Last Updated on April 30, 2022
Malunion and nonunion are complications of fracture treatment. Nonunion of fracture is a delayed complication of fracture. Literally, it means the absence of a union. But by definition, a bone can be labeled as in nonunion only when the union has not occurred in the bone even after a passage of sufficient time [in which the bone normally would have united].
Fractures of the shaft of long bone should not be considered nonunion until at least 6 months post-injury but in contrast, a central fracture even after 3 months.
After the fracture has occurred, the body initiates a complex overlapping sequence of events, including inflammation, repair, and remodeling.
This sequence can restore the normal bone structure, biologic function, and mechanical strength in patients of any age.
Despite the potential for a successful hearing through regeneration of normal bone, certain types of bone injury and, in some instances, the treatment of bone or soft tissue injury, lead to complications such as delayed union, nonunion, malunion, or bone necrosis that prevent the timely healing.
These complications of fractures and their treatment are inevitable in some patients, but it is possible to avoid or minimize complications, and becomes important to diagnose and treat them.
Definitions
[More about fracture healing and factors affecting it]
The concepts of slow union delayed union, and nonunion are based primarily on the state of activity and rate of progression of the repair process.
Slow Union
This term basically implies that fracture union is present but slow.
A slow union does not result necessarily in a delayed union or nonunion. Such fractures often unite if immobilization is maintained long enough.
Delayed Union
The term delayed union refers to a fracture in which repair is not complete within the interval expected for that specific fracture.
A delayed union, if given a proper milieu, has the potential to unite.
Nonunion
A nonunion exists when repair is not complete within the period expected for a specific fracture, and cellular repair activity at the fracture site ceases.
Clinically, it is diagnosed when a repair process has stopped completely and the union will not occur without therapeutic intervention.
This cessation of activity is the most important feature that differentiates between non and slow/delayed union.
In an established nonunion, sclerosis develops around the bone ends and the medullary canals are sealed off. The bone ends are joined by dense fibrous tissue.
For a fracture of the shaft of a long bone in an adult, at least 6 months must elapse after the injury before this diagnosis can be made.
Once nonunion has occurred, the fracture would not unite without intervention.
How Important are Time Frames?
The terms slow union, delayed union, and nonunion all imply a time frame. This time frame depends on the factors that influence the rate of fracture healing, including the location of the fracture and the amount of soft tissue injury.
However, time elapsed since the injury was used in classical definitions and was important for defining surgical indications.
In the past, surgery was done only in cases where all possibility of healing without intervention was nil.
But with changing times, a more aggressive approach to obtaining fracture union often is taken, and the time frames are less important.
For example, surgery may be contemplated after 4 months of conservative treatment, although technically this does not meet the criteria for a nonunion.
Similarly, fractures that carry a high risk for nonunion may be grafted primarily. This is mainly done in open fractures and comminuted fractures.
From hereon, the main topic of discussion will be nonunion
What Causes Nonunion?
There are multiple factors responsible for the development of nonunion and all the factors responsible for the event may not be known.
Following adverse mechanical factors influence the development of nonunion
- Excess motion
- Inappropriate stabilization
- Large interfragmentary gap
- dIstraction by internal fixation or traction
- The interposition of soft tissues
- Loss of bone
- Loss of blood supply.
- High-energy causes loss of the bony soft tissue envelope
- Damage to nutrient vessels
- Segmental or comminuted free fragments
- Excessive periosteal stripping during hardware insertion.
Some bones like the scaphoid, distal tibia, and the base of the 5th metatarsal are at higher risk for nonunion due to the precarious blood supply in these areas.
Fracture patterns like segmental fractures and those with butterfly fragments are at increased risk of nonunion as the blood supply is compromised to the broken fragment.
There is a long list of causes. Few of them are modifiable and others are not.
- Older age
- Poor nutrition
- Steroid therapy
- Radiation therapy
- Anticoagulant therapy
- Smoking
- High alcohol intake
- Open injuries
- Soft tissue interposition
- Bone loss resulting in a gap
- Compromised blood supply following an injury to the nutrient artery
- Stripping injury to muscle and periosteum
- Severe comminution
- Infection
- Inadequate immobilization
- The distraction of fragments from traction or internal fixation
- Malposition of fragments
- Implant failure
Types of Nonunion
Hypertrophic nonunion
A callus is formed, but the bone fractures have not joined. This can be due to inadequate fixation of the fracture or inadequate mobilization is capable of a healing response to injury.
A radionuclide will show an increased uptake signifying healing activity.
A hypertrophic callus is a sign of motion and the union will occur rapidly when motion is stopped by stable internal or external fixation devices. A bone graft usually is unnecessary.
Oligotrophic nonunion
The callus is absent. It occurs after major displacement of fractures, a distraction of fragments, or internal fixation without correct apposition of fragments.
Blood supply is usually good.
They demonstrate uptake on radionuclide scans but the healing response is inadequate.
Atrophic nonunion
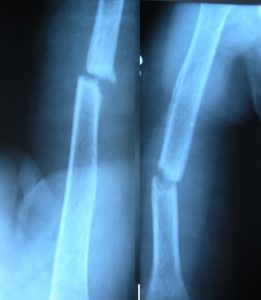
No callus is formed. This is often due to impaired bony healing due to decreased blood supply. They show radionuclide uptake failure.
The bone remains avascular or is revascularized very slowly or poorly.
If alignment is good and there is no gap, then stabilization under compression, with shingling and bone grafting, will stimulate the fracture healing process.
If there is malalignment or a gap, resection of the scar tissue is essential followed by eduction, shingling and stabilization and bone grafting.
Gap nonunion
There is a loss of a fragment of the diaphysis of a bone. The ends of the fragments are viable but as time passes the ends of the fragments become atrophic. Occurs after open fractures, sequestration in osteomyelitis, and resection of tumors.
Pseudarthrosis
The term pseudarthrosis implies a nonunion with false joint formation in which the medullary canal is sealed off, with new cartilaginous surfaces covering the bone ends and the nonunion surrounded by a fibrous capsule having a synovial lining.
Pseudarthrosis means a false joint.
Diagnosis
Diagnosis is made on clinical examination and x-rays. On clinical examination, the fracture fragments would show relative mobility and there would be an absence of tenderness on the fracture site.
The absence of tenderness differentiates nonunion from a delayed union and denotes the absence of any biological activity.
Xrays would show
- The absence of bone crossing the fracture site (bridging trabeculae)
- Sclerotic fracture edges
- Persistent fracture lines
- No changes toward union on serial x-ray
The presence or absence of callus is not a very reliable finding, especially in cases of rigid fixation.
Treatment
The treatment principle is to augment the healing process by freshening the ends of the bone and bone grafting and providing adequate immobilization.
Some superficial fractures may respond to bone stimulation which may be tried as part of nonoperative treatment. Few selected nonunions may be tried with fracture brace immobilization
Contraindications to non-operative treatments are
- synovial pseudoarthroses
- Nonunions that move
- Greater than 1 cm gap between fracture ends.
Operative Treatment
Typical treatment of nonunion is surgical. Following are the essential steps
- Exposure of the fracture site
- Freshening of sclerotic edges to get a bleeding surface.
- The opening of intramedullary cavities of fragments to facilitate the flow of blood circulation
- Rigid fixation
- Bone grafting to augment bone healing
- External splintage if required.
The approach to different nonunion treatments is as below
- Hypertrophic
- biologically viable bone ends
- It May be treated with internal fixation to provide mechanical stability
- Bone grafting may not be required.
- Oligotrophic/ Atrophic
- It May require biological stimulation along with internal fixation
- Bone graft taken from the autologous iliac crest is the gold standard.
- Infected
- The first step is to control infection
- A staged approach required
- It May require external fixation and debridement till the infection heals
- Usually followed by internal fixation and bone grafting
- Pseudoarthrosis
- Removal of atrophic, non-viable bone ends
- Internal fixation with mechanical stability. Soft tissue coverage procedures may be needed.
Fixation Methods
- Internal Fixation
- Screw Fixation
- May be used as interfragmentary screws along with neutralization plate
- Screw Fixation
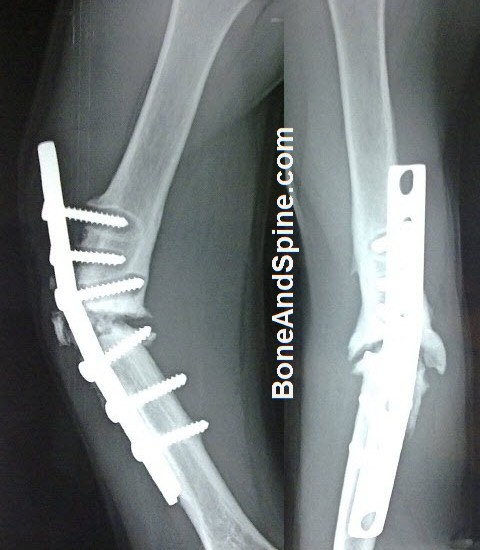
- Plate Fixation
- Plate fixation may be used with or without cancellous bone grafting
- Intramedullary Nailing
- Intramedullary nailing is mainly used for nonunions of the lower limb.
- In open nailing, bone grafting is added.
- External Fixation
- The use depends on the type of nonunion.
- Treatment of bone losses of 3 cm or more may require bone transport with the Ilizarov ring fixator.
- Combined Internal and External Fixation
Bone Grafting
Autogenous bone remains, even today, the best bone grafting material. Bone grafting can be nonvascularized or vascularized.
Bone grafting can be used as an isolated procedure, associated with internal or external fixation.
Depending on the individual case, packing cancellous bone chips in and around the nonunion may suffice, or it may be combined with a structural corticocancellous graft. A nonvascularized segment of the fibula may be used as a graft to fill a large bone defect in the radius or ulna.
Vascularized autografts are effective but require microvascular techniques.
Biophysical Stimulation
- Electrical Bone Stimulators
- Orthobiologics
- Biological substances that are used to help injuries to heal more quickly.
- Autogenous Bone Marrow
- Platelet extract
Infected Nonunions
Infected nonunions become a special case because infection needs to be controlled before the union could occur. Infected non-union is characterized by
- Atrophic radiographic appearance
- Poor fracture vascularisation
- Inadequate soft tissue coverage
- Loose fixation
These require aggressive patient management.
The treatment includes antibiotics, local debridement, stabilization [often external first, followed by internal], repair of the defect to control the infection, soft tissues and bone reconstruction surgeries when needed.
When active drainage is ongoing, healing will be longer and more difficult.
If drainage has not occurred for 3 or more months and the wound is quiescent, the infected may be treated as atrophic .