Last Updated on August 29, 2021
Subtrochanteric fractures are fractures of proximal femur below lesser trochanter. Subtrochanteric region is typically defined as the area from lesser trochanter to 5cm distal to it.
Subtrochanteric fracture is between the lesser trochanter and the isthmus of the femoral shaft. These account for approximately 5% to 34% of all hip fractures.
Fractures with an associated intertrochanteric component may be called intertrochanteric fractures with a subtrochanteric extension or peritrochanteric fractures.
Subtrochanteric fractures are usually high energy fractures seen usually in younger patients.
Low energy subtrochanteric fractures should arouse the suspicion of pathological fractures.
There is also recently identified patient population of individuals experiencing subtrochanteric fractures after bisphosphonate use, particularly alendronate. These have a transverse or short oblique pattern with cortical thickening and a medial cortical beak.
The treatment of subtrochanteric fractures has evolved in recent decades because of a better understanding of both fracture biology and biomechanics, and the availability of better surgical gadgets.
Specially designed implants that can withstand significant muscular forces for prolonged periods of healing are available now and are associated with better surgical outcomes.
Anatomy
The subtrochanteric region of the femur is between the lesser trochanter and a point 5 cm distal. It mainly consists of cortical bone.
Femoral head and neck are anteverted approximately 13º with respect to the plane of the femoral shaft.
The piriformis fossa lies at the base of the neck and is oriented in line with the femoral shaft. It is often the entry point for insertion of femoral nails.
Lesser trochanter is posteromedial. It serves as an insertion point for the psoas and iliacus tendons.
The gluteus medius and minimus tendons attach to the greater trochanter
The deformity in fractures is affected by the major muscles that surround the hip.
Glutei muscles attaching on the greater trochanter abduct the proximal fragment. The psoas and iliacus on the lesser trochanter and flex the proximal fragment. The adductors attach on the shaft and pull the distal fragment medially.
Subtrochanteric fractures are associated with significant hemorrhage. During exposure, profunda femoris vessel is at risk of exposure when the femur is approached from lateral side by splitting or elevating the vastus lateralis off the intermuscular septum close to the large perforating branches of the profunda femoris.
A subtrochanteric fracture is quite slow to consolidate as it heals by cortical healing and is also exposed to high stresses during routine activities significant lateral tensile stresses and medial compressive loads.
Significant compressive forces have been described in the calcar region which result in dense bone in this region
During normal activities of daily living, up to six times the body weight is transmitted across the subtrochanteric region of the femur.
[Read detailed anatomy of femur]
Biomechanics of Subtrochanteric Fractures
The subtrochanteric region is the site of very high mechanical stresses; the medical and posteromedial cortices are subject to high compressive forces, whereas the lateral cortex experiences high tensile forces.
Furthermore, the cortical bone in the subtrochanteric region is less vascular, therefore, the risk of healing complications is greater.
Due to attached muscle forces, certain characteristic deformity patterns arise after subtrochanteric fracture.
The proximal fragment may be flexed, abducted, and externally rotated secondary to the forces exerted by the iliopsoas muscle, the gluteus medius and minimus muscles, and the short external rotators.
The gluteus medius and minimus muscle abduct the proximal fragment through their attachment onto the greater trochanter.
The iliopsoas muscle flexes and externally rotates the proximal fragment if the lesser trochanter is attached.
The short external rotators externally rotate the proximal fragment.
The adductors and hamstrings cause shortening and adduction of the distal fragment.
Most of the subtrochanteric fractures occur because of complex loading patterns.
Nevertheless, there are specific loading patterns that produce characteristic fractures;
Pure Bending
The convex side of the femur is loaded in tension and the concave side in compression. The side subjected to tension fails and results in a transverse fracture.
Bending with axial compression
Bending produces a transverse fracture line on the convex side and axial compression converts the transverse fracture to on oblique fracture pattern on the concave side of the loaded bone resulting in a butterfly fragment.
Pure Torsion
Results in a spiral fracture with the fracture.
Low- energy trauma usually results in a minimally comminuted oblique or spiral fracture but fractures from high-energy trauma are often comminuted
Mechanism of Injury
In younger individuals, these subtrochanteric fractures result from a high-energy trauma.
- Motor vehicle accident
- Fall from a height
- Penetrating injury like a gunshot wound
In elderly persons, they are more commonly secondary to low-energy trauma.
Pathological fractures are another reason for subtrochanteric fractures.
In low-energy trauma, significant associated injuries are unusual. Patients who sustain a high-energy subtrochanteric fracture had other injuries to the long bones, pelvis, spine or abdominal organs.
Classification of Subtrochanteric Fractures
Russel-Taylor Classification

Type I
These fractures do not involve the piriformis fossa. They are subdivided into subtypes
1A
Fractures below the lesser trochanter
1B
Fractures involving the lesser trochanter
Type 2
Fractures involve the piriformis fossa.
2A
fractures have a stable medial buttress
2B
has no stability of the medial femoral cortex. These fractures may have varying degrees of proximal comminution, sometimes with extension into the femoral neck, and may present difficulty with implant choice.
Seinsheimer Classification

It is based on the fracture pattern of the proximal femoral shaft.
I
less than 2mm displacement
II
A
2-part transverse fracture
B
2-part spiral fracture with lesser trochanter attached to the proximal fragment
C
2-part spiral fracture with lesser trochanter attached to the distal fragment
III
A
3-part spiral fracture with lesser trochanter as a separate fragment
B
3-part spiral fracture with butterfly fragment
IV
Comminuted fracture with 4 or more fragments
V
Fracture with proximal extension into the greater trochanter
AO/OTA Classification
32-A3.1
Simple (A), Transverse (3), Subtrochanteric fracture (0.1)
32-B3.1
Wedge (B), Fragmented (3), Subtrochanteric fracture (0.1)
32-C1.1
Complex (C), Spiral (1), Subtrochanteric fracture (0.1)
Causes of Subtrochanteric Fractures
- High Energy Trauma
- Younger patients
- Motor vehicle accident
- Fall from height
- Gunshot wounds [10% of high-energy subtrochanteric femur fractures]
- Iatrogenic fractures
- Stress following previous surgery on the proximal femur
- Seen in arthroplasties
- Minor slips in elderly
- Pathological fractures
Clinical Presentation
Pain at the injured site, swelling, and deformity of the affected limb including shortening is the usual presentation. Physical findings at the time of injury often include a shortened extremity on the fractured side.
Tenderness to palpation in the proximal thigh region is present. The leg may lie in internal or external rotation. The patient should be monitored for vital signs as significant hemorrhage can cause systemic shock and compartment syndrome.
In high-energy fractures, associated injuries to the cranium, thorax, and abdomen, pelvis, spine, and other long bones should be looked for common, especially on the ipsilateral side.
Imaging
X-rays
- Full-length anteroposterior (AP) views of the femur from the hip to the knee should be obtained.
- Cross-table lateral view of the hip allows
- AP view of the pelvis
X-rays are able to tell about fracture pattern and ipsilateral injuries which can affect the treatment decision.
Pathological nature of fractures can be noted.
Bisphosphonate-related fractures are characterized by
- Lateral cortical thickening
- Transverse fracture orientation
- Medial spike
- Lack of comminution
Computed Tomography
Not generally required for diagnosis or treatment planning.
MRI
Indicated in pathological fractures
Treatment of Subtrochanteric Fractures
Approach Considerations
In modern orthopedics, the treatment of subtrochanteric fractures in adults is almost exclusively surgical.
Indications for surgical treatment are
- Displaced and nondisplaced fractures in adults
- Fractures in patients with multiple traumatic injuries
- Open fractures
- Severe ipsilateral extremity injuries
- Pathologic fractures
However, in selected patients where fractures who are medically unstable for surgical intervention, treatment with skeletal traction can be considered.
In children, traction followed by cast bracing is an accepted treatment option.
Therefore, nonsurgical treatment protocols are of historic interest.
If surgery is anticipated within 24 hours of admission, one can place a pillow under the knee of the injured extremity or apply Buck’s skin traction.
If there is a longer delay, a distal femoral or proximal tibial pin should be inserted to maintain reasonable fracture alignment and length and prevent addition soft tissue injury from displaced fracture fragments.
Surgical Therapy
Surgical treatment can be divided into the following three main techniques:
- External fixation
- Open reduction with plates and screws
- Intramedullary fixation
External Fixation
External fixation is indicated in severe open fractures. It is done rarely. It is often temporary, and after healing, converted to internal fixation.

Open reduction with plates and screws
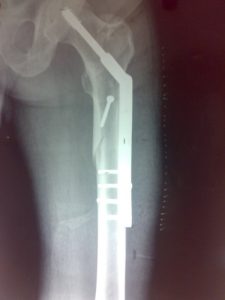
Following choices are available
- Sliding hip screw or dynamic hip screw [DHS]
- Dynamic condylar screw
- Anatomically contoured locking plates
Intramedullary Fixation
These are fast emerging as the treatment of choice for subtrochanteric fractures.
Two types of nails are in use
- Centromedullary – These are contained within the medullary canal without involving the neck and head of the femur
- Cephalomedullary – These nails are affixed to the femoral neck and head
Fractures with large fragments and have limited comminution can be treated with reduction, lag screw fixation of fragments and plate neutralization.
But, in the presence of severe comminution, indirect reduction and minimally invasive bridge plating techniques are better.
Primary bone grafting may be needed in comminuted fractures and open fractures
With plate fixation, weight-bearing is not allowed till enough bone union has occurred. In stable fixations, minimal protected weight-bearing can begin immediately but is advanced slowly. After intramedullary nailing, if bone quality and cortical contact are adequate, 50% partial weight-bearing can be allowed immediately.
Complications
Loss of fixation
With the sliding hip screws, implant failure usually occurs secondary to screw cutout from the femoral head and neck, in patients with osteoporotic bone.
Fixation failure may be clinically evident as progressive deformity and limb length inequality associated with thigh pain.
Loss of fixation with use of interlocked nails is commonly related to
- Failure to statically lock the device
- Comminution of the entry portal
- Use of thinner nails
Failure of fixation is addressed by removal of hardware, revision internal fixation, and bone grafting.
Nonunion
Patient’s inability to resume full weight bearing within 3 to 6 months indicate non-union.
It may be confirmed by radiographs and /or tomograms.
It is often seen that nonunion usually persists in the femoral shaft portion of the fracture which is best treated with an interlocked nail and autologous bone grafting.
Malunion
Limp, leg length discrepancy or rotational deformity are signs of malunion. The affected leg should be compared to the opposite side for deformity evaluation.
The femoral neck-shaft angle must be resorted, otherwise, the patient will have a Trendelenburg gait [lurching to affected side] with abductor weakness secondary to shortening of the abductor muscle group.
A valgus osteotomy and revision internal fixation with bone grafting is the treatment of choice for a varus malreduction.
If significant internal or external rotational deformities are detected, revision surgery with derotation osteotomy may be indicated.
Infection
Acute infection may become evident within the first and second weeks after surgery by increasing pain associated with the usual signs inflammation. A nonunion should also be assessed for infection before revision is contemplated.
Acute postoperative infection is best managed by immediate surgery for drainage and debridement of all necrotic material followed by antibiotics.
References
- Senter B, Kendig R, Savoie FH. Operative stabilization of subtrochanteric fractures of the femur. J Orthop Trauma. 1990. 4(4):399-405.
- Boyd AD, Wilber JH. Patterns and complications of femur fractures below the hip in patients over 65 years of age. J Orthop Trauma. 1992. 6(2):167-74.
- Nieves JW, Bilezikian JP, Lane JM, Einhorn TA, Wang Y, Steinbuch M, et al. Fragility fractures of the hip and femur: incidence and patient characteristics. Osteoporos Int. 2009 May 30.
- Kloen P, Rubel IF, Lyden JP, Helfet DL. Subtrochanteric fracture after cannulated screw fixation of femoral neck fractures: A report of four cases. J Orthop Trauma. 2003. 17:225-233.
- Waddell JP. Subtrochanteric fractures of the femur: a review of 130 patients. J Trauma. 1979 Aug. 19(8):582-92.
- Craig NJ, Maffulli N. Subtrochanteric fractures: current management options. Disabil Rehabil. 2005 Sep 30-Oct 15. 27 (18-19):1181-90.
- Sanders R, Regazzoni P. Treatment of subtrochanteric femur fractures using the dynamic condylar screw. J Orthop Trauma. 1989. 3(3):206-13.
- Vaidya SV, Dholakia DB, Chatterjee A. The use of a dynamic condylar screw and biological reduction techniques for subtrochanteric femur fracture. Injury. 2003 Feb. 34(2):123-8.
- Queally JM, Harris E, Handoll HH, Parker MJ. Intramedullary nails for extracapsular hip fractures in adults. Cochrane Database Syst Rev. 2014 Sep 12. CD004961.