Last Updated on December 31, 2023
Also called atlantoaxial rotatory fixation, atlantoaxial rotatory subluxation is a condition where there is a fixed rotation of C1 over C2. This condition occurs when normal motion between the atlas and axis becomes limited or fixed spontaneously or following minor trauma [which is usually the case]. It can also or follow an upper respiratory tract infection.
The cause of this subluxation is not completely understood. It is related to increased laxity of ligaments and capsular structures caused by inflammation or trauma.
Atlantoaxial Rotatory Displacement is a pediatric cervical spine rotatory instability and a common cause of childhood torticollis. Both the subluxation and torticollis usually are temporary. but rarely they persist and become atlantoaxial rotatory fixation.
Relevant Anatomy
The occipitoatlantoaxial joints provide stability and mobility to the head. The occipitoatlantal joint offers stability and the atlantoaxial joint is the center for mobility. The stability of these joints by
- Odontoid process and its supporting ligament
- Transverse ligament
- Limits anterior translation of the atlas
- Alar ligaments and apical ligaments
- Limit rotation
- The left alar ligament limits rotation of C1 to right and the right one limits to the left
Classification of Atlantoaxial Rotatory Subluxation
[Fielding and Hawkins]
- Type I: Simple rotatory displacement without anterior shift of C1. There is a unilateral facet subluxation with the intact transverse ligament. The odontoid acts as a pivot point with one facet subluxating anteriorly, and the other facet subluxating posteriorly. Type I is the most common type. It also is the most benign.
- Type II: Rotatory displacement with an anterior displacement of C1 on C2 of 5 mm or less. It is a unilateral facet dislocation and injury to the transverse ligament. One facet acts as a pivot point and one lateral mass is displaced anteriorly
- Type III: Rotatory displacement with an anterior shift of C1 on C2 greater than 5 mm. There is bilateral anterior facet displacement along with both lateral masses. Carriers higher risk of neurological injuries.
- Type IV: Rotatory displacement with a posterior displacement of the atlas (C1). There could be odontoid fracture, or hypoplastic dens present. It is rare. Carries the highest risk of neurological injury and death.
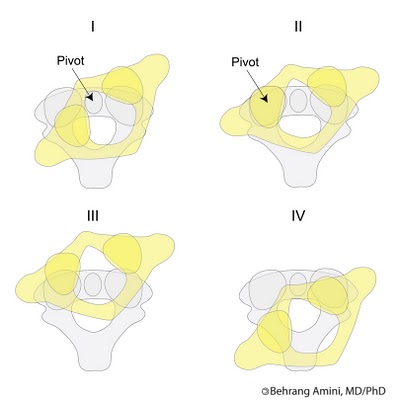
Type I atlantoaxial rotatory subluxation is the most common and occurs primarily in children. Type II atlantoaxial rotatory subluxation is less common but carries a higher risk for neurological damage.
[Goel and Shah’s classification]
- Rotatory locking: Results in torticollis
- Translatory dislocation: Facets of the atlas on both sides were dislocated anterior, resulted in a fixed flexion neck deformity
Causes of Atlantoaxial Rotatory Subluxation
Trauma or infection has been implicated as the most possible pathogenetic factor. Other factors considered are impingement of fragments of the articular capsule or ligaments. Weakness of muscles in the elderly and shallow design of the facets in the children are also thought to contribute.
Many conditions have been associated with atlantoaxial rotatory subluxation. These are rheumatoid arthritis, Down syndrome, Morquio disease, and various congenital cervical anomalies.
The major causes of the condition are listed below.
- Infection
- Trauma
- recent head or neck surgery
- Idiopathic
- Tumors
- Congenital abnormalities
Presentation of Atlantoaxial Rotatory Subluxation
The child usually presents with torticollis following trauma or upper respiratory tract infection. The sternocleidomastoid muscle on the side opposite to the tilt is in spasm as there is an attempt to correct this deformity. Head movements may cause pain in acute situations.
When the subluxation is acute, attempts to move the head cause pain.
With time, the deformity persists as the muscle spasms subside, and the torticollis becomes less painful. A neurological examination should be carried out to find compression.
Other symptoms of atlantoaxial rotatory subluxation are
- Cock-robin head position (Head rotated to one side and tilted to the opposite side
- Pain in the neck
- Spasm in the sternocleidomastoid muscle on the rotation of the chin
- Decreased cervical range of motion
Imaging
X-rays
Anteroposterior, lateral, and open-mouth odontoid views of the cervical spine should be done.
In the anteroposterior and open-mouth odontoid view, the asymmetric distance between the lateral mass and dens is a common finding. The lateral mass that is rotated forward appears wider and closer to the midline, and the opposite lateral mass appears narrower and further away from the midline. Apparent overlapping may obscure one of the facet joints of the atlas and axis.
On the lateral view, the anteriorly rotated lateral mass appears wedge-shaped in front of the odontoid. The posterior arch of the atlas may appear to be assimilated into the occiput because of the head tilt.
Flexion and extension views in the lateral position are done to find atlantoaxial instability.
CT
CT reveals the deformity better and CT with the head rotated as far to the left and right as possible can confirm the loss of normal rotation at the atlantoaxial joint.
This loss of normal rotation at the atlantoaxial joint confirms the diagnosis of rotatory subluxation.
Dynamic CT
Dynamic CT with bilateral maximal rotation imaging may be done for better assessment. Dynamic CT is considered as diagnostic gold standard. It is taken with the head straight forward, and then in maximal rotation to the right and left.
A fixed rotation of C1 on C2 which does not change with dynamic rotation
MRI
Though routinely MRI does not provide any further information MRI can provide soft tissue and neural details better. Therefore MRI can evaluate better
- Spinal cord compression
- Any disruption of the transverse atlantal ligament
- Bony or soft-tissue infection
Treatment of Atlantoaxial Rotatory Subluxation
Non-Operative Treatment
Nonoperative treatment should be used only if no significant anterior displacement or instability is seen on radiographic evaluation.
- Duration less than 1 week, immobilization in a soft collar, analgesics, and bed rest for 1 week. If reduction does not occur spontaneously, hospitalization and traction are indicated
- Longer than 1 week, hospitalization and cervical traction [Head-halter traction but if duration > 1 month, skeletal traction] may be required. Traction is maintained until the deformity corrects, then a cervical collar is worn for 4 to 6 weeks.
Operative Treatment
Operative treatment is indicated in the following situations
- Neurological involvement
- Anterior displacement
- Failure to achieve and maintain correction and deformity > 3 months
- Recurrence of the deformity after an adequate trial of conservative management
A preoperative traction for 2 to 3 weeks to correct the deformity is recommended as much as possible.
C1-C2 open reduction and posterior fusion are carried out with the head in a neutral position. Six weeks of traction/ immobilization after surgery is recommended to maintain correction while the fusion becomes solid. Immobilization is continued until there is radiographic evidence of fusion.
References
- Horsfall HL, Gharooni AA, Al-Mousa A, et al. Traumatic atlantoaxial rotatory subluxation in adults – A case report and literature review. Surg Neurol Int 2020;11:376. [Link]
- Kinon MD, Nasser R, Nakhla J, et al. Atlantoaxial Rotatory Subluxation: A Review for the Pediatric Emergency Physician. Pediatr Emerg Care 2016;32:710-6. [Link]
Image Credit: Behrang Amini