Last Updated on September 20, 2020
The triphalangeal thumb is a congenital hand anomaly where the thumb has three phalanges instead of two. The middle phalanx is the extra one.
In the normal human hand, the thumb has two phalanges. It is believed to be first described by Columbo in 1559.
The triphalangeal thumb with full-length normal second phalanx and without duplication resembles a finger; when it does not oppose because the thenar muscles are absent, the hand is referred to as a five finger hand.
Triphalangeal thumb is considered a form of pre-axial polydactyly.
The triphalangeal thumb is a rare condition. It occurs in about one per 25,000 births and can occur as an isolated defect or in association with other hand malformations. The triphalangeal thumb also occurs as a feature of many syndromes such as Holt-Oram syndrome.
The triphalangeal thumb is inherited as an autosomal dominant trait though sporadic cases may occur.
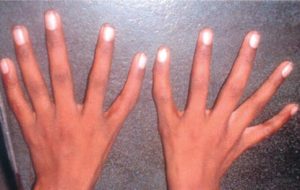
Image Credit: indianpediatrics.net
Pathophysiology
The exact mechanism of the condition is not clear. There is an abnormality of the apical ridge which is a structure formed by the ectodermal cells at the distal end of each limb bud during fetal development. It provides major induction signals during the development of limb for the early growth and differentiation of the limb.
Abnormalities of these inductions can lead to inadequate development. On the preaxial side, these can range from complete thumb aplasia [non-formation] to varying degrees of hypoplasia [abnormal small thumb] to a relatively long triphalangeal thumb lying in the same plane as the fingers.
Thenar eminence The muscle mass making the thenar eminence is also diminished and the palm appears triangular.
There is no sex predilection. In about 87 percent of the cases, involvement is bilateral.
The thumb of the contralateral hand may be normal, absent, or duplicated.
The triphalangeal thumb may also be part of a generalized syndrome.
Isolated triphalangeal thumb anomaly has been mapped to chromosome region 7q36.
Types of Triphalangeal Thumb
Isolated triphalangeal thumbs are of two functional types
- Opposable – Presence of opposition movement of the thumb
- Non-opposable – Opposition movement weak or absent.
Wood described a classification of triphalangeal thumb based on three different shapes of extra phalanx [middle phalanx]
- Wedge
- Trapezoidal
- Rectangular
Buck-Gramcko described a more detailed classification
- I – Rudimentary triphalangism
- II- Short triangular middle phalanx
- III – Trapezoidal middle phalanx (intermediate)
- IV – Long rectangular middle phalanx
- V – Hypoplastic triphalangeal thumb
- VI – Triphalangeal thumb associated with polydactyly
Associated Syndromes and Conditions
Due to its association with many syndromes and defects, the triphalangeal thumb may have one of the following associations. This is not an exclusive list and only major types of associations are written.
- Radial hypoplasia
- Bone marrow dysfunction
- Congenital heart disease
- Lung hypoplasia/agenesis
- Anorectal malformations,
- Hearing loss [Sensorineural type]
- Onychodystrophy [Deformed nails]
- Mental retardation
- Duplication of the hallux or the little toe
- Lobster feet and hands
- Absent tibia
- Absent carpal bones
Following are few of the long list of syndromes which might be associated with triphalangeal thumb
- Triphalangeal thumb- polydactyly syndrome
- Tibial hemimelia-polysyndactyly-triphalangeal thumb syndrome
- Acropectoral syndrome
- Aase syndrome (associated with congenital hypoplastic anemia
- Townes-Brocks syndrome (deafness, anal anomalies)
- Townes-Brocks syndrome [renal dysplasia]
- Laurin-Sandrow syndrome (underdeveloped nasal bones, large heads of mandibular condyles, synostosis of tarsal bones along with polysyndactyly)
- Diamond-Blackfan syndrome [anemia]
- Holt-Oram syndrome
- Poland syndrome
- Trisomy 13
- Trisomy 22
Clinical Presentation
The length of thumb is variable depending on the size of the extra middle phalanx.
The patient may complain of problems arising due to deficient opposition like difficulty with activities like writing, picking up smaller objects. Functionally, fine motor activities such as precision handling are defective.
Thumb may appear like a thumb or like a finger. The first web could be normal or aberrant. The extra phalanx may be delta-shaped, rectangular, or normal. A small trapezoid second phalanx will cause ulnar angulation.
Failure of opposing the thumb indicates the weakness of the thenar muscles and is of variable degree.
There may be hypermobility at the metacarpophalangeal joint. The carpometacarpal joint can be either hypoplastic or malformed or absent.
In the case of duplication of thumbs [two thumbs], the ulnar thumb is usually better formed.
Rarely, triplication of the thumb is seen and all of these thumbs are underdeveloped.
Imaging
Routine x-rays would reveal three phalanges instead of two in the involved thumb.
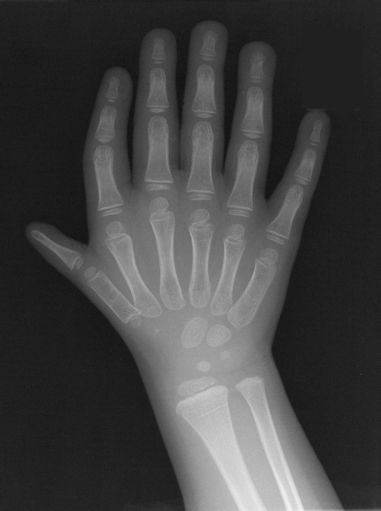
If an extra ray is present, it may be visible as a full ray or with proximally or distally developed parts.
There may be a duplication of a malformed trapezium.
X-rays are good ways to define the shape of the thumb and the status of the whole ray.
Treatment of Triphalangeal Thumb
The parents may seek correction of the deformity for their children because of the appearance of the thumb or associated functional deficit.
The surgery aims at
- Reducing thumb length [Ideally the tip of the thumb should not be longer than the level of the index PIP joint]
- Create a good function
- Stable and non-deviated joint
Surgery is done at the age of one year generally. In a five-fingered hand with only a slight distal deviation there is no need for an early operation and can be delayed to preschool age.
Different surgical options are as follows
- Resection of the extra wedge-shaped phalanx
- Reduction arthrodesis at DIP level (DIPRAD)+ epiphysiodesis at a later stage.
- DIPRAD+corrective osteotomies
- Opposition plasties in five-fingered hand
- By muscle transfers
- Abductor digiti mini most common
- Others are flexor carpi ulnaris and flexor digitorum superficialis to ring finger
In thumb duplication, when a triphalangeal thumb accompanies a normal thumb, the three phalanxed thumb is ablated.
When the accompanying two-phalanx thumb is hypoplastic but functional, again it is best to ablate the triphalangeal thumb.
When both thumbs have three phalanges and hypoplastic, the more functional of the duplicated thumbs is retained.
Treatment is individualized in each case where wound care and exercises for mobilization are instituted.
The complications of surgery are rare.
Minor complications are skin issues, infection, or non-union,
References
- Hovius SER, Zuidam JM, de Wit T. Treatment of the triphalangeal thumb. Tech Hand Upper Extrem Surg. 2004, 8: 247–56.
- Zuidam JM, de Kraker M, Selles RW, Hovius SER. Evaluation of function and appearance of adults with untreated triphalangeal thumbs. J Hand Surg Am. 2010, 35: 1146–52.
- Zuidam JM, Selles RW, de Kraker M, Hovius SE. Outcome of two types of surgical correction of the extra phalanx in triphalangeal thumb: is there a difference? J Hand Surg Eur 2016, 41: 253–7