Last Updated on October 29, 2023
Clavicle fracture is often caused by a fall onto an outstretched hand, fall onto the shoulder, a direct blow to the shoulder. Eighty-seven percent get fracture clavicle due to fall onto the shoulder.
Direct trauma to clavicle can occur with either blunt or penetrating trauma. Sporting activities that may result in direct trauma to the clavicle include bicycling and skiing. Bicycling accidents were the most common cause of clavicle fractures in both sexes.
Pathologic fractures can occur in the clavicle and stress fractures of the clavicle have been reported especially in people involved in repetitive upper limb activity.
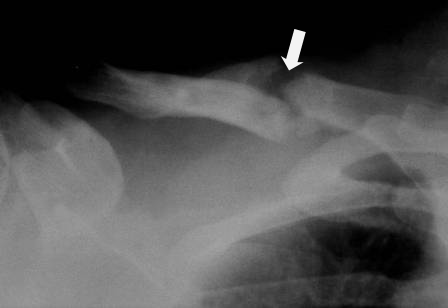
Classification of Clavicle Fracture
Allman Classification
Allman separated clavicle fractures into three groups:
Group I- Middle third fractures
Group II – Lateral third fractures
Group III – Medial third fractures
Although helpful in terms of localizing the injury, the system does not describe displacement, comminution, or shortening which have bearing on treatment and prognosis.
Craig gave a more descriptive and functional information and also included more unusual injuries.
Craig Classification of Clavicle Fractures
Group I – Fracture of the middle third
Group II – Fracture of the distal third
- Type I – Minimal displacement (interligamentous)
- Type II – Displaced secondary to fracture line medial to the coracoclavicular ligaments
- A) conoid and trapezoid attached
- (B) conoid torn, trapezoid attached
- Type III – Fractures of the articular surface
- Type IV – Periosteal sleeve fracture (children)
- Type V – Comminuted with ligaments attached neither proximally nor distally, but to an inferior comminuted fragment
Group III – Fractures of the proximal third
- Type I – Minimal displacement
- Type II – Displaced (ligaments ruptured)
- Type III – Intraarticular
- Type IV – Epiphyseal separation (children and young adults)
- Type V – Comminuted
Presentation of Clavicle Fracture
Most patients will give a history of a fall directly onto the shoulder. It can be a history of injury of a simple fall, fall from a height, fall during a sporting activity, or a motor vehicle accident.
Abrasions, ecchymosis, and deformity are usually apparent. Skin tenting may be present and should be looking for as it might change the treatment.
Associated fracture of the ipsilateral scapula and upper ribs can occur. The prevalence of pneumothorax in association with a clavicle fracture is 3%.
Injury to the brachial plexus in conjunction with a clavicle fracture has also been reported.
Vascular injuries associated with a clavicle fracture, although rare, have also been reported and may be life or limb threatening.
Imaging
AP radiograph of the clavicle is usually sufficient. An apical oblique radiograph is helpful obtained by placing a bump or roll the contralateral scapula with beam angled 20 degrees cephalad gives a better view.
Medial fractures are not that well visualized in routine x-rays and might need computed tomography.
An axillary radiograph may be useful to adequately define intra-articular fractures and, to ensure the integrity of the coracoid process. A chest x-ray may be done to rule out chest injuries.
Before planning for surgery of lateral clavicle fractures, a Zanca radiograph taken with the patient standing and the affected arm hanging to gravity is a done for better visualization of the fractures.
Treatment of Clavicle Fracture
Medial Fractures
Most authors report good results after nonoperative treatment. However, posterior displacement that threatens neurovascular structures should be managed surgically. Displaced fractures displacement combined with spinal accessory palsy, operative fixation of the clavicle should be considered.
Midshaft Clavicle Fractures
Immobilization
The nonoperative treatment produces good results but not all midshaft clavicle fractures heal with nonoperative treatment. Clavicle fractures with greater than 20 mm of shortening are highly predisposed to develop a nonunion.
Sling, strapping, or a combination of the two have been recommended for immobilization.
Most midshaft clavicle fractures will go on to healing with any method of immobilization.
Immobilization is discontinued when there is no pain or palpable fracture motion on scapular elevation and retraction. Usually, no subsequent therapy is necessary.
Some authors also recommend closed reduction before immobilization. It can be done in the supine position by placing a pillow between the scapulae while the shoulders are manipulated superiorly and laterally. In the sitting technique, a knee is placed between the scapulae and a sheet is used, in a configuration similar to a figure-of-eight bandage, to pull the scapulae outward.
External Fixation
External fixation is the best for open fracture or severe bruising and displacement with the risk of soft-tissue necrosis.
Open Reduction, Internal Fixation
Open surgical treatment of midshaft fractures for fall into two main groups: intramedullary devices and plate fixation.
Intramedullary fixation procedure is easy, carries minimal soft-tissue disruption, and satisfactory rates of healing whereas open reduction and plate fixation have the advantage of rigid fixation, cortical compression, and rotational control.
Indications for surgery
Absolute Indications
- Shortening of >20 mm
- Open injury
- Impending skin disruption and irreducible fracture
- Vascular compromise
- Progressive neurologic loss
- Displaced pathologic fracture with associated trapezial paralysis
- Scapulothoracic dissociation
Relative Indications
- Displacement of >20 mm
- Neurologic disorder like Parkinsonism, seizures
- Head injury
- Polytrauma
- Expected prolonged recumbency
- Floating shoulder
- Intolerance to immobilization
- Bilateral fractures
- Ipsilateral upper extremity fracture
Surgical procedure for a midshaft clavicle fracture.
Lateral Clavicle Fracture
Nonoperative treatment of most displaced lateral fractures does well and most patients would have a reasonable function after closed treatment, even in the presence of nonunion. The treatment consists of immobilization.
Type I and Type III distal clavicle fractures are treated nonoperatively in a simple sling. For Type II fractures, operative fixation is preferred.
The general choices for surgical goals are as follows:
- Direct fixation of the fracture site without coracoclavicular stabilization
- Direct fixation of the fracture site with coracoclavicular stabilization
- Coracoclavicular stabilization with or without excision of the lateral clavicular segment
Techniques of surgical repair of distal clavicle fractures.
Unusual Patterns of Clavicle Fracture
Medial Physeal Separation
Medial clavicular fractures or fracture dislocations are often medial physeal separations, even in young adulthood as closures of the medial clavicular physis can occur as late as age 25 years.
This fracture is classified by Craig as the Group III, Type IV injury. The diagnosis should be considered in any medial injury in a patient less than age 25 years. Most of the injuries are treated in a nonoperative manner.
Surgery is indicated for acute vascular or laryngeal compromise.
Periosteal Sleeve Fractures [Group II, Type IV Craig Injury]
Distal clavicle can become separated from its periosteal sleeve. The injury is also called pseudodislocation of the acromioclavicular joint.
Most of these injuries are treated with nonoperative methods but closed reduction and closed reduction and pinning were performed for severely displaced injuries.
Midshaft Fractures with AC Separation
Middle third clavicle fracture with concomitant acromioclavicular separation are infrequent and have been treated by both nonsurgical and surgical methods.
Floating shoulder
Floating shoulder is used when an injury occurs both in clavicle and neck of glenoid.
Complications of Clavicle Fracture
Soft Tissue Compromise
Because of the subcutaneous position of the clavicle bone, abrasions, bump or tenting is commonly seen. Sometimes skin may be pierced by the fracture spike resulting in an open fracture. Other times the skin may intact be under pressure from the spike and if not attended to would be compromised.
Neurovascular Compromise
In high energy clavicle fractures, brachial plexus injuries may occur. Late brachial plexus lesions have been more commonly seen after clavicle fracture.
Thoracic outlet syndrome has also been reported as a complication of clavicle fracture.
Vascular complications are rarer and more serious.
Hardware Problems
Migration of pins in the aorta, the mediastinum, lung, and around and in the spinal canal have been reported. Plate failure can also occur.
Infection
A rate of infection after operative treatment has been reported as 1.2 to 7.8%.
Wound Problems
Wound dehiscence is a rare problem despite clavicle having minimum tissue over it. If it happens, local adipofascial flap coverage has been described as being successful
Hypertrophic uncosmetic scar after open plating has been reported and is not uncommon. It may require scar excision at the time of plate removal.
Nonunion of clavicle fracture is a complication, especially in type II distal clavicle fracture. Most of the nonunions may are asymptomatic but when symptomatic, it and can cause significant disability. The nonunion rate has been reported to be between 0.1% and 15%.
Nonunion usually describes a fracture that has not adequately healed between 6 and 9 months after injury. Symptoms include pain, paresthesia, and extremity weakness from neurovascular entrapment, shoulder weakness from disturbed shoulder mechanics, crepitation at the fracture site and unacceptable cosmetic appearance.
Nonunion
Clavicle nonunion is defined as lack of evidence of healing 4 to 6 months after injury. The incidence of nonunion has been reported to be between 0.13% and 15% for midshaft fractures and as high as 30% or more for a Type II distal fracture.
Factors Associated with Development of Nonunion of Clavicle Fracture
- Type II fracture
- Shortening or displacement of 2 cm or more
- Severe initial trauma
- Refracture
- Older age
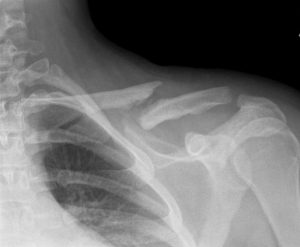
Not all nonunions of the clavicle are symptomatic. Symptomatic nonunion of clavicle fracture should be treated.
Pain at the nonunion site is the most frequent symptom. Static or progressive neurovascular compromise is another indication for surgery.
Reconstructive Procedures for Nonunion of Clavicle
Reconstructive procedures are designed to achieve bone union.
Thes include fixation methods for the treatment of nonunion of clavicle fracture.
Intramedullary pin fixation and Autogenous Bone Grafting
Advantages of intramedullary pinning over other forms of fixation, particularly plate and screw osteosynthesis, include cosmetically acceptable incision, less dissection of the soft tissues, easy removal of the hardware, lesser risk of osteoporosis as it is load sharing device.
However, there is a disadvantage of this technique of lack of rotational control with the pin.
Rush pins, Knowles pin, threaded Steinmann pins have been used for the treatment of nonunion of fracture clavicle with success.
Plate and Screw Osteosynthesis and Autogenous Bone Grafting
Plating and bone grafting is favored over intramedullary fixation for the treatment of nonunion of clavicle fracture for several reasons
- Improved rotational stability
- Ability to incorporate an intercalary graft
- No fear of implant migration
The technique consists of debridement and trimming of the bone ends, placement of a cortical bone transplant posteriorly and metal plate anteriorly, and fixation of the plate to the clavicle and cortical bone transplant with screws.
Disadvantages to plate fixation include the need for wider exposure and increased periosteal stripping, which can disturb the blood supply to the healing fragments. Also, a larger exposure is required for hardware removal.
Free Fibular Vascularized Transfer
For recalcitrant midshaft clavicular nonunions, the use of a free-fibular vascularized graft is a surgical option. This should be used when other fixation techniques fail.
Other Procedures for Nonunion Clavicle
Salvage procedures attempt to alleviate symptoms or deformities without achieving bone union.
- Removing a bony prominence
- Partial or total clavicle removal so that l grating or neurovascular compromise is relieved.