Last Updated on November 12, 2019
Bacterial arthritis is infectious arthritis caused by the invasion of the joint space by bacteriae.
The bacteria enters the joint from the bloodstream, from a contiguous site of infection in bone or soft tissue. In trauma, surgery or invasive procedures, the bacteria might directly be inoculated in the joint, or by direct inoculation during surgery, injection, or trauma.
Pathophysiology
Synovial capillaries, lack the natural barrier of basement membrane which allows infiltration of the joint with bacteria. Within hours of bacteriae entering the joint, neutrophilic reaction begins in the synovium,the membrane that lines the joint.
Neutrophils and bacteria enter the lumen of the joint, and bacteria adhere to articular cartilage.
Degradation of cartilage begins within 48 hour due to following factors
- Increased intraarticular pressure
- Release of proteases and cytokines from chondrocytes
- Invasion of the cartilage by bacteria and inflammatory cells.
Synovial proliferation results in the formation of pannus over the cartilage, and thrombosis of inflamed synovial vessels develops.
Pathogens
Infants
- Group B streptococci
- Gram-negative enteric bacilli
- S. aureus
In a child vaccinated for H influenzae
- Staphylococcus aureus
- Streptococcus pyogens (group A streptococcus)
Young Adults
- N. gonorrhoeae [most commmon]
- Staphylococcus aureus [most common nongonococcal bacteria]
- Gram-negative bacilli.
Surgical procedures or penetrating injuries
- Staphylococcus aureus
- aGram-negative bacilli.
Infections with coagulase-negative staphylococci are unusual except after the prosthetic joint surgery or arthroscopy.
Anaerobic organisms, often in association with aerobic or facultative bacteria, are found after human bites and when decubitus ulcers or intraabdominal abscesses spread into adjacent joints.
Polymicrobial infections refers to when there are multiple pathogens infecting the lesion. These complicate traumatic injuries with extensive contamination. Pasteurella multocida has been noted in cat bites.
Presentation of Bacterial Arthritis
Ninety percent of patients present with involvement of a single joint.
Infections of the spine, sacroiliac joints, or sternoclavicular joints are more common in intravenous drug abusers.
Infection involving multiple joints is most common among patients with rheumatoid arthritis and may resemble a flare of the underlying disease.
In the affected joint, there is moderate to severe pain accompanied by joint effusion, muscle spasm and decreased range of motion.
There is also high-grade fever. Fever may not be present in patients with rheumatoid arthritis, renal or hepatic insufficiency, or conditions requiring immunosuppressive therapy.
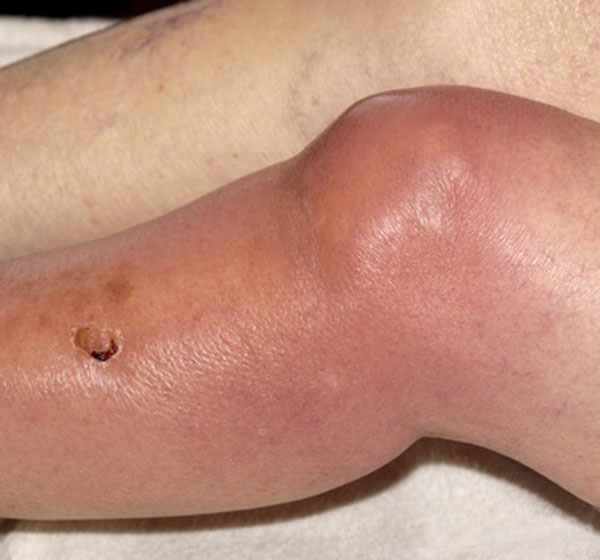
The joint on examination is inflamed and swollen. Joint is kept in the attitude of maximum joint space. For example in knee joint bacterial arthritis, the knee is kept in mild flexion.
Lab Studies
Complet blood count shows an increase in the number of white blood cells [leukocytosis] particularly, neutrophils. Inflammation markers like ESR and CRP are very high.
Specimens of peripheral blood and synovial fluid should be obtained before antibiotics are administered.
Blood cultures are positive in up to 50 percent of S. aureus infection but are less frequently positive in infection due to other organisms.
The synovial fluid is turbid, serosanguineous(blood mixed), or frankly purulent [Compare with normal fluid]
Gram-stained smears confirm the presence of large numbers of neutrophils.
Organisms are seen on synovial fluid smears in nearly 75% of infections with Staphylococcus aureus and streptococci but lesser infections due to gram-negative and other bacteria. Synovial fluid cultures are positive in more than 90 percent of cases.
Imaging
Plain radiographs show evidence of soft tissue swelling, joint space may be widened, and there is displacement of tissue planes by the distended capsule. Narrowing of the joint space and bony erosions indicate advanced infection and a poor prognosis.
Ultrasound is useful for detecting effusions.
Computed tomography or magnetic resonance imaging can demonstrate the status of joint structures.
Treatment
Once the bacterial arthritis is diagnosed, the patient should receive systemic antibiotics immediately and drainage of the involved joint is done on an urgent basis.
These measures are very important to prevent the destruction of cartilage, degenerative arthritis, joint instability, or deformity.
Antibiotics are given by intravenous route. Third-generation cephalosporin such as cefotaxime (1 g every 8 hourly) or ceftriaxone (1 to 2 g every 24 hourly) and an aminoglycoside will provide adequate coverage.
Intravenous vancomycin should be given if methicillin-resistant S. aureus is a possibility. In addition, an aminoglycoside should be given to intravenous drug users or other patients in whom Pseudomonas aeruginosa may be the responsible agent.
Definitive therapy is based on the identity and antibiotic susceptibility of the bacteria isolated in culture.
Drainage of pus is often required, unless the infection has been identified very early. Pus and necrotic debris from the infected joint is removed.
Needle aspiration, arthroscopic drainage, and lavage may be employed initially.
In some cases, open joint drainage or arthrotomy is necessary to remove loculations and debride infected synovium, cartilage, or bone
Septic arthritis of the hip is best managed with arthrotomy, particularly in young children, in whom infection threatens the viability of the femoral head.
Immobilization is not required after drainage and active mobilization should be done after pain is tolerated.
Antibiotics are given for at least six weeks.
Complications
- Residual arthritis
- Joint dislocation
- Ankylosis
- Pathological fracture
- Septicemia
- Contiguous osteomyelitis