Last Updated on April 6, 2024
Proximal row carpectomy is a surgical procedure that involves the removal of bones of the proximal row of the wrist namely the scaphoid, lunate, triquetral, and in some cases radial styloid. It is a motion-sparing procedure.
Proximal row carpectomy converts complex wrist joint to a simple hinge joint creating a radiocarpal articulation and preserves about 60-80% of motion & 70-100% grip strength.
However, it has a disadvantage of relative lengthening of extrinsic tendons.
Indications
- Disabling wrist pain secondary to Scapholunate Advanced Collapse wrist
- Kienbock’s disease
- Scaphoid Nonunion
- Avascular necrosis of scaphoid
Proximal row carpectomy should not be done in severe degenerative changes and rheumatoid arthritis.
Wrist Arthroplasty and wrist fusion are two alternative procedures that must be considered and discussed with the patient.
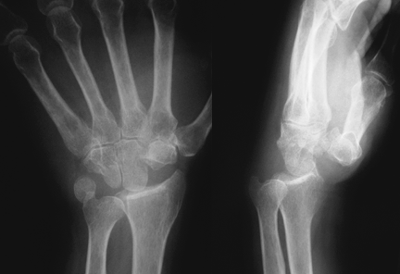
Technique of Proximal Row Carpectomy
The wrist is opened through a dorsal longitudinal approach through the third compartment. The radioscaphocapitate ligament is preserved to prevent ulnar subluxation after the procedure of proximal row carpectomy is performed.
After exposure, traction is applied to the index and long fingers, in a longitudinal direction. This tract facilitates the excision of the proximal carpal row. For bone removal, small rongeurs are used first to excise the middle of each bone. This allows the proximal and distal edges of the proximal carpal bones to collapse together. This makes the rest of the removal of the bones easy along their peripheral edges.
Injury to palmar wrist ligament, triangular fibrocartilage complex, capitate, and pisiform should be avoided. Passive flexion extension of the hand is done in neutral and slight radial deviation to detect impingement of the trapezium and the radial styloid. Some patients do require radial styloidectomy because of impingement.
The wound is closed and the wrist is immobilized in a well-padded plaster splint for 2 weeks.
Sutures are removed at 2 weeks, the patient is placed in a removable splint, and motion is started.
References
-
Wall LB, Stern PJ. Proximal row carpectomy. Hand Clin. 2013 Feb;29(1):69-78. [link]