Last Updated on November 12, 2019
Arthritis [Plural – arthritides] means inflammation in joint. The term includes all the causes of joint inflammation which are about hundred in number.
Pain is the most frequent complaint, the pattern of which may differ with arthritis type.
Thought arthritis has many causes, the common outcome is the deterioration of joint surfaces and progressive loss of joint function.
It could occur as a primary disease as in osteoarthritis or it may occur following some other disease such as infection. Former is called primary and latter is secondary arthritis.
Following are common causes of primary or secondary osteoarthritis. Primary is said to occur when the joint is primarily affected.
Secondary osteoarthritis is said to occur when arthritis occurs as a result of the disease that does not primarily affect the joint.
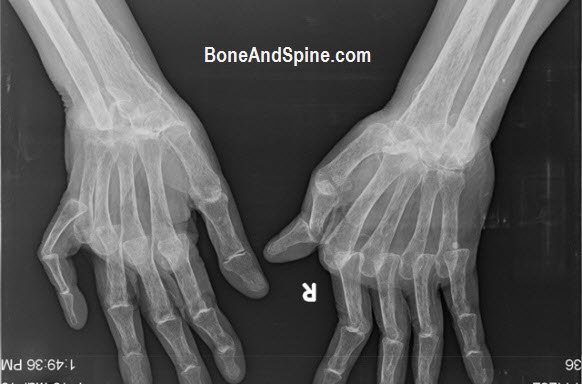
Primary Arthritis:
- Osteoarthritis
- Rheumatoid arthritis
- Septic arthritis
- Gout
- Pseudogout
- Juvenile idiopathic arthritis
- Still’s disease
- Ankylosing spondylitis
Secondary Arthritis:
- Lupus erythematosus
- Henoch-Schönlein purpura
- Psoriatic arthritis
- Reactive arthritis
- Hemochromatosis
- Hepatitis
- Wegener’s granulomatosis (and many other vasculitis syndromes)
- Lyme disease
- Familial Mediterranean fever
- Hyperimmunoglobulinemia D with recurrent fever
- Inflammatory bowel disease.
As such musculoskeletal diseases account for more than 40% of all patients referred for vocational rehabilitation.
Causes
A joint is where one bone moves on another bone and is held by ligaments. The cartilage is the covering on the surface of the bone that articulates with the surface. A joint is covered by a structure called a joint capsule and space within is filled by synovial fluid which is produced by the synovium which lines the joint cavity.
The affection of any structure may lead to joint disease.
The following factors may contribute to higher risk.
- Genetic makeup
- Higher physical demands
- Previous injury to the joint
- Overweight or obese body
- Autoimmune disease.
Common Types of Arthritides
Osteoarthritis
When the cartilage loses its elasticity, it becomes stiff and gets damaged easily and wear off leading to stretch on tendons and ligaments. Eventually, the bones may rub against each other and cause pain.
Rheumatoid
This is inflammatory where the synovial membrane is affected resulting in swelling and pain. It affects more than one joint and is much more common in women than men.
Infectious
It is an infection of the joint caused by bacteria, fungi or viruses.
Juvenile rheumatoid
JRA is a type of arthritis that affects a person aged 16 or less.
Presentation
Pain, swelling, joint stiffness, inability to use the hand or walk, malaise, muscle aches, and pains and joint stiffness are complaints in patients of arthritis.
The presentation of arthritis depends on the type of arthritis. For example, osteoarthritis affects the hips, hands, knees, and spine.
In osteoarthritis, the symptoms develop insidiously and progress with time. The pain in a joint occurs during or after use, or after a period of inactivity. The joint line would be tender and stiffness can be present. The severity of the symptoms increases as time passes. Deformities in the affected joints can occur in the late stage of the disease.
In RA, generally, there is symmetric involvement of joints which are swollen, inflamed, and stiff. The fingers, arms, legs, and wrists are most commonly affected. Symptoms are usually worst on waking up in the morning and the stiffness can last for 30 minutes at this time. Fatigue can be associated with finding.
Infection of the joint presents with fever and swelling of the affected joint. The joint is extremely painful to move. It is more common in children.
Juvenile rheumatoid arthritis patient has intermittent fevers, blotchy rashes on arms and legs and anemia are also common.
The affected joint is swollen and stiff.
Cutaneous nodules, cutaneous vasculitis lesions, lymphadenopathy, edema, ocular inflammation, urethritis, tenosynovitis, Bursitis, diarrhea, and orogenital ulceration are extra-articular manifestations of certain arthritides and should be looked for when relevant.
Lab Investigations
Osteoarthritis generally does not require any laboratory investigation. CBC, ESR, CRP and rheumatoid factor are required in cases of suspected rheumatoid arthritis and juvenile rheumatoid arthritis and infectious arthritis.
Joint aspiration [arthrocentesis] may be required in cases where the diagnosis is not clear-cut.
Imaging
Anteroposterior and lateral views of the involved joint are generally enough. The x-rays help to gauge the joint destruction, suggest the likely cause and differentiate from other causes of joint pain.
X-rays show the destruction of the joint which is depicted by narrowed joint space, osteophytes, osteosclerosis, subchondral cysts, and bone erosions.
MRI and CT may be needed in selected cases.
Treatment
Treatment of arthritis includes drugs, physical therapy, and occupational therapy.
Drugs
Drugs used differ with the type of arthritis. For example, in osteoarthritis, simple analgesics are used and in rheumatoid arthritis drugs for RA are used in addition to analgesics.
NSAIDs
NSAIDs are the most commonly prescribed drugs for arthritis patients. They are potent analgesics but should not be prescribed in people have had a heart attack or stroke, have heart disease, have a peripheral vascular disease, hypertension, hyperlipidemia diabetes, and are regular smokers.
Glucocorticoids
These are steroid drugs which have very high anti-inflammatory action and can be extremely helpful when used properly in selected patients.
Hydroxychloroquine and chloroquine
Used in RA
Sulfasalazine, Methotrexate, Azathioprine
Used in inflammatory arthritis.
Gout medications
In gouty arthritis.
Leflunomide
To treat rheumatoid arthritis and psoriatic arthritis.
Cyclosporine – an immunosuppressant drug, used in combination with methotrexate for RA patients. Although effective, this may be limited by its toxicity.
Diet and Weight Control
This is a very important aspect of management. The patients should avoid foods that cause weight gain.
They should eat plenty of fruit and vegetables, as well as whole grains. Omega-3 essential fatty acids have been shown to relieve some extent the symptoms of rheumatoid arthritis.
Physical Therapy and Occupational Therapy
Physical therapy and occupational therapy help maintain joint mobility and range of motion. Severity and type, age, and the general state of health determine kind of therapy required.
The aim of the physical therapy is to help the patient improve joint stiffness and provide a good range of motion. Physical therapy has been shown to delay the need for surgical intervention in advanced cases.
Occupational therapy helps to manage daily activities so that you put the least strain on the affected joint. This also includes modification of home and workplace, use of splints and aids for activities like dressing, housekeeping, work activities, driving, washing, and bathing, devise a dietary plan if you are overweight or help with decisions like buying the suitable shoe.
Arthritis patients who are physically active generally enjoy better health, are happier, live longer, experience improvements in pain, sleep, day-to-day functioning, and general energy levels.
Local Therapy
It is also important to give intermittent rest to the affected joints.
Local pain can be relieved with ice packs or heating pads.
Local analgesic gels are effective in relieving pain.
Surgery
Joint replacement or arthrodesis may be needed in some cases to relieve the pain.