Last Updated on April 30, 2022
Fractures treatment in modern times allows most of the fractures to heal without a problem. But complications of fractures do occur sometimes which may affect management and outcome.
Complications of fractures can be acute or chronic.
- Acute complications of fractures are mostly due to initial injury and generally as a result of the initial trauma and include neurovascular and soft tissue damage, blood loss and localized contamination and infection.
- Delayed complications of fractures may occur after treatment and may include malunion, embolic complications, infection and loss of function.
Complications of fractures are affected by
- Fracture site
- Fracture pattern
- Type of treatment
- Patient age
- Nutritional status
- Smoking and alcohol use.
Early Complications of Fractures
- Injury to important vessels
- Pneumothorax, Flail chest, and respiratory compromise in case of rib fractures
- Loss of mobility in hip fractures which may result in pneumonia, thromboembolic phenomenon, fat embolism or rhabdomyolysis in elderly
- Vascular injury
- Nerve Injury
- Visceral injury causing damage to structures such as the brain, lung or bladder.
- Compartment syndrome
- Wound Infection
- Fracture Blisters
Late complications of Fractures
- Delayed union, malunion, nonunion
- Joint stiffness
- Contractures
- Myositis ossificans
- Avascular necrosis
- Complex Regional Pain Syndrome
- Osteomyelitis
- Growth disturbance or deformity.
Brief ABout Various Complications of Fractures
Vascular Injury
Vascular injuries, especially arterial injuries may have disastrous consequences resulting in the loss of life and limb. Certain areas are more prone than others due to the location of the vessel. These are
- axilla
- Medial and anterior upper arm
- Antecubital fossa
- Inguinal area
- Medial thigh
- Popliteal fossa
Both in the upper and lower limbs, there is one single vessel at the beginning of the limb which divides into branches after the elbow and just below the knee.
Thus before the furcation or division of the vessel, there is a single vessel supply and after furcation, it becomes two in upper limb and three in the lower limb. This is important because when the injury is to a vessel above elbow or knee, it means loss of entire supply to the limb and thus a risk of loss of limb.
Signs suggestive of vascular injury are
- Active or pulsatile hemorrhage
- Pulsatile or expanding hematoma
- Dusky limb
- Cold limb
- Signs of limb ischemia
- Pallor
- Paresthesias
- Pulse deficit
- Paralysis
- pain on passive extension of the compartment
Doppler ultrasound and arteriography are the investigations that help to ascertain level and type of blood vessel injury.
Arterial Injury is an emergency that needs urgent repair/reconstruction.
Nerve Injury
If the fracture is open, nerve should be explored at the time of debridement. If the wound is clean, the nerve cleanly transected, and the soft tissue bed adequate, primary nerve repair can be done.
Otherwise, nerve ends should be tagged together with sutures to prevent retraction and facilitate later repair.
If the fracture is closed, nerve injury is neuropraxia most of the time. If the fracture is being treated with closed reduction and plaster cast then nothing more needs to be done. This kind of injury generally recovers on its own.
However, if there is an injury occurs while reduction or manipulation, exploration is indicated.
If a fracture is being treated by surgery, it is always prudent to explore the nerve as well.
Visceral Injury
This injury mostly occurs in fractures around the chest, abdomen, and spine. The treatment depends on the part injured and fracture pattern.
Compartment Syndrome
Compartment syndrome is an acute problem following injury or surgery in which increased pressure within a confined space in the limb impairs the blood supply of the limb resulting in ischemia.
Compartment syndrome is a condition caused by increased pressure within a confined space, or compartment, in the body. It mostly is associated with fractures of the tibia, forearm fractures, foot injuries, and hand injuries.
Compartment syndrome results in ischemia of the tissues. If untreated, it can result in necrosis of the muscles and other tissues.
However, rapid diagnosis and treatment can lead to complete recovery.
When a fracture occurs, the force of injury also results in soft tissue injury. Bleeding from the bone or other tissues accumulate in muscle compartments which are limited by fasciae and muscular septae. This causes elevation of the pressure in the compartment and capillary blood flow is compromised.
Ischaemia or decreased tissue perfusion results in edema of the soft tissue which further raises the intra-compartment pressure. Venous and lymphatic drainage of the injured area gets compromised, adding further insult. This further increases the pressure and vicious cycle is formed.
Untreated compartment syndrome mediated ischemia of the muscles and nerves lead to eventual irreversible damage and death of the tissues within the compartment.
Click to see image of the incision for fasciotomy done for compartment syndrome
Characteristics of Compartment syndrome are
- Pain is usually of severe, deep, constant, and poorly localized and is sometimes described as out of proportion with the injury. The pain is aggravated by stretching the muscle group within the compartment and is not relieved by analgesia.
- Paresthesia (altered sensation e.g. “pins & needles”) in the cutaneous nerves of the affected compartment is another typical sign.
Paralysis of the limb is usually a late finding. The compartment may feel very tense and firm as well. - Lack of pulse rarely occurs in patients. and is not a reliable sign. Moreover, it is present in very late stages. Pulse is only affected if the relevant artery is contained within the affected compartment.
Acute compartment syndrome is a medical emergency. It requires opening up of compartments to release pressure. This procedure is called fasciotomy.
Fat Embolism
Fat embolism refers to the passage of fat globules in the lung parenchyma and peripheral circulation. and causing serious consequences resulting in a distinct pattern of clinical symptoms and signs. Fat embolism and related complications of fractures typically occur in long bone fractures of the lower limb.
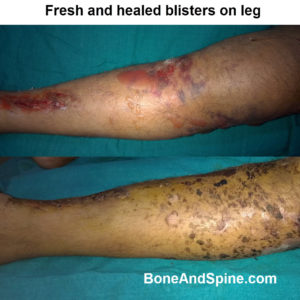
Fracture Blisters
These are relatively uncommon complications of fractures and occur in areas where skin adheres tightly to the bone with little intervening soft tissue cushioning. Examples include the ankle, wrist, elbow, and foot.
Fracture blisters are believed to result from large strains applied to the skin during the initial fracture deformation, and they resemble second-degree burns rather than friction blisters.
Blisters alter management and repair, often necessitating early cast removal and immobilization by bed rest with limb elevation.
Infection
Infection can be a devastating complication of fractures. It occurs in the bone following a fracture by three means
- The fracture is open and the wound gets infected by an organism introduced from without.
- The fracture hematoma can get infected by organisms from the bloodstream.
- Post-surgical infection
Despite all the measures to control it, infection occurs. The incidence is higher in patients with extensive soft tissue injury.
The first goal of the treatment is to prevent the infection. However, if an infection develops it should be controlled.
- If the infection is superficial and limited, local cleaning and antibiotics help. Drainage of pus, debridement of local necrotic tissues, and irrigation of the wound are various local measures that can be used in case of deep infections.
- If internal fixation is in place and the fixation device has not loosened, it should not be removed. The majority of internally fixed fractures unite in spite of infection with antibiotic treatment and drainage.
- If fixation is loose, revising or removing the internal fixation and using external fixation to maintain stability and to allow dressing changes and wound care should be considered.
Uncontrolled infection can lead to septic arthritis and osteomyelitis.
Problems with Bone Healing
A delayed union is a failure of a fracture to consolidate within the expected time. Healing processes are still continuing, but the outcome is uncertain.
Non-union occurs when there are no signs of healing after >3-6 months (depending upon the site of the fracture). Malunion refers to the union of fracture in an unsatisfactory position.
Delayed and Nonunion may be managed conservatively by putting a load on the bone as by weight-bearing in case of lower limbs, bone stimulation by pulsed ultrasonic or electromagnetic or drug treatment, particularly in patients with osteoporosis.
Most of the patients require surgery including fixation and bone grafting or bone graft substitutes.
Myositis ossificans
Myositis ossificans involves calcifications and bony mass formation within the muscle and can occur as a complication of fractures, especially in supracondylar fractures of the humerus. Rest, NSAIDs may be helpful.
Complex Regional Pain Syndrome
Complex regional pain syndrome is a chronic progressive disease characterized by severe pain, swelling, and changes in the skin in the involved region. It can be triggered by injury.
Iatrogenic Complications of Fractures
Iatrogenic complications are the complications caused in the course of the treatment of the issue. In case of fractures, these may include
- Pressure ulcers due to cast
- Thrombophlebitis due to stasis following immobilization or plaster application
- Nerve injury during surgery
- Arterial injury can occur during surgery
- Pin tract infection in external fixation
Synostosis
It is an uncommon complication of fracture and occurs typically in forearm fractures. This leads to the union of both the bones. This complication has been noted in patients who had crushed injury of the forearm or there was an associated head injury.
Results are quite variable.
Concluding Note of Complications of Fractures
Complications of fractures are adverse events following an injury or during the treatment of the injury. In spite of best efforts and treatment options, complications of fractures may occur.
These need to be accepted and managed individually as every patient and injury presents a different challenge.