isolation Test
It is also known as empty can and full can test. The original test described by Jobe and Moynes to test the integrity of the supraspinatus tendon is called empty can test. Full Can Test was later suggested by Kelly as it was less provocative and tested in the same manner.
Empty can and full can represents the position. The patient is tested at 90° elevation in the scapular plane and full internal rotation (empty can) or 45°external rotation (full can).
In these positions, downward pressure exerted by the examiner at patients elbow or wrist. Muscle weakness or pain or both represent a positive test.
Tests for Instability
Sulcus sign
In this test, the examiner grasps the patient’s elbow and applies downward traction. Dimpling of the skin below he acromion (the sulcus sign) indicates inferior humeral translation. This indicates instability of the shoulder joint.
Anterior Drawer Test
With the patient in sitting position, one hand stabilizes the shoulder by holding coracoid and spine of scapula, and the other hand moves the humeral head anteriorly and posteriorly. Any abnormal movement is noted.
The Apprehension and Relocation Test
With the patient in supine position, the examiner brings the affected arm into an abducted and externally rotated position. If patient apprehensively guards and does not allow further motion, it indicates a positive anterior shoulder instability.
The test is repeated with shoulder supported anteriorly. The absence of guarding and pain confirms the instability.
Differential Diagnoses
- Acromioclavicular Injury
- Bicipital Tendonitis
- Brachial Plexus Injury
- Cervical Injuries/Cervical Discogenic Pain
- Infraspinatus Syndrome
- Myofascial Pain
- Rotator Cuff Injury
- Labrum Lesions
- Rotator Cuff Tendonitis
- Thoracic Discogenic Pain Syndrome
- Thoracic Outlet Syndrome
Imaging Studies in Shoulder Impingement Syndrome
Xrays are done to rule out glenohumeral/acromioclavicular arthritis and os acromiale.
AP view, internal rotation view of the humerus with a 20° upward and axillary view are most useful to rule out subtle signs of instability and to find an os acromiale.
Stryker notch view also let os acromiale be easily visualized.
Supraspinatus outlet view is used to assess the supraspinatus outlet space and anatomy of the acromion. [if supraspinatus outlet space 7 mm, the patient is more at risk for impingement syndrome.]
MRI is considered the imaging study of choice as it can detect structural changes and pathologies better.
Treatment of Shoulder Impingement Syndrome
Conservative treatment includes rest, restriction of painful activity, and physiotherapy. Rest, ice packs and NSAIDs help to ease the pain.
Corticosteroid injection of into the subacromial space relieves pain. Betamethasone, triamcinolone, and methylprednisolone are commonly used. These injections do not have a long-term effect and it is common for the pain to return. If required, another injection can be given after six weeks.
High-Intensity Laser Therapy
A small study has reported high-intensity laser therapy to be beneficial but further research is wanted.
Surgical Treatment of Shoulder Impingement Syndrome
If there is no improvement after three months of conservative treatment, the patient should be evaluated for surgery.
The patient should be examined under anesthesia and diagnostic arthroscopy should be done.
Before arthroscopy, the range of motion should be checked and if stiff, manipulation of the shoulder is performed. Arthroscopic subacromial decompression is generally not performed in patients with significant preoperative stiffness due to the increased risk of postoperative adhesive capsulitis.
Any instability present should be documented.
During arthroscopy, the integrity of all the structures is checked. If there is a partial tear in supraspinatus tendon, fragmented and torn tissue is debrided.
If there is no rotator cuff disruption, the coracoacromial ligament is smooth, subacromial space is adequate, then the diagnosis of subacromial impingement is unlikely. In this case, subacromial decompression is not performed.
If the patient has changes suggestive of impingement syndrome, subacromial decompression is performed by resecting anterior inferior portion of the acromion.
Patients with evidence of impingement perform better with surgery. Results of subacromial decompression are poor in young high-performance athletes.
After initial recuperation patient is put on stretch and range of motion exercises and gradually progress to strengthening exercises to enable the return to work or sports.