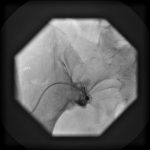
An intrathecal pain pump is a surgically implanted drug delivery system that sends pain medication directly to the spinal cord. This unique treatment option may be recommended to selected patients of chronic pain who have not experienced adequate pain relief from conservative approaches. The intrathecal pain pump is a small battery-powered, programmable pump which is […]
Pain Management
Ketamine Use in Pain Management – First Guidelines Published
Consensus guidelines for ketamine use in pain management have been developed jointly by the American Society of Regional Anesthesia and Pain Medicine, the American Academy of Pain Medicine, and the American Society of Anesthesiologists Ketamine is a drug that is used for the initiation and maintenance of anesthesia during invasive or non-invasive procedures. It produces […]
Postoperative Pain Management
Perioperative pain relief or postoperative pain management or postoperative analgesia deals with the treatment of pain that occurs after the surgery. Postoperative pain can be acute that occurs immediately after the surgery or chronic that occurs and continues over a period. This article mainly concentrates on acute postoperative pain and the term postoperative pain here […]
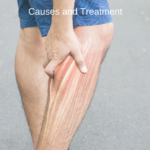
Myalgia or Muscle Aches – Causes and Treatment
Myalgia is a medical term for muscle pain. It is derived from the prefix my(o)-, meaning muscle, and the suffix –algia, which refers to pain or a painful condition. Muscle aches can be caused by diseases and disorders. It is a common complaint among adults presenting for medical care. Nearly everyone, at some point in […]
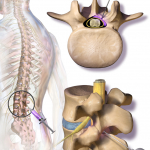
Epidural Steroid Injection Procedure
Epidural steroid injection, as the name implies, is a technique of injecting a steroid into the epidural space for relieving pain in the neck, arm, back, and leg, caused by inflamed spinal nerves due to spinal stenosis or disc herniation. An epidural steroid injection typically includes both a corticosteroid like methyl-prednisolone, dexamethasone or other […]
Sacroiliac Joint Injection Indications and Procedure
A sacroiliac joint injection is also called a sacroiliac joint block. It is primarily used either to diagnose or treat low back pain and/or sciatica symptoms associated with sacroiliac joint dysfunction. Relevant Anatomy The sacroiliac joint is an amphiarthrodial joint, formed between the auricular surfaces of the sacrum and the ilium. Interosseous ligament, the anterior […]
Selective Nerve Root Block – Indications and Applications
Selective nerve root block is similar in approach to facet joint injections but they address different pathologies. Both of these might be used in the same patient for the diagnostic purpose [to find if the pain is due to facet joint or nerve root] but as therapeutic measure, they address different issues. As in epidural […]
Meralgia Paresthetica
Meralgia paresthetica is an entrapment neuropathy of lateral femoral cutaneous nerve resulting in pain in the outer thigh. Lateral femoral cutaneous nerve is a sensory nerve that supplies the lateral aspect of the thigh. Meralgia paresthetica comes from the Greek words meros (thigh) and algos (pain). The compression of the nerve commonly due to focal […]
Hand Pain Causes and Treatment
Hand pain could be due to many causes many causes, including injury and disease. Fortunately, many of those causes can be treated and the symptoms eased. Here are some of the most common conditions that cause hand pain. But first an overview of the anatomy of hand. Anatomy of Hand Each hand contains 27 distinct […]
Platelet Rich plasma Therapy and its Uses
Platelet rich plasma is platelet plasma fraction of blood drawn from patient [autologous blood] which contains concentrated platelet and used as orthobiologics to treat many musculoskeletal conditions. Orthobiologics are biological substances that are used to help injuries to heal more quickly. Orthobiologics are used to improve the healing of fractures, injured muscles, tendons and ligaments. […]