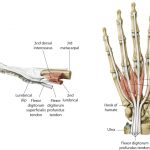
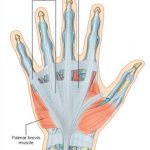
The term dorsal digital expansion refers to the small triangular aponeurosis covering the dorsum of the proximal phalanx with its base at the metacarpophalangeal joint. The main tendon of the extensor digitorum occupies the central part of the expansion and is separated from the metacarpophalangeal joint by a bursa. [Aponeurosis is a flat sheet or […]
Anatomy
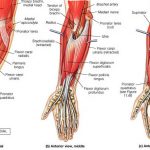
Forearm Muscles – Anatomy and Function
The forearm is the area of upper extremity between the elbow and wrist. The bony structure of the forearm is formed by two bones – radius and ulna. There are twenty forearm muscles which are arranged in two compartments – anterior and posterior. The anterior compartment contains flexor muscles and is also called the flexor […]
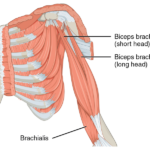
Muscles of Arm- Anatomy and Function
The region between the shoulder joint and the elbow joint is called the upper arm or arm. That between elbow and wrist is called forearm. Brachium and antebrachium are anatomical terms for arm and forearm respectively but are not used that commonly. Muscles of arm can be classified as that of a flexor compartment or […]
Muscles of Shoulder Region
The human shoulder is made up of three bones Clavicle or collarbone Scapula Humerus Glenohumeral joint and acromioclavicular joints are the main joints of the shoulder region. The joints are stabilized by muscles, ligaments and tendons. The shoulder joint is a very mobile joint to allow for a wide range of actions such as lifting, pushing and […]
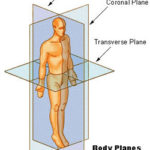
Anatomical Position, Planes and Locations
Anatomical Position of Human Body Anatomical position is the basic premise or central tenet, the very core on which all the details of anatomy are based. Thus, to understand the anatomy of the human body, the anatomical position has always to be remembered. The anatomical position of the human body is The person standing erect […]
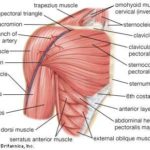
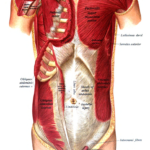
Muscles of Pectoral Region – Anatomy and Clinical Significance
Muscles of pectoral region or pectoral muscles are the muscles that connect the front of the chest to the bones of shoulder and arm. The pectoral region refers to the anterior chest wall. They are commonly called as pecs. These muscles also provide shape to the chest and pectoral exercises are quite famous among bodybuilders. […]
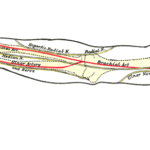
Ulnar Nerve Anatomy, Course and Supply
The ulnar nerve, an extension of the medial cord of the brachial plexus, is a mixed nerve (both motor and sensory) that supplies hand muscles and medial aspect of the skin of the hand. The ulnar nerve and median nerve are responsible for the supply of flexor muscles and skin of the hand. These nerves […]
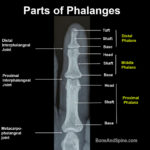
Phalanx of Hand – Anatomy and Function
Phalanx [plural phalanges] is a tubular bone present in hand and foot and form digits [fingers and toes]. In this article, we discuss the phalanges of the hand. There are five digits in each hand – four finger and one thumb. All fingers have three phalanges distal, middle and proximal. Thumb has only proximal and […]
Flexor Retinaculum of Hand and Foot
Flexor retinaculum of hand is a fibrous band that is present in the flexor aspect of wrist and flexor aspect of the ankle. Flexor retinaculum of the hand is also called transverse carpal ligament or anterior annular ligament. It is a strong, fibrous band, that arches over the wrist region and converts the deep groove […]
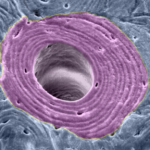
Osteon or Haversian System and Its Significance
The osteon is the basic building block and fundamental functional unit of compact bone. It is also called a Haversian system, named after Clopton Havers, an English physician who worked extensively on the microstructure of the bone. Structurally, osteons are roughly cylindrical structures which are several millimeters long and around 0.2 mm in diameter. Structure […]