Last Updated on October 29, 2023
Tuberculosis of foot is rare and constitutes less than 10% of cases of osteoarticular tuberculosis.
Calcaneum is the most common bone involved followed by subtalar joint and midtarsal joints.
Pathophysiology
Bonewise, the order of involvement in decreasing order is calcaneum, talus, first metatarsal, navicular, first and second cuneiforms cuboid and others.
The infection first lodges into the foot via the bloodstream. Endarteritis of the nutrient artery in such lesions is common. The disease may spread to neighboring structures once the intertarsal joints are involved, due to intercommunicating synovial channels or joint cavities.
Isolated lesions of tarsal and metatarsal bones may also occur.
Relevant Surgical Anatomy of Foot
The foot is formed by tarsal and metatarsal bone. Talus, calcaneum, navicular, cuboid and three cuneiforms form tarsal bones. Five metatarsals and their respective phalanges complete the skeletal parts of the foot.
The talus which also participates in the formation of ankle joint also forms gliding synovial joint with the calcaneum below. It also articulates distally with navicular.
Distally, calcaneum forms the calcaneocuboid joint which lies lateral to but in the same transverse plane as the talonavicular joint. Together these are described as transverse tarsal or midtarsal joint. Medial to the cuboid and distal to the navicular are situated the cuneiform bones and their articulations.
Synovial cavities of tarsal joints frequently communicate with one another. This makes the spread to disease to multiple joints and bones.
Foot allows inversion and eversion movements at talocalcaneal, talonavicular, and calcaneocuboid joints [hind foot]. At the intertarsal joints and distal joints of the foot, the principle movement is gliding to provide plantarflexion and dorsiflexion of the distal part of the foot.
Types of Lesions
Five types of lesion have been noted in foot tuberculosis as seen on x-ray.
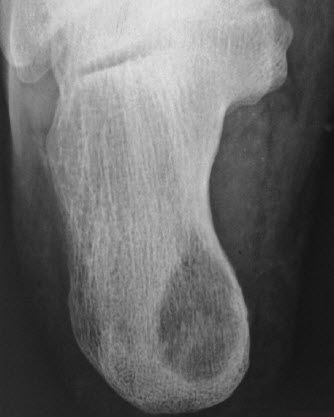
Cystic
A well-defined radiolucent area with loss of trabeculae in the middle of the bone, but no sequestrum. Usually seen in calcaneum.
Rheumatoid
There is a loss of articular cartilage and osteoporosis of all the tarsal bones.
Subperiosteal
There is subperiosteal scalloping of bone. Usually seen in cuboid bone, the base of the fifth metatarsal and the head of the talus.
Kissing
Symmetrical scalloped lesions across a joint on the articular surfaces of the bones.
Spina ventosa
Spina ventosa is generally seen in children and involves short tubular bones like metatarsals and phalanges.
Spina ventosa is a spindle-shaped expansion of the bone with successive layers of periosteal new bone.
Clinical Presentation of Foot Tuberculosis
There is a pain in the foot which may be accompanied by swelling. The pain is insidious in onset and may not be very severe in nature. The patient may not seek medical consultation for a long time.
On examination, there would be swelling of the affected area and part is tender to touch.
The cold abscess may be present in nearby areas. Sometimes sinuses can be seen.
Investigations
Diagnosis is early made by the presence of pain, swelling, tenderness and cold abscess/sinuses.
Xrays may be normal initially. X-rays reveal osteoporosis, areas of bone destruction and cavitation.
Phemister’s triad of periarticular osteoporosis, marginal erosions, and narrowing of the joint space is the radiological feature of osteoarticular tuberculosis.
The ESR is almost always elevated.
Demonstration of acid acid-fast mycobacteria from these lesions is difficult due to the paucibacillary nature of tuberculosis.
A biopsy may be sometimes required to reach at the diagnosis.
MRI can demonstrate lesions in and adjacent to the bone before they are visible on plain radiography.
Diagnosis
In endemic regions, the diagnosis of tuberculosis can be safely deduced from the clinical features, radiological appearance, and elevated ESR.
In nonendemic regions, histopathological examination or microbiological confirmation should be mandatory.
Differential Diagnosis
- Rheumatoid arthritis
- Gout
- Neuropathic joints
- Sarcoidosis
- Neoplasms
- Fungal Infection
- Brucellosis
- Sarcoidosis.
Treatment of Tuberculosis of Foot
Antitubercular drugs are the basis of treatment. Surgery is an adjunct and not usually required in most of the cases.
Along with drugs, below knee plaster cast or a below knee orthosis is advised.
As the healing progresses, spontaneous bony fusion may occur in the involved joints especially in cases with superadded infection.
Surgical treatment may be desirable in patients who do not respond.
Clinical signs of healing included a decrease in pain and swelling, disappearance of sinuses, improvement in gait and gain in body-weight. Clinical signs occur by six weeks or so.
These signs precede the radiological signs of healing which become evident by 3-6 months.
The radiological evidence of healing includes a decrease in osteoporosis with repair of scalloped lesions and focal sclerosis.
Surgery
Surgery is required in cases which do not heal by antitubercular drugs and rest.
Surgical options are
Surgical excision of a large isolated lesion
This, for example, is done in calcaneum to prevent the involvement of adjacent joints
Debridement
In cases where the lesions do not heal in spite of antitubercular drug treatment. Sometimes, the surgery just involves resection of a sequestrum. Other times curettage is done to take out the necrotic material.
In rare cases, whole diseased bone is resected.
Arthrodesis
Arthrodesis means fusion across joints. Two major types of arthrodesis in foot TB are triple arthrodesis, also called subtalar arthrodesis and pantalar arthrodesis.
Triple arthrodesis involves fusion of talocalcaneal, calcaneocuboid and talonavicular joints. In pantalar arthrodesis, the ankle joint is also fused in addition to this.
Sometimes, in the rheumatoid type of lesion, loss of the medial longitudinal and transverse arches of the foot occurs due to destruction of the intertarsal ligaments and tarsal bones leading to misshapen and stiff foot.
This kind of stiff and painful foot needs arthrodesis.