Last Updated on October 28, 2023
Serratus anterior paralysis is a condition that characterized by pain, loss of shoulder movement and winging of scapula owing to damage or injury of the long thoracic nerve.
This nerve evolves from the roots of neck vertebrae (C5-C7) and supplies to serratus anterior muscle that retains the scapula bone to the chest wall.
Long thoracic nerve is more prone to injury due to its excessive length. Usually, injury to this nerve occurs due to trauma, repetitive injury or iatrogenic causes.
Anatomy and Function of Serratus Anterior Muscle
Serratus anterior muscle originates from superior lateral surfaces of upper 8 or 9 ribs at the side of the chest.
It inserts on to the costal surface of the vertebral border along the inferior angle of the scapula.
Serratus anterior muscle is supplied by long thoracic nerve [C5, C6 and C7].
It functions to draw scapula forward, abducts scapula and rotates it to point glenoid cavity superior. It also stabilizes vertebral border of the scapula to thoracic cage, along with rhomboids and middle trapezius.
The muscle is supplied by the long thoracic nerve which is formed by joining of ventral rami of, C5, C6, C7 and passes under the clavicle to the thorax to supply serratus anterior muscle.
Blood supply of the muscle is by the circumflex scapular artery, which emerges at the lateral border of the scapula and divides into cutaneous scapular & periscapular arteries.
Function of Serratus Anterior
The main function of the serratus anterior muscle is to position the glenoid so that upper limb could be placed in position for efficient energy use.
The plane of the scapular position at rest is parallel to that of the posterior thoracic wall.
Within this plane, the scapula can translate (move in a straight line) in four directions leading to all gliding movements of the scapula across the posterior thoracic wall. These movements are named elevation, depression, retraction, and protraction are
- The elevation is upward movement
- Depression is downward movement
- Retraction or adduction is the movement that It brings the medial scapular border is closer to the spine
- Protraction or Abduction is the movement that causes the scapula to translate away from the spine
All of these motions occur essentially within the same plane.
The combination of movements is responsible for rotator scapular motion.
There are two other movements of the scapula that occur perpendicular to the plane of rest.
These are anterior tilting and posterior tilting.
Contraction of the serratus anterior is responsible for protraction and upward rotation of scapula and contributing to the abduction of the shoulder by increasing the angle of humeral elevation.
The serratus anterior is more active in forward flexion than pure abduction, as abduction requires some retraction of the scapula as well which is a function of the trapezius muscle. [A smooth scapulothoracic motion requires synergy between serratus anterior and trapezius]
When upward rotation and protraction of the scapula is absent due to non-functioning by the serratus anterior, full glenohumeral elevation is not possible.
Read more on Scapulohumeral Rythm
Details of Scapular Motion
Contraction of the serratus anterior initiates scapular lateral rotation. With the lateral movement of the scapula, the lower fibers of the trapezius fire to resist displacement.
The synergistic activity of these two muscles changes the center of scapular rotation from the root of the scapular spine to the deltoid tubercle.
This allows participation of the upper trapezius fibers, which then assist in lateral rotation of the scapula.
In a complete paralysis of the serratus anterior, abduction is limited to 110°
Causes of Serratus Anterior Paralysis
Causes of serratus anterior paralysis are well explained by the anatomy of the long thoracic nerve and its relationship to the serratus anterior.
The long thoracic nerve is a unique nerve in that it arises directly from the spinal nerve roots, has no sensory fibers, and supplies a single muscle.
As the course of the nerve is long, the affection of the nerve anywhere would result in paralysis of serratus anterior muscle.
Causes of Long Thoracic Nerve Palsy are
Non-traumatic and idiopathic Lesions
- Viral illness
- Influenza
- Tonsillitis-bronchitis
- Poliomyelitis
- Allergic-drug reactions
- Toxic exposure
- Herbicides
- Tetanus antitoxin
- Muscular dystrophy-facioscapulohumeral dystrophy
- C7 radiculopathy
- Aortic coarctation
Blunt Trauma
- Sudden depression of the shoulder girdle
- Unusual twisting of the neck and shoulder
Repetitive Injuries
- Athletics
- House-hold activities
- Hedge-clipping
- Digging
- Car washing
Iatrogenic
- Chiropractic manipulation
- Injury during Surgery
- Mastectomies with axillary node dissection
- Scalenotomies
- Surgical treatment of spontaneous pneumothorax
Miscellaneous
- Post-general anesthesia for various clinical reasons
- Electrical shock may also cause long thoracic nerve palsy
- Use of a single axillary crutch
Most of the chronic nerve compression may be caused by compression at following sites
- Scalene muscles
- Subcoracoid
- Between coracoid and 1st or 2nd rib
- Often due to carrying heavy objects on the shoulder
- Inflamed bursae
- Subcoracoid
- Subscapular
- Supracoracoid)
- Anteroinferior scapular border
Clinical Presentation of Serratus Anterior Paralysis
The patient presents with ill-defined, nonspecific shoulder girdle pain and fatigue of muscles of the base of neck, scapula, and deltoid. Muscle spasms may be present.
The symptoms are more prominent with repetitive motions involving forward flexion (such as push-ups).
There may be a complaint of weakness may be notable with prolonged activity like as carrying heavy weights.
Overhead activity is associated with worsening of the shoulder pain.
Tilting of the head to opposite side with arm elevation may exacerbate symptoms.
The patient may complain about shoulder being unstable.
Pain is most noticeable in muscles that oppose serratus anterior like rhomboids and levator scapulae. This is because the muscles suffer unopposed contraction.
Those involved in sports may report a loss of throwing power. The at, however, may continue the sports as the pain is not severe enough.
There might be a complaint of scapular protuberance which may be noticed especially when the patient sits in a high back chair.
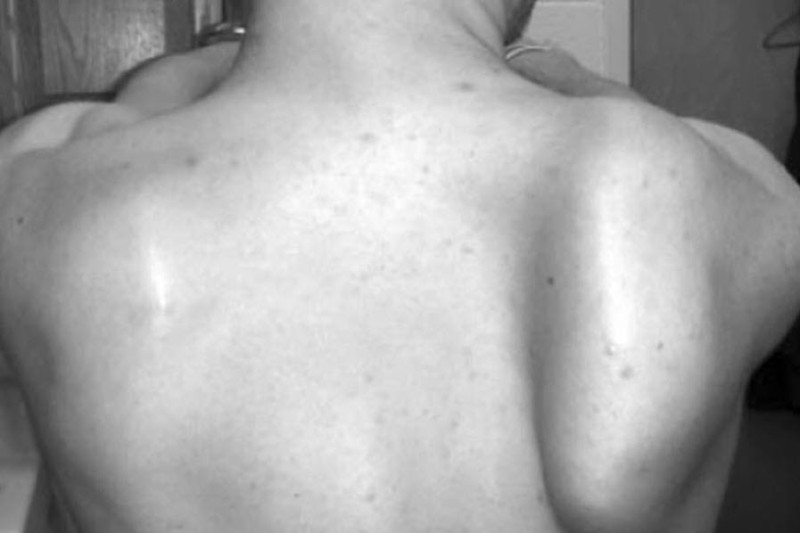
The examination would reveal wasting of the muscle and a winged scapula. Scapular movements may be asymmetrical and appear uncoordinated.
A relative weakness in forward flexion compared to the opposite arm is seen.
Winging of the scapula is suggested by the prominence of the inferior and medial borders of the scapula when the arms are in forward flexion. In subtle cases, activity, like pushing the wall or push-ups, may reveal the deformity.
Scapular stabilization manually improves manual stabilization of the scapula often improves pain.
Differential Diagnoses
- Rotator cuff tear
- Trapezius palsy
- Impingement syndrome
- Acromioclavicular joint disease
- Biceps tendonitis
- Suprascapular nerve entrapment
Diagnostic studies
Electromyography helpful in finding the nerve site involved and the type of injury [ neuropraxia or axonal injury]
Treatment of Serratus Anterior Paralysis
Conservative Treatment
When serratus anterior paralysis is from a stretch injury [neuropraxia], conservative treatment is usually preferred, especially initially.
This includes watchful waiting while preventing further injury.
Conservative treatment consists of
- Observation
- Physical therapy
- Activity modification
The observation is for a minimum of 6 months and ideally up to 2 years for the nerve to recover.
The patient should avoid painful or heavy lifting activities.
Physical therapy includes serratus anterior strengthening, stretching and bracing with a modified thoracolumbar brace can be considered.
Majority of patients will spontaneously resolve with full return of shoulder function and resolution of winging by 2 years
Operative Treatment
In lesions where the nerve is transected surgical treatment is preferred.
The treatment options include
Neurolysis of the long thoracic nerve
- Failure to improve with conservative treatment taken at least 6 months
- Electromyography with signs of nerve compression.
Muscle transfer
This is considered when there is a failure to improve with conservative treatment, for 1-2 years and there is no visible nerve compression.
Following transfers can be considered
- Split pectoralis major transfer [most effective]
- Pectoralis minor transfer
- Rhomboid transfer
Abduction weakness usually persists.
Nerve transfer
It is a microsurgery and indications are still developing.
The transfer could be of
- lateral branch of the thoracodorsal nerve to the long thoracic nerve
- medial pectoral nerve with sural nerve graft to the long thoracic nerve
The procedure has been shown to innervate the long thoracic nerve and provides the benefit of muscle preservation.
Scapulothoracic fusion
It is a salvage procedure performed to stabilize the scapula on the thorax. It involves the fusion of the medial border of the scapula to the underlying 3 to 5 ribs, with wire cables and/or plates and screws
It is often the last resort with a goal of pain relief.