Last Updated on October 29, 2023
Radiation therapy is a form of cancer treatment which uses high-energy radiation such as X-rays, gamma rays, and charged particles to shrink tumors and kill cancer cells.
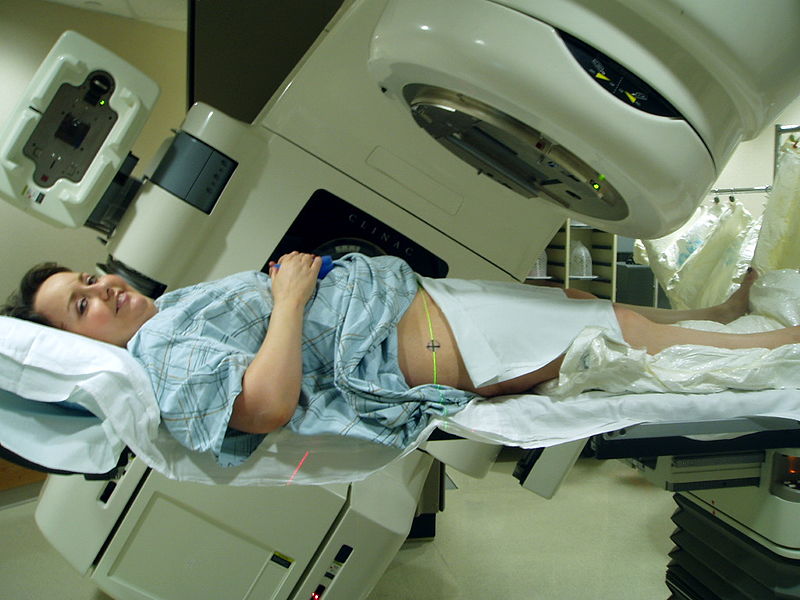
The radiation may be delivered by an external machine external-beam radiation therapy or by material placed in the body near cancer cells (internal radiation therapy, also called brachytherapy).
Radiation therapy is a local treatment, in contrast to chemotherapy, which is a systemic treatment affecting the whole body.
Radiation therapy may be used alone or in combination with surgery, chemotherapy, or both.
A patient may receive radiation therapy before, during, or after surgery.
How Does Radiation Therapy Work?
Radiation therapy kills cancer cells by damaging their DNA either directly or by creating charged particles or free radicals within the cells that can in turn damage the DNA.
Affected cells stop dividing and die.
Radiation therapy may be
Curative
This aims to cure the tumor or prevent recurrence after tumor removal.
Palliative
This aims to control symptoms only and there is no intent to cure the symptoms. This is done in incurable tumors.
The dose of radiation is measured in a unit called a gray [Gy] and measures the amount of radiation energy absorbed by 1 kilogram of human tissue.
The dose of radiation varies with the type of tumor and the part of the body involved.
When delivering the dose, the area selected for radiation usually includes the whole tumor plus a small amount of normal tissue surrounding the tumor to neutralize the microscopic local spread.
Types of Radiation Therapy
or from radioactive material placed in the body near cancer cells (internal radiation therapy, more commonly called brachytherapy). Systemic radiation therapy uses a radioactive substance, given by mouth or into a vein, that travels in the blood to tissues throughout the body.
External-beam
Radiation can come from a machine outside the body (linear accelerator)
It is most often delivered in the form of x-rays or gamma rays.
linear accelerator. This creates high-energy radiation that may be used to treat cancer.
Following types of external beam radiation therapy are used –
3-dimensional conformal
It uses a sophisticated computer software and advanced treatment machines for precise delivery of radiation.
Intensity-modulated
It uses collimators of devices that shape beams allowing for different areas of a tumor to receive different doses of radiation.
Image-guided
Repeated imaging like CT, MRI, or PET is performed during treatment. The computers process this information and adjust the position of the patient or the planned radiation dose, increasing the accuracy of radiation treatment.
Tomotherapy is an example which uses the machine which is a hybrid between CT imaging scanner and an external-beam radiation therapy
Stereotactic radiosurgery
Stereotactic radiosurgery is used to treat only small tumors with well-defined edges, most commonly in the brain or spinal tumors.
Proton therapy and electrons may also be used instead of photons. Electron beams are used to irradiate superficial tumors, such as skin cancer
Internal Therapy
Internal radiation therapy is also called (brachytherapy. It delivers the radiation by placing radioactive materials inside or on the body by using delivery devices, such as needles, catheters, or some other type of carrier.
Brachytherapy may be able to deliver higher doses of radiation to some cancers than external-beam radiation therapy while causing less damage to normal tissue.
Types of brachytherapy are
Interstitial brachytherapy
This places a radiation source within tumor tissue, such as within a prostate tumor.
Intracavitary brachytherapy
It uses a source placed within a surgical cavity or a body cavity, such as the chest cavity, near a tumor.
Episcleral brachytherapy
It is used to treat melanoma inside the eye, uses a source that is attached to the eye.
In brachytherapy, while the radioactive material is inside the body, the patient is radioactive [in contrast to external radiotherapy which does not make patient radioactive].
however, as soon as the material is removed, the patient is no longer radioactive. For temporary brachytherapy, the patient will usually stay in the hospital in a special room that shields other people from the radiation.
Systemic Therapy
A radioactive substance is ingested orally or given by an injection. For example swallowing of radioactive iodine or a radioactive substance bound to a monoclonal antibody.
Side effects of Radiation Therapy
Acute
The side effects occur during treatment and depend on the area of the body being treated, the radiation dose and the patient’s general medical condition.
These are caused by damage to rapidly dividing normal cells in the area being treated.
Examples are damage to the salivary glands or hair loss in head or neck area therapy or urinary problems when the lower abdomen is treated.
Most acute effects disappear after treatment ends, though some like salivary gland damage can be permanent.
The radioprotective drug amifostine helps to protect normal tissues from radiation during treatment.
Fatigue and nausea may occur irrespective of the part of the body treated.
Late
Depending on the area of the body treated, late side effects can include (1):
- Fibrosis
- Damage to the bowels, causing diarrhea and bleeding.
- Memory loss.
- Infertility
- Radiation exposure tumor
These adverse effects are not seen across all the patients.
References
- Gaspar LE, Ding M. A review of intensity-modulated radiation therapy. Current Oncology Reports 2008; 10(4):294–299.
- Veldeman L, Madani I, Hulstaert F. et al. Evidence behind use of intensity-modulated radiotherapy: A systematic review of comparative clinical studies. Lancet Oncology 2008; 9(4):367–375. Erratum in: Lancet Oncology 2008; 9(6):513.
- Noda SE, Lautenschlaeger T, Siedow MR, et al. Technological advances in radiation oncology for central nervous system tumors. Seminars in Radiation Oncology 2009; 19(3):179–186.
- Kavanagh BD, Timmerman RD. Stereotactic radiosurgery and stereotactic body radiation therapy: An overview of technical considerations and clinical applications. Hematology/Oncology Clinics of North America 2006; 20(1):87–95.
- Lam MG, de Klerk JM, van Rijk PP, Zonnenberg, BA. Bone seeking radiopharmaceuticals for palliation of pain in cancer patients with osseous metastases. Anti-cancer Agents in Medicinal Chemistry 2007; 7(4):381–397.
- Connell PP, Hellman S. Advances in radiotherapy and implications for the next century: A historical perspective. Cancer Research 2009; 69(2):383–392.
- Calvo FA, Meirino RM, Orecchia R. Intraoperative radiation therapy first part: Rationale and techniques. Critical Reviews in Oncology/Hematology 2006; 59(2):106–115.