Last Updated on August 2, 2019
Myositis ossificans or heterotopic ossification is extra-skeletal ossification that occurs in muscles & other soft tissues. It affects the function of the normal soft tissues around bones and joints. Cases of heterotopic ossification causing ankylosis have been reported.
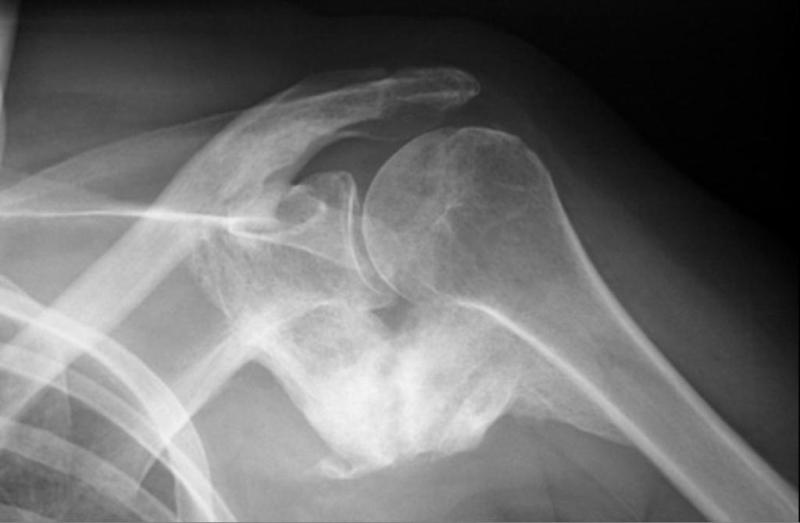
The term myositis ossificans is somewhat misleading. The condition is characterized by fibrous, bony and cartilaginous proliferation but can occur in sites other than muscles and inflammatory changes are rarely evident.
When muscles are involved, these are brachialis, quadriceps femoris and adductor muscles of thigh. If the ossification is located in the adductor muscles, it is known as “Prussian’s disease”.
Young athletic men are predisposed with myositis. Elbow region is the most commonly affected.
Myositis is also known by many other names such as
- Localized non neoplastic bone
- Myositis ossificans traumatica
- Myo-osteosis
- Myositis ossificans circumscripta
- Traumatic ossifying myositis
- Ossifying haematoma
The term heterotopic ossification is, therefore, is a better term that describes the condition and is increasingly being used. But the terms ectopic ossification and myositis ossificans are still used interchangeably with the term heterotopic ossification.
Types
Three types of heterotopic ossification have been described, as follows:
- Traumatic HO – This follows injury to tissue surrounding the bones and joints
- Myositis ossificans progressiva – a rare pediatric metabolic disease whereby skeletal muscle ossifies
- Neurogenic HO – This occurs as a result of burns or neurologic injury
Heterotopic ossification is the formation of mature lamellar bone in nonosseous tissue, whereas myositis ossificans is a specific type of heterotopic ossification that occurs in inflammatory muscle. Both of these processes are examples of ectopic ossification, and they may coexist.
Pathophysiology and Causes
The process involves alteration within the ground substance of connective tissue, and there is a intense proliferation of fibroblasts and mesenchymal cells .
The specific cause and pathophysiology are not clear. Heterotopic ossification may be caused by an interaction between local and unknown systemic factors which leads to the inappropriate differentiation of fibroblasts into bone-forming cells (osteoblasts).
Osteogenic cells begin to form osteoid. Bone morphogenic protein is believed to be important mediator.
Migrated bone marrow cells have been suggested as a potential cause of osteogenesis in connective tissue. Muscle lesions or interstitial hemorrhagic are thought to be a potential cause of muscle degeneration, perivascular connective tissue proliferation, and subsequent bone metaplasia.
The cause of heterotopic ossification is, to some extent, determined by the type.
Myositis ossificans progressiva is rare genetic disease that accounts for accounts for the metabolic disease in children.
Neurogenic heterotopic ossification may occur after
- Head injury
- Spinal cord injury
- Infections of the central nervous system
- Tetanus
- Polio
- CNS tumors
- Multiple sclerosis
- Cerebrovascular accidents.
Traumatic heterotopic ossification is due to trauma to bones and joints which might be caused by injury or surgery.
Risk factors for Acquired Heterotopic Ossification
- Trauma
- Burns
- Neurologic injury
- Previous heterotopic ossification
- Hip and pelvic surgery including arthroplasty
- Male sex
- Advanced age (>60 years)
- Genetic predisposition
- Higher risk in
- Diffuse idiopathic skeletal hyperostosis
- Paget disease
- Hypertrophic osteoarthritis
- Ankylosing spondylitis
- Children with cerebral palsy
- Higher risk in
- Preexisting hip fusion
- Posttraumatic arthrosis
- Surgical technique
- Prolonged surgery
-
- Presence of pressure sores near the surgical field
- Amount of bone resected
- Amount of soft tissue dissected
- Persistence of bone debris
- Prolonged soft-tissue retraction
- Presence of devitalized tissue
- Presence of hematoma/ wound infection/ prolonged wound drainage
Traumatic Heterotopic Ossification
Traumatic heterotopic ossification occurs in 10-20% of predisposed patients. Following total hip arthroplasty and acetabular fracture surgery, the incidence can be 2-63%.
History and Physical Examination
There is often history of trauma or surgery. The condition can be a cause of physical symptoms or the condition may be entirely asymptomatic and may be detected radiologically on follow-up films
A person who has symptomatic heterotopic ossification may present
- Restricted range of movement
- Pain in the muscle when you use it
- A hard lump in the muscle
- Incidental finding on x-ray
In severe cases, joint ankylosis may result. Nerve entrapment across joints also occur.
Laboratory Studies
Alkaline phosphatase levels indicate ongoing osteoblastic activity.
Imaging Studies
Plain radiographs are useful in the diagnosis.
For hip, Brooker developed a grading system.
- Grade I – Appearance of islands of bone within the tissues
- Grade II – Spurs of bone emanate from either the femur or the pelvis, with gaps of more than 1 cm between these spurs
- Grade III – Gaps between spurs are less than 1 cm
- Grade IV – Apparent ankylosis of the hip caused by the heterotopic ossification
Schmidt and Hackenbroch classification is more extensive where The number denotes the site and letter the extent.
- Region I – Heterotopic ossifications are strictly below the tip of the greater trochanter
- Region II – Heterotopic ossifications are below and above the tip of the greater trochanter
- Region III – Heterotopic ossifications are strictly above the tip of the greater trochanter
- Grade A – Single or multiple heterotopic ossifications are less than 10 mm in maximal extent without contact with the pelvis or the femur
- Grade B – Heterotopic ossifications are greater than 10 mm without contact with the pelvis but with possible contact with the femur; there is no bridging from the femur to the proximal part of the greater trochanter and no evidence of ankylosis
- Grade C – Ankylosis by means of firm bridging from the femur to the pelvis is present
It takes about 2 weeks for heterotopic ossification to be visible on the x-ray. Computed tomography or bone scans may detect this condition sooner.
Treatment of Myositis
Non operative Treatment
Treatment is initially conservative. Some calcifications will spontaneously be reabsorbed, and others will have minimal symptoms.
Here are treatment modalities
- Rest
- Immobilization
- Anti-inflammatory drugs
- Physiotherapy
- pulsed Ultra sound and phonophoresis
- Iontophoresis with 2 % acetic acid solution.
- Extra corporeal shock wave therapy
Surgical Therapy
Heterotopic ossification is seldom excised. This is because pain relief is often inadequate and improvement in range of motion may not last
Excision may be indicated on the basis of pain, nerve entrapment, and stiffness.
Heterotopic ossification is often thought to take approximately 12 months to mature. The lesion should be removed after maturation but has been done effectively at 3 and 6 months after trauma.
Growth should not be removed in premature stage as it will likely reoccur.
Prevention of Heterotopic Ossifications
During surgery, following precautions could help
- Meticulous exposure
- Careful soft tissue handling
- Adequate irrigation
- Efficient hemostasis
- Postoperative anticoagulation
After procedures, prophylaxis with nonsteroidal anti-inflammatory drugs such as indomethacin, or aspirin like for 6 weeks after the procedure may reduce the risk.
Radiation therapy may be effective if given up to 24 hours preoperatively or within 72 hours postoperatively.
Myositis ossificans Progressiva
Myositis ossificans progressive now termed as Fibrodysplasia ossificans progressiva is a rare [~1 per 2 million.], inherited disorder characterised by progressive fibrosis and ossification of muscles, tendons, fasciae, aponeuroses, and ligaments of multiple sites.
Most cases arise from sporadic mutations, although some are inherited in an autosomal dominant fashion. The process and symptoms of heterotopic ossification starts between 2 and 5 years old.
Characteristic features include:
- Hallux valgus
- Monophalangic first toe
- Shortened metacarpals
- Pseudoexostoses (ossification of ligamentous insertions)
- Microdactyly of the first metacarpal/metatarsal
- Neck muscle oedema
- C2-C7 facet joint fusion
Treatment and prognosis
This is a progressive, fatal disease with the median survival being 45 years.