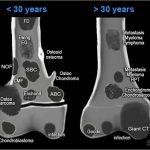
Juxtacortical tumors or surface tumors of bone are neoplasms [abnormal and excessive growth] arising from or just outside the cortex, and are composed of different histologic types. Some of the important juxtacortical tumors are Periosteal or juxtacortical chondroma Periosteal or juxtacortical chondrosarcomas Periosteal or juxtacortical osteosarcomas Types of Juxtacortical Tumors Juxtacortical tumors are divided into […]
Tumors
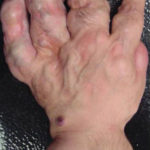
Maffucci Syndrome Features, Diagnosis and Treatment
Maffucci syndrome is a rare disorder is characterized by enchondromas, bone deformities with venous malformations with or without spindle cell hemangiomas. The condition was first reported by Maffucci in 1881. There is no racial or sexual predilection. It usually manifests early in life, usually around age 4-5 years. About one-fourth of the cases are congenital. But […]
Enchondromatosis – Types, Presentation and Differentiation
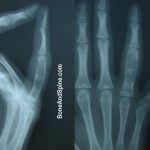
Enchondromatosis: insights on the different subtypes Enchondromatosis is the presence of multiple enchondromas. Enchondromas are benign, and often asymptomatic lesions of hyaline cartilage in the metaphyses and diaphyses of the short and long tubular bones of the limbs. They are especially common in hands and feet. They are often found as incidental lesions, usually solitary […]
Enchondroma – Features, Sites and Treatment
Enchondroma is a common intramedullary benign neoplasm composed of mature cartilage. It has limited growth potential, and a majority of enchondromas are small, asymptomatic lesions less than 3 cm in diameter. It is a type of chondroma that occurs within the medullary cavity. Enchondroma accounts for 12% to 24% of the benign bone tumor and […]
Chondroma – Presentation, Types, Diagnosis and Treatment
The term chondroma refers to a benign tumor of cartilage origin. The tumor contains cartilage cells that are similar to normal cartilage cells but contains vessels that differentiate it from normal cartilage. Chondromas may arise inside or outside the bone. These tumors are called enchondromas when they occur in the medullary canal of the bone. The […]
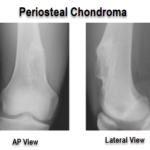
Periosteal Chondroma or Juxtacortical Chondroma
Periosteal chondroma is a benign cartilage tumor that develops on the surface of bone under the periosteum. It is also called as juxtacortical chondroma. Chondroma consists of mature hyaline cartilage. Periosteal chondromas are rare lesions and account for less than 1% of all chondromas. The majority of cases are diagnosed during the second and third […]
What is Chemotherapy for Tumors and How Does it work
Chemotherapy literally means treatment of a disease by drugs. But the term has become a synonym with chemotherapy of tumors. Tumor chemotherapy is one of the basic pillars of cancer treatment, others being surgery and radiotherapy form the basic pillars of cancer treatment. Tumor chemotherapy drugs are also called anti-neoplastic drugs. Chemotherapy works by killing […]
Musculoskeletal Tumors – Classification, Diagnosis and Treatment
Musculoskeletal tumors are a rare and diverse group of tumors. Benign bone and soft tissue tumors are 100 times more common than malignant tumors. The musculoskeletal system is made of skin and subcutaneous tissue, lymphatic tissue, vascular structures, musculoaponeurotic tissue, neurological structures, bone, and joints. Musculoskeletal tumors of different histological types can present with similar […]
Tumor Mineralization Patterns
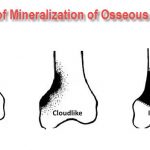
Tumor mineralization means deposition of additional mineral in and around focal lesions of bone. Tumor mineralization is seen as Mineralization of tumor matrix Reactive bone proliferation Mineral deposition in areas of degeneration or necrosis The characteristic mineralization patterns have diagnostic significance. Depending on the mineralization pattern, bone tumors and tumor-like conditions can be divided into […]
Enneking Staging System and TGNM Staging System for Musculoskeletal Tumors
Enneking Staging System and TGNM staging system are two main staging systems used for staging for benign and malignant tumors of the musculoskeletal system Many factors are involved in choosing the proper therapy for the patients. They include the stage of the disease, the expected functional result after surgery, the age of the patient, the […]